HIPAA in the Heavens: Ensuring Secure DHA Cloud Data Sharing

How Secure DHA Cloud Data Sharing Cuts Data Search Time 80% (Or You Keep Wasting Weeks)
Secure dha cloud data sharing is changing how the Defense Health Agency (DHA) delivers care to 9.6 million military beneficiaries. For decades, the Military Health System (MHS) was hindered by extreme fragmentation, with patient data siloed across dozens of legacy platforms. This transition from decentralized facilities to a unified enterprise required a complete overhaul of data storage and protection.
Historically, the MHS operated as a collection of independent hospitals and clinics, each maintaining its own local servers and data protocols. This led to a “digital archipelago” where a service member’s medical history was often trapped within the walls of a single facility. When a soldier moved from Fort Bragg to a base in Germany, their records didn’t always follow them digitally, leading to redundant blood tests, missed allergy warnings, and delayed treatments. The shift to a secure cloud environment isn’t just a technical upgrade; it is a fundamental reimagining of military medicine.
Key highlights of this transformation include:
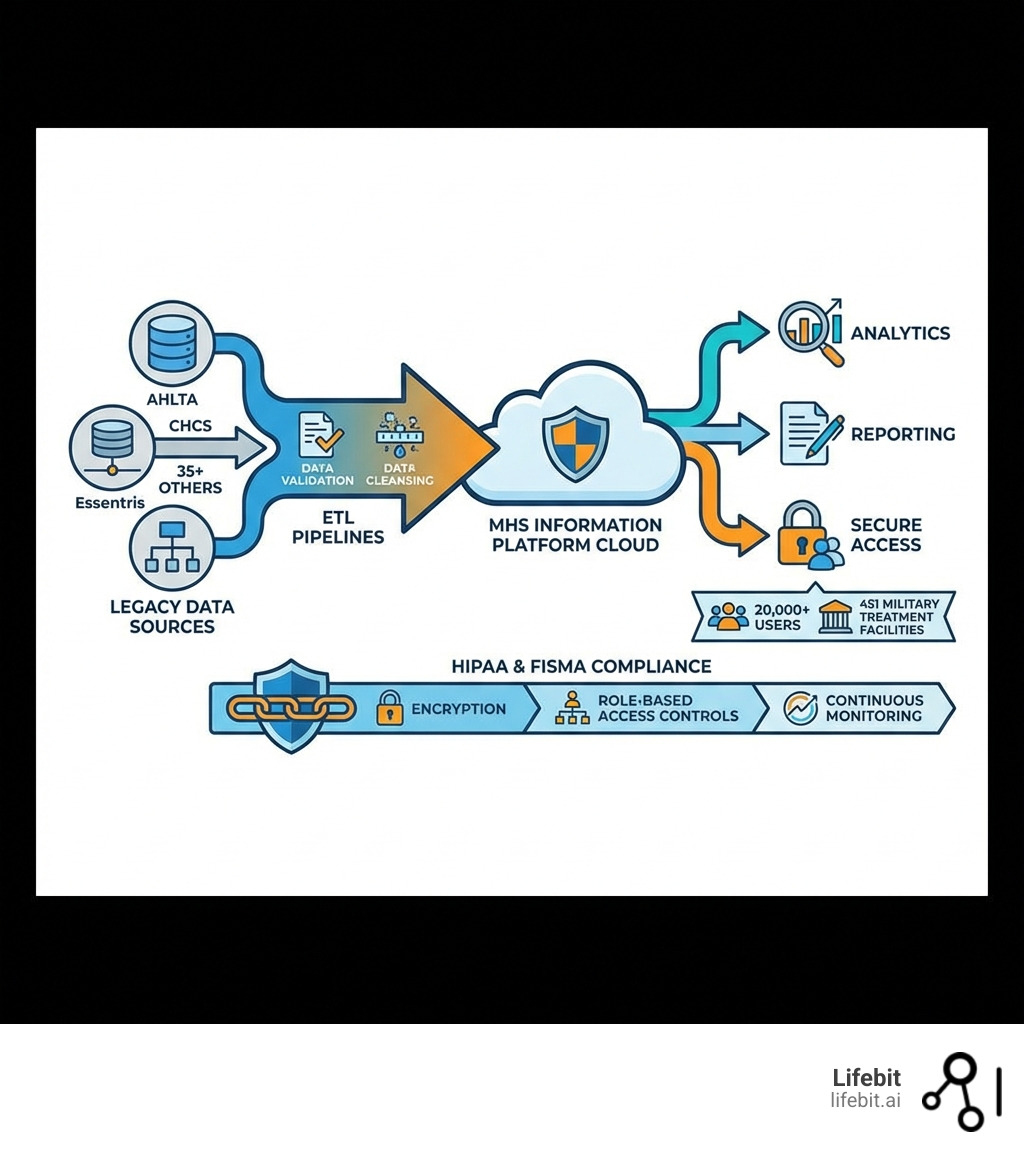
- The Challenge: 30 years of fragmented records across 35+ legacy systems like AHLTA (outpatient), CHCS (administration), and Essentris (inpatient), which were often incompatible and increased medical error risks.
- The Solution: Operation Helios migrated 1 petabyte of data to the MHS Information Platform (MIP), creating a unified cloud environment as the DoD’s single source of truth.
- The Result: Analysts spend 80% less time finding data, shifting from “data archaeology” to real-time clinical insight and faster public health responses.
- Key Requirements: Strict HIPAA and FISMA compliance, zero-trust security, and federated governance to ensure data access is limited to those with a “need to know.”
- Core Technologies: Adoption of the OMOP Common Data Model, role-based access controls (RBAC), and FIPS 140-2 validated encryption.
Previously, military providers lacked a single view of patient histories, often forcing service members to carry paper records during Permanent Change of Station (PCS) moves. Analysts spent up to 80% of their time searching across 140 outpatient systems, leading to redundant testing and delayed care. This “data archaeology” meant that by the time a report was generated, the information was often weeks out of date, making it useless for rapid response during events like the COVID-19 pandemic or localized disease outbreaks.
That fragmentation is ending.
Operation Helios moved over 1 petabyte of records into a unified cloud platform, processing 60 billion records annually. This allows a medic in a forward-deployed environment to access the same high-quality data as a specialist at Walter Reed National Military Medical Center. Beyond migration, the challenge is securing Protected Health Information (PHI) while enabling global analytics. This requires zero-trust architectures that meet both HIPAA and DoD-specific FISMA requirements.
I’m Dr. Maria Chatzou Dunford, CEO of Lifebit. We’ve spent 15 years building federated platforms for secure dha cloud data sharing in genomics and research. Our work mirrors DHA’s challenges: balancing data sovereignty with collaboration and maintaining compliance without sacrificing speed. In the federal space, security is the prerequisite for innovation. Without a secure foundation, the most advanced AI tools in the world are a liability rather than an asset.
Key secure dha cloud data sharing vocabulary:
Migrate 1 Petabyte Without Downtime: The Operation Helios Success Story
Operation Helios, launched in December 2020, moved 30 years of MHS data into a centralized environment without disrupting care. This was a mission-critical operation where failure could impact vaccine distribution, readiness tracking, and active clinical trials. The scale involved over 1 petabyte of data dispersed across 35 disparate sources, including legacy systems from the 1990s with significant technical debt.
To put this in perspective, 1 petabyte is equivalent to roughly 500 billion pages of standard printed text. Migrating this volume of sensitive health data while hospitals are actively treating patients is akin to changing the engines on a Boeing 747 while it is mid-flight. The DHA could not afford a single minute of downtime, as clinicians rely on these systems for life-saving decisions every second of the day.

To achieve secure dha cloud data sharing, the team built sophisticated ETL (Extract, Transform, Load) pipelines that validated and cleansed 60 billion records annually. This involved mapping legacy codes—some of which were proprietary or obsolete—to modern standards and reconciling patient identities across systems. A major hurdle was the “identity resolution” problem: ensuring that a record for “John Doe” in an Army clinic was correctly linked to the “John Doe” record in a Navy hospital, despite potential differences in middle initials or social security number formats.
The migration strategy moved the MHS Data Repository (MDR) and MHS Mart (M2) into the cloud first, proving that complex, legacy-heavy organizations can modernize. This mirrors Scientific research on secure clinical data implementation which emphasizes that infrastructure must be lightweight for performance yet heavyweight for security. By utilizing a phased approach, the DHA was able to identify and mitigate risks in smaller batches before scaling to the full petabyte of data.
The ultimate goal was interoperability. By moving away from a “hodgepodge” of systems, the DHA is creating a longitudinal record for every service member that follows them from induction through veteran status. This longitudinal view is essential for identifying long-term health trends, such as the impact of specific environmental exposures during deployment. At Lifebit, our federal health services focus on breaking down these silos so data is accessible where needed without compromising security. Operation Helios serves as a blueprint for other federal agencies to transform data from a liability into a strategic asset, proving that even the most entrenched legacy systems can be modernized with the right governance and technology.
MHS Information Platform: One Source of Truth for 9.6M Patients
The MHS Information Platform (MIP) is the central nervous system for military medical intelligence. By consolidating 35+ sources, the DHA eliminated conflicting results caused by different data refresh rates in legacy databases. In the old system, a commander might see one readiness percentage in the morning, while a medical officer saw a different number in the afternoon because their respective databases synced at different times. The MIP provides a “Single Source of Truth” (SSOT) that ensures everyone is looking at the same data in real-time.
| Feature | Legacy Data Silos | MHS Information Platform (MIP) |
|---|---|---|
| Data Access | Manual, fragmented; required multiple logins | Centralized, automated discovery via single portal |
| Data Volume | Scattered across local servers and tape drives | 1 Petabyte+ consolidated in high-availability cloud |
| Interoperability | Low; conflicting formats (ICD-9 vs ICD-10) | High; standardized via OMOP Common Data Model |
| Security | Perimeter-based (firewalls only) | Zero-trust, FISMA-compliant, identity-centric |
| Analytics Speed | Weeks or months for complex queries | Hours or minutes for enterprise-wide insights |
The MIP aligns with the DOD VAULTIS framework, ensuring data is:
- Visible: Users find data via a centralized catalog. No more guessing which server holds the relevant records.
- Accessible: Available to authorized users regardless of location, whether at a desk in the Pentagon or a field hospital in a combat zone.
- Understandable: Well-documented with clear metadata. Users know exactly what a data field represents and where it came from.
- Linkable: Clinical and operational datasets can be joined. For example, linking weather patterns to respiratory illness rates among deployed troops.
- Trustworthy: Quality ensured through rigorous validation. Automated checks flag anomalies or missing values before they reach the analyst.
- Interoperable: Follows standard formats like OMOP, allowing the DHA to share insights with the VA and CDC seamlessly.
- Secure: Protected by zero-trust and encryption. Data is encrypted at rest, in transit, and even during processing in some advanced enclaves.
As noted in the DOD Data Strategy and VAULTIS goals, the objective is to treat data as a strategic asset. Dr. Jesus Caban, the DHA’s Chief Data and Analytics Officer, has prioritized a master data catalog to reduce administrative overhead. This governed environment uses role-based access and data stewardship to build trust while ensuring individual privacy is never sacrificed through regular audits and compliance checks. By empowering “Data Stewards” within each medical specialty, the DHA ensures that the data remains relevant and accurate for the specific needs of clinicians on the ground.
Standardize Data in Hours: How OMOP Fixes Fragmented Military Records
For decades, military health data was a mix of ICD-9, SNOMED CT, and LOINC codes, often customized by individual facilities. This created a “Tower of Babel” effect where researchers couldn’t easily compare outcomes across different hospitals. To fix this, the DHA adopted the OMOP Common Data Model (CDM), managed by the OHDSI (Observational Health Data Sciences and Informatics) community. OMOP acts as a universal translator, mapping disparate vocabularies into standardized concepts.
This standardization is vital for standardizing metrics via the MHS Common Data Model, allowing coordination with the VA, CDC, and international partners. When a new health threat emerges, such as a novel virus, the DHA can now run a single query across the entire 9.6 million patient population and get results in hours. Previously, this would have required writing custom code for 35 different systems and manually aggregating the results in a spreadsheet—a process that took weeks and was prone to human error.
Analysts were once digital archaeologists, writing custom SQL code for every single query. Now, with automated workflows and the OMOP framework, the 80% time-waste has been flipped. Analysts spend 80% of their time generating insights and 20% on data preparation. This speed is critical for responding to deployment-related illnesses, where identifying a cluster of symptoms early can prevent a widespread health crisis.
Key benefits of the OMOP implementation include:
- Concept Mapping: Automatically converting local “lab codes” into standardized LOINC codes.
- Temporal Consistency: Ensuring that the timeline of a patient’s care is preserved accurately across different recording systems.
- Collaborative Research: Allowing DHA researchers to use open-source tools developed by the global OHDSI community, such as the “Achilles” dashboard for data quality visualization.
This is the philosophy we use at Lifebit with our R.E.A.L. (Real-time Evidence & Analytics Layer). By removing technical friction, the DHA allows its best minds to focus on medicine rather than data cleaning. Standardized data also creates a “plug-and-play” environment for AI models, allowing new capabilities—like predictive sepsis alerts—to be deployed enterprise-wide quickly. Tools like the OHDSI “Athena” vocabulary service ensure that the DHA is always using the most current medical terminologies, keeping information reliable for clinical decisions at the point of care.
Stop Breaches: How Zero Trust Secures DHA Cloud Data Sharing
In secure dha cloud data sharing, security is the foundation. The DHA must comply with HIPAA for patient privacy and FISMA (Federal Information Security Management Act) for federal cybersecurity. A standout achievement is the Comply to Connect (C2C) program, which aligns with zero-trust principles. Unlike traditional networks that rely on a “hard shell, soft center” approach (where once you are inside the firewall, you have broad access), zero-trust assumes no connection is safe; every request must be verified, authenticated, and encrypted.
Critical layers of the DHA’s security architecture include:
- Encryption: Using FIPS 140-2 validated modules for data at rest and in transit. This ensures that even if data is intercepted, it remains unreadable to unauthorized parties.
- Continuous Auditing: The MIP tracks every single access event, creating an immutable audit trail. If a record is viewed, the system logs who viewed it, when, from what device, and for what purpose. This is essential for forensic analysis and HIPAA compliance.
- Device Health Attestation: Before a laptop or tablet can connect to the MIP, the system checks its “health.” If the device is missing a security patch or has unauthorized software installed, access is denied automatically.
- Attribute-Based Access Control (ABAC): This goes beyond simple roles. ABAC considers the user’s role, the sensitivity of the data, the user’s current location (e.g., on-base vs. off-base), and the time of day before granting access. A researcher might have access to anonymized data from their office but be blocked from viewing identifiable records from a public Wi-Fi connection.
These protocols align with NIST guidelines for secure data sharing. By implementing these controls, the DHA has created a “secure enclave” that withstands sophisticated cyber threats while allowing fluid information movement for authorized users.
Consolidating disparate networks into MHS GENESIS (the new electronic health record) required massive cultural shifts alongside the technical ones. With 20,000+ users, the agency invested heavily in “clinical champions”—doctors and nurses who were trained early and helped their peers navigate the new tools. This human-centric approach to security ensures that protocols are followed not just because they are mandatory, but because staff understand how they protect their patients. The success of this transition demonstrates the DHA’s commitment to a data-driven future where technology enables care rather than hindering it through complex, unusable security hurdles.
Predict Injuries Faster: How AI Transforms Military Medical Readiness
With the MIP providing a foundation of high-quality, standardized data, the DHA is shifting from reactive to proactive medicine using Artificial Intelligence (AI) and Machine Learning (ML). Commander David Wright, a leader in DHA’s digital transformation, has noted that AI is the most effective means to improve health results across a massive, global population. By analyzing the 1-petabyte repository, AI can identify patterns that are invisible to the human eye.
Transformative use cases currently being explored or implemented include:
- Predictive Readiness: Identifying service members at risk for musculoskeletal injuries (the #1 cause of medical non-readiness) before they occur. By analyzing training loads and past medical history, AI can suggest modified training schedules for specific individuals.
- Advanced Image Recognition: Using AI to spot early signs of disease in radiology scans or pathology slides. This is particularly vital in remote environments where a general practitioner might need the support of an AI “specialist” to triage urgent cases.
- Casualty Treatment & Triage: AI-driven protocols that help medics in high-stress combat zones prioritize treatments based on the likelihood of survival and available resources. This “augmented intelligence” supports human decision-making when every second counts.
- Precision Medicine: Integrating genomic data with clinical records to tailor treatments to an individual’s genetic profile. This is especially relevant for cancer treatments and mental health prescriptions, where “one size fits all” approaches often fail.
This is where the Lifebit platform excels. Our federated AI approach allows models to run where the data lives. Instead of moving sensitive records to an external lab—which creates security risks and consumes massive bandwidth—the AI comes to the secure DHA cloud. This maintains 100% data sovereignty and compliance with HIPAA and FISMA. The data never leaves the DHA’s secure environment; only the “insights” (the mathematical results of the AI model) are exported.
Service members now access their own records through secure portals like MHS GENESIS Patient Portal, and providers have a 360-degree view of patients. Secure dha cloud data sharing is the engine driving medical readiness. By moving to data-driven health management, the DHA ensures the highest standard of care for the armed forces, whether in a state-of-the-art US hospital or a forward-deployed clinic in a remote region. This evolution protects the military’s most valuable asset: its people. As the DHA continues to refine these tools, the goal remains clear: a medically ready force and a ready medical force, powered by the world’s most secure and advanced health data platform.
Frequently Asked Questions about Secure DHA Cloud Data Sharing
What is Operation Helios?
Operation Helios was a massive, multi-year project that successfully migrated two legacy data warehouses (MDR and M2) and over 1 petabyte of data into the MHS Information Platform (MIP). It involved transferring 30 years of health records from 35+ sources without interrupting patient care.
How does the MHS Information Platform (MIP) protect patient privacy?
The MIP uses a multi-layered security approach including zero-trust architecture (Comply to Connect), role-based access controls, and full encryption of data both at rest and in transit. It is fully compliant with HIPAA for health privacy and FISMA for federal cybersecurity standards.
What role does the Common Data Model play in DHA modernization?
The Common Data Model (specifically OMOP) standardizes health data from different sources into a single “language.” This allows researchers and doctors to query data consistently, regardless of which legacy system it originally came from, improving analytics speed by up to 80%.
Conclusion
The change of the Defense Health Agency from a fragmented network of legacy servers to a unified, AI-ready cloud environment is nothing short of heroic. By prioritizing secure dha cloud data sharing, the DHA has laid the cornerstone for a future where military healthcare is proactive, personalized, and, above all, secure.
At Lifebit, we are proud to support this vision of federated governance and secure collaboration. The lessons learned from Operation Helios and the MIP are a blueprint for any organization handling high-stakes, regulated data.
Secure your federal health data today with Lifebit’s federated platform.

