From Silos to Synergy: Integrating Data for a Healthier Military
Military Healthcare Data Integration: Save Lives and Cut $10B in Waste
Military healthcare data integration is the process of connecting and harmonizing health information across the Military Health System (MHS) to enable seamless care delivery, from the point of injury on the battlefield to veteran repatriation and beyond. For the 9.5 million beneficiaries—active duty service members, military retirees, and their families—integrated data is the backbone of the “Quadruple Aim”: increased readiness, better health, better care, and lower costs.
In the modern defense landscape, integrated data means:
- Faster, more informed clinical decisions through real-time access to complete medical histories, including longitudinal exposure data and previous trauma interventions.
- Improved continuity of care as personnel transition between military treatment facilities (MTFs), deployed units, civilian provider networks, and the Department of Veterans Affairs (VA) systems.
- Improved operational readiness by enabling predictive analytics, AI-driven decision support, and evidence-based resource management that ensures the right medical assets are in the right place at the right time.
- Reduced costs through the elimination of duplicative contracts, streamlined procurement, and optimized supply chains that leverage the DOD’s massive strategic buying power.
- Better research outcomes via longitudinal analysis of exposures, treatments, and health outcomes across diverse populations, facilitating breakthroughs in TBI and PTSD treatment.
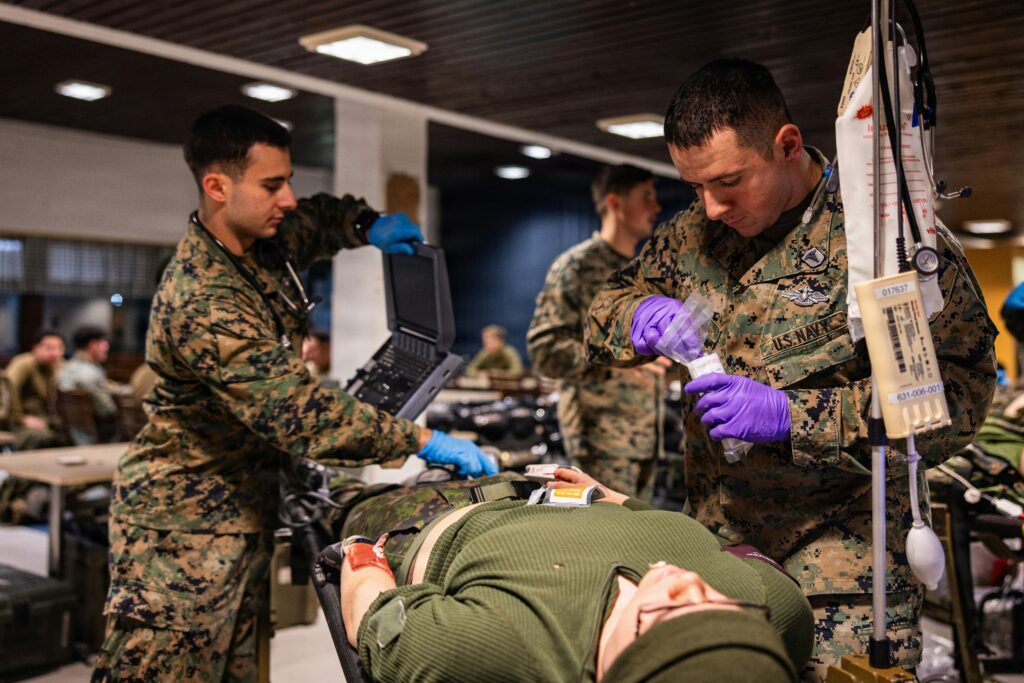
The stakes are high. Military medical personnel often treat everyday illnesses between deployments, lacking daily exposure to high-intensity battlefield trauma. When seconds count in a mass casualty event or combat zone, clinicians need immediate access to patient records, exposure histories, and treatment protocols. Yet the MHS has historically operated with fragmented systems—separate databases for pharmacy, radiology, mental health, and administrative functions—creating dangerous gaps in care. This fragmentation, often referred to as “silos of excellence,” has historically hindered the ability to track a service member’s health journey from enlistment to retirement.
The MHS Digital Change Strategy, published in March 2025, outlines four lines of effort to address these challenges: modernizing infrastructure, developing digital care models, building a digitally competent workforce, and integrating AI with data management. This strategy recognizes that data integration is not a technical nicety but an operational imperative for supporting the National Defense Strategy and saving lives. It moves the MHS from a reactive posture to a proactive, data-driven force multiplier.
From the deployment of MHS GENESIS—the Department of Defense’s single electronic health record—to the Joint Health Information Exchange (JHIE) connecting 268 provider organizations across 2,000 hospitals and 33,000 clinics, the military is changing how health data flows across the care continuum. AI and digital simulation tools now generate biometric training data, predict when medics need skill refreshers, and create virtual trauma scenarios that compress years of experience into minutes. Meanwhile, platforms like the VA’s ADDS UP have surfaced over $90 million in cost avoidance by identifying duplicative contracts through federated data analysis.
But significant barriers remain. Privacy and security concerns, infrastructure limitations in deployed environments (the “disconnected, intermittent, and low-bandwidth” or DIL environment), interoperability challenges across NATO and coalition partners, and the complexity of integrating legacy systems all slow progress. The 2024 GAO audit of MHS GENESIS deployment revealed that while the system is now operational at all military facilities, user satisfaction lags behind benchmarks, and full integration at joint DOD-VA facilities remains incomplete due to legal and policy barriers.
I’m Maria Chatzou Dunford, CEO and Co-founder of Lifebit, where we’ve spent over a decade building federated data platforms that enable secure, real-time analysis across siloed health systems—experience directly applicable to solving military healthcare data integration challenges at scale. In this guide, we’ll walk through the MHS Digital Change Strategy, explore technical solutions to interoperability barriers, and show how integrated data is already improving care from battlefield to bedside.
Must-know military healthcare data integration terms:
Stop Fragmented Care: The MHS Strategy for a Digital Health Force Multiplier
The Military Health System is currently navigating one of its most significant shifts in history. The MHS Digital Change Strategy, finalized in March 2025, serves as the primary roadmap for moving away from fragmented “silos of excellence” toward a unified, data-driven ecosystem. This strategy isn’t just about software updates; it’s about ensuring that the 9.5 million beneficiaries receive world-class care regardless of where they are stationed, whether in a state-of-the-art hospital in Bethesda or a forward operating base in a contested environment. This digital transformation is designed to support the “Quadruple Aim”: increased readiness, better health, better care, and lower costs, aligning military medicine directly with the National Defense Strategy.
We see this strategy as a direct response to the increasing complexity of modern warfare and the growing demands on military readiness. By focusing on four distinct lines of effort, the MHS aims to create a “digital health force multiplier.” These lines of effort include:
- Modernizing the Digital Foundation: Upgrading the underlying hardware, cloud infrastructure, and cybersecurity protocols to support high-speed data exchange. This includes the transition to a cloud-native environment that can handle the massive throughput required for real-time genomic and imaging data.
- Making Digital Health the New Standard of Care: Transitioning from traditional in-person models to a hybrid approach that includes telehealth, remote patient monitoring, and AI-assisted diagnostics. This ensures that a specialist in San Antonio can support a general surgeon in a deployed environment via high-definition tele-surgical links.
- Building a Digitally Competent Workforce: Ensuring that every medic, nurse, and physician is trained not just in medicine, but in the use of advanced data tools and EHR systems. This involves a cultural shift where data literacy is treated as a core military competency, similar to marksmanship or physical fitness.
- Integrating AI and Data Management: Moving toward a “data-centric” architecture where information is treated as a strategic asset, governed by strict standards and accessible for real-time analytics. This line of effort focuses on breaking down the remaining barriers between clinical, administrative, and operational data sets.
Modernizing Infrastructure for military healthcare data integration
The first line of effort involves a massive investment in the existing digital health infrastructure. For years, clinicians had to steer multiple legacy systems—such as AHLTA (Armed Forces Health Longitudinal Technology Application), CHCS (Composite Health Care System), and Essentris—that didn’t always talk to each other. The rollout of MHS GENESIS—a commercial-off-the-shelf electronic health record (EHR) system based on Oracle Health—replaces these disparate systems with a single record for every service member. This transition is critical for eliminating the “paper trail” that often led to lost records during permanent change of station (PCS) moves, which occur for roughly one-third of the force every year.
However, as the April 2024 GAO report points out, modernization is about more than just flipping a switch. While the DOD has deployed the system across 700 facilities, challenges remain in joint facilities where DOD and VA workflows diverge. To achieve true military healthcare data integration, we must address the legal and policy barriers that force staff to switch between different system configurations for pharmacy, dental, and pediatrics. The report emphasizes that “interoperability is not just a technical achievement but a workflow requirement.” This means that the data must not only be present but must be presented in a way that fits the high-tempo clinical environment of a military treatment facility.
Future-Proofing Readiness via military healthcare data integration
Readiness is the heartbeat of military medicine. Data integration allows us to shift from a reactive “document what happened” model to a proactive “anticipate what’s needed” model. By integrating health data from training, deployments, and garrison care, the MHS can perform real-time health surveillance. This includes monitoring for clusters of injuries or illnesses that could indicate a broader readiness issue, such as a localized outbreak of a respiratory virus or a spike in musculoskeletal injuries related to a specific training protocol.
This is particularly vital for the National Defense Strategy. When we integrate data, we aren’t just filing records; we are building a longitudinal view of warfighter health. This includes the Individual Longitudinal Exposure Record (ILER), which tracks environmental exposures—such as burn pits, chemicals, or radiation—throughout a service member’s career. According to research on military EHR systematic reviews, these integrated systems are essential for improving patient safety and ensuring that when a warfighter is deployed, their medical history—including every allergy, immunization, and past trauma—is already there waiting for the medic. This “pre-deployment health visualization” ensures that commanders know exactly who is fit for duty and what medical support is required for specific missions, reducing the risk of non-battle injuries (DNBI) that historically account for more medical evacuations than combat wounds.
End the Security-Access Paradox: Securely Sharing Military Health Data
Integrating healthcare data in a military context is like trying to change the tires on a Humvee while it’s moving at 60 mph. We face a “security-access paradox”: we need data to be instantly available to a medic in a remote location to save a life, but it must also be protected by the most rigorous encryption and privacy standards to prevent sensitive information from falling into the hands of cyber adversaries. A breach of military health data isn’t just a privacy violation; it’s a national security risk that could reveal unit locations, readiness levels, or vulnerabilities. For instance, an adversary could analyze aggregated health data to determine the combat effectiveness of a specific unit or identify the arrival of new forces in a theater of operations.

Standardizing Interoperability for military healthcare data integration
Interoperability is the “language” that allows different systems to communicate. In the past, data was often trapped in proprietary formats, making it nearly impossible to share between a Navy ship and a Landstuhl Regional Medical Center. Today, the MHS is moving toward international standards like HL7 FHIR (Fast Healthcare Interoperability Resources). FHIR is a game-changer because it uses modular, lightweight “resources”—such as Patient, Observation, and MedicationRequest—that allow for real-time data exchange via RESTful APIs. This essentially makes healthcare data as easy to share as a web page, while maintaining strict security protocols.
Beyond FHIR, NATO standards (such as STANAGs) are crucial for coalition operations. When US, UK, and Canadian forces operate together in a multinational task force, their medical systems must be able to share patient tracking and evacuation data seamlessly. This semantic interoperability ensures that “blood type A+” means the same thing in a British field hospital as it does in a US Navy ship’s sickbay. Without these standards, the risk of medical errors during handoffs between coalition partners increases exponentially. The MHS is currently working on mapping these NATO standards to the FHIR framework to ensure that US forces can lead in a multi-domain, multi-national medical environment.
Solving the Security-Access Paradox
Privacy and security are non-negotiable. Military health data contains personally identifiable information (PII) and protected health information (PHI) that are high-value targets for state-sponsored cyber actors. To solve this, the MHS is adopting a Zero Trust Architecture, which assumes that no user or system is trusted by default, regardless of whether they are inside or outside the network perimeter. This architecture is built on five pillars: Identity, Device, Network, Application, and Data. Key components include:
- Rigorous Encryption: Protecting data at rest and in transit using FIPS 140-3 validated modules, ensuring that even if data is intercepted, it remains unreadable to unauthorized parties.
- Federated Data Networks: Instead of moving all data to a central “honey pot” that could be breached, federated models (like the ones we champion at Lifebit) allow researchers and clinicians to analyze data where it lives. This “data-to-code” approach ensures that sensitive records never leave their secure environment, significantly reducing the attack surface.
- Identity and Access Management (IAM): Using multi-factor authentication (MFA) and role-based access controls (RBAC) to ensure that a medic only sees the data necessary for the immediate treatment of a patient. For example, a medic in the field may have access to blood type and allergies, while a psychiatrist at an MTF has access to mental health records.
- Trust Agreements: Frameworks like the Data Use and Reciprocal Support Agreement (DURSA) ensure that every partner in the Joint HIE follows the same security playbook, creating a “circle of trust” that extends to civilian providers.
Research on UK Armed Forces EHR integration highlights that even with different national health systems (like England, Scotland, and Wales), using “variable commonality” can help harmonize datasets for research while maintaining local data sovereignty. This model serves as a blueprint for how the US DOD can integrate with international partners while respecting national security constraints and individual privacy laws.
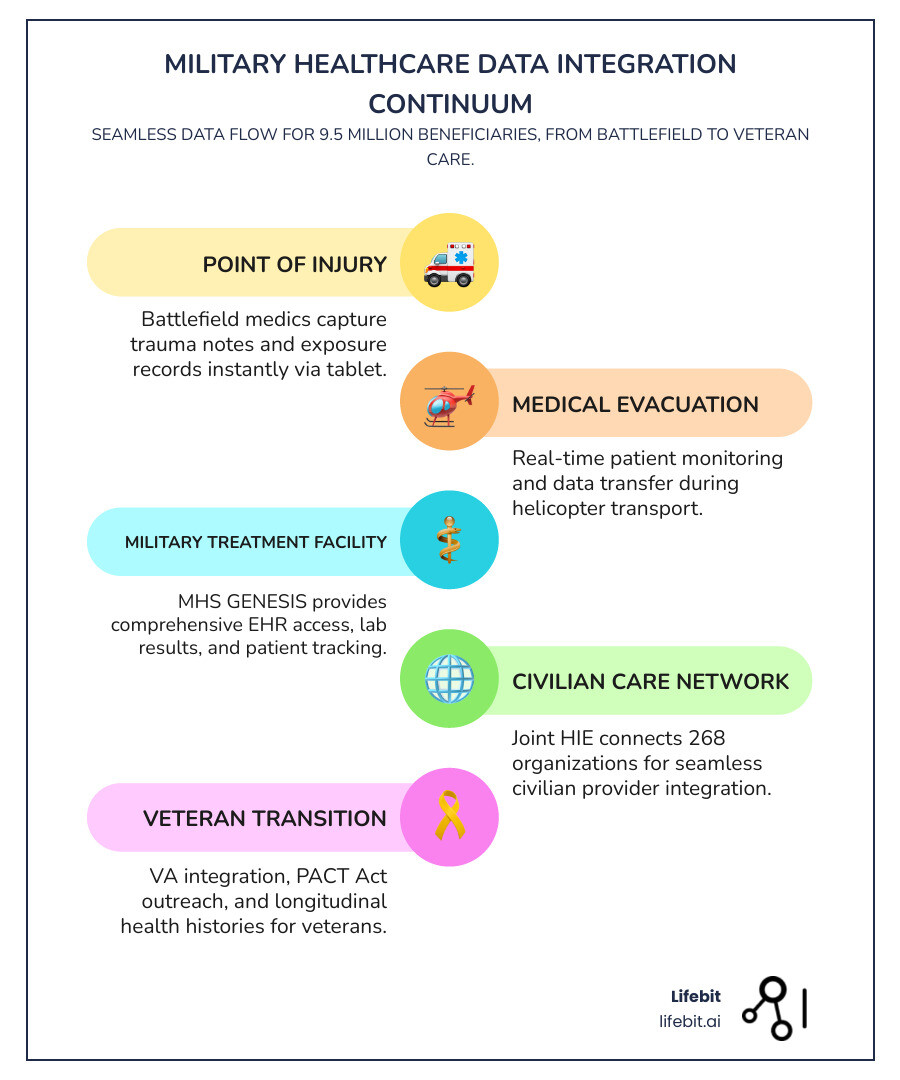
Battlefield to Bedside: How Integrated Data Saves Warfighters in the Golden Hour
The ultimate goal of military healthcare data integration is to save lives. This “continuum of care” starts at the point of injury and doesn’t end until the service member has successfully transitioned to veteran status. In military medicine, we talk about the “Golden Hour”—the critical window where rapid medical intervention can mean the difference between life and death. Integrated data is the fuel that accelerates care during this window, supporting the “10-1-2” rule: 10 minutes for point-of-injury care, 1 hour for surgical intervention, and 2 hours for stabilization.
Streamlining the Care Continuum
Imagine a medic on a night watch in a remote duty station. They use a ruggedized tablet to access the medical history of a soldier who has just sustained a blast injury. Because of the Joint Health Information Exchange (JHIE), that medic can see if the soldier has any drug allergies, pre-existing conditions, or previous TBI history that might complicate treatment. This information is pulled in real-time from MHS GENESIS, even if the soldier was last treated at a different facility thousands of miles away. This immediate access prevents adverse drug reactions and allows the medic to tailor their interventions to the soldier’s specific physiological profile.
As the patient is evacuated, their “digital twin”—their integrated health record—moves with them. This is facilitated by the Theater Medical Information Program – Joint (TMIP-J) and its successors, which ensure that data captured at the point of injury flows into the permanent record. By the time the patient arrives at a major military treatment facility (MTF) or a civilian trauma center, the surgeons already have the battlefield notes, imaging results, and vital signs recorded during transport. This seamless handoff reduces errors, eliminates the need for redundant testing, and speeds up life-saving interventions. Furthermore, the Joint Patient Tracking Application (JPTA) allows commanders and medical planners to see the status and location of every casualty in real-time, optimizing the flow of patients through the evacuation chain.
Enhancing Veteran Transitions
One of the most significant successes in recent years is the integration between the DOD and the VA. Historically, “the handoff” was where many veterans fell through the cracks, leading to delayed benefits and interrupted care. Now, with the PACT Act and improved data sharing, the transition is becoming more automated. The Individual Longitudinal Exposure Record (ILER) plays a central role here, providing the VA with a clear history of a veteran’s environmental exposures, which is essential for processing disability claims related to toxic substances. This record is built from data captured during every deployment, including air quality sensors, water testing, and proximity to known hazards like burn pits.
For example, the VA used a data-driven outreach platform to identify veterans exposed to toxic burn pits. By unifying millions of siloed data points from DOD deployment records and VA health records, they were able to launch targeted messaging campaigns. The result? 1,800 Vietnam veterans registered for VA healthcare for the first time after a single targeted campaign. This is the power of integrated data—it finds the people who need help, validates their service-connected conditions, and brings them into the system of care they earned. It also ensures that the VA has the necessary data to conduct long-term epidemiological studies on the effects of military service, leading to better clinical guidelines for veteran-specific conditions.
AI-Driven Readiness: Gain Years of Trauma Experience in Minutes
We are entering an era where AI doesn’t just store data; it learns from it to predict the future. The MHS has been conducting AI/ML inventories since 2018, and the 2025 strategy places AI at the center of medical training, clinical support, and population health. By leveraging the massive datasets generated by integrated EHRs, the military can develop algorithms that provide real-time guidance to clinicians in high-stress environments, effectively acting as a “digital consultant” on the battlefield.
AI-Driven Decision Support
AI algorithms are now being used to scan integrated health records for early warning signs of conditions that are often difficult to diagnose in their early stages. This includes:
- PTSD and Suicide Risk: Identifying patterns in mental health encounters, pharmacy data, and even wearable data (like sleep patterns or heart rate variability) to flag at-risk individuals before a crisis occurs. This allows for “left of bang” interventions—preventative measures taken before a traumatic event or crisis—that save lives and preserve unit cohesion.
- Traumatic Brain Injury (TBI): Correlating blast exposure records from wearable sensors with clinical symptoms and neuroimaging for more accurate screening and long-term monitoring. AI can identify subtle cognitive declines that might be missed in a standard clinical exam.
- Population Health and Bio-Surveillance: Real-time surveillance of disease outbreaks across global bases, allowing the DHA to move resources and implement quarantine protocols before an outbreak impacts mission readiness. This was particularly effective during the COVID-19 pandemic, where data integration allowed for rapid tracking of vaccination rates and infection clusters.
High-Fidelity Simulation for Medics
Digital simulation tools are a “game changer” for medical readiness. Most military clinicians don’t see trauma every day, especially during periods of lower-intensity conflict. AI-driven simulations allow them to gain “years of trauma experience in minutes” by practicing on virtual patients that react with physiological realism. These simulations use synthetic data derived from real-world trauma cases to create scenarios that are indistinguishable from reality.
| Feature | Legacy Training | AI-Driven Simulation |
|---|---|---|
| Realism | Static mannequins with limited feedback | High-fidelity VR with human-like physiological responses |
| Data Capture | Manual observation by instructors | Automated biometric and task-performance data capture |
| Accessibility | Requires travel to specialized training centers | Portable VR headsets available at remote duty stations |
| Repetition | Limited by resources and instructor time | Infinite repetition until muscle memory is built |
| Feedback | Delayed instructor review | Instant, data-driven dashboards with performance metrics |
These tools generate biometric data that feeds into readiness dashboards, allowing leaders to predict when a medic’s skills are starting to “atrophy.” If a medic hasn’t performed a needle decompression or applied a junctional tourniquet in six months, the system can flag them for a custom VR refresher by dawn, ensuring they are always mission-ready. This data-driven approach to training ensures that the medical force is not just “trained” but “proficient” at all times.
Cut $92M in Waste: How Federated Data Analysis Optimizes Military Health
Beyond the clinic, military healthcare data integration is changing how the Military Health System manages its multi-billion dollar budget and conducts life-saving research. The MHS is one of the largest healthcare delivery systems in the world, and even small gains in efficiency can lead to massive savings that can be reinvested into warfighter care and advanced medical research.
Optimizing the Military Health System
Efficiency isn’t just about saving money; it’s about reallocating resources to where they can do the most good. The VA’s ADDS UP (Acquisition Data Driven Support Unit Platform) is a prime example of how data integration impacts the bottom line. By integrating disparate acquisition data from across the enterprise, the platform:
- Surfaced over 1,300 duplicative contracts for the same medical supplies, such as surgical gloves and orthopedic implants.
- Resulted in $92 million in cost avoidance in just six months by consolidating those contracts and negotiating better rates.
- Prevented an estimated $10.9 billion in inefficient spending over a five-year projection by identifying systemic procurement bottlenecks.
This level of transparency allows leadership to leverage “strategic buying power,” ensuring that medical supplies—from bandages to advanced imaging equipment—are procured at the best price and are available when and where they are needed. It also streamlines the supply chain, reducing the risk of stockouts during a surge in demand or a logistical disruption in a contested environment. By integrating logistics data with clinical demand forecasts, the MHS can ensure that the right blood types and medications are pre-positioned for upcoming operations.
Advancing Global Health Research with OMOP
Integrated data is a goldmine for epidemiological research. However, for research to be effective, data must be harmonized. The MHS is increasingly adopting the OMOP Common Data Model (CDM). OMOP allows data from different sources (EHRs, insurance claims, registries) to be transformed into a common format, enabling researchers to run the same analysis across multiple datasets without moving the data. This is particularly important for military research, where data must remain within secure, classified, or highly protected environments.
By linking records across nations—as seen in the UK’s framework for England, Scotland, and Wales—researchers can track the long-term health consequences of military service on a global scale. This research informs policy, such as new protocols for toxic exposure or improved treatments for service-related injuries. The Individual Longitudinal Exposure Record (ILER) is particularly important here. It allows us to look back decades and see if a specific deployment environment is linked to later health outcomes like rare cancers or respiratory diseases. This research is only possible when data is integrated, harmonized, and accessible to authorized researchers in a secure, federated environment like a Trusted Research Environment (TRE). These TREs provide a secure “sandbox” where researchers can analyze sensitive data without the risk of data exfiltration, ensuring that national security and patient privacy are maintained while driving medical innovation.
Military Healthcare Data Integration: Your Top Questions Answered
What are the primary benefits of integrating military healthcare data?
The primary benefits include improved clinical decision-making through real-time access to records, better continuity of care as service members move between systems, improved operational readiness for the warfighter, and significant cost savings through streamlined resource management. It also enables long-term research into service-connected illnesses.
How does the Joint Health Information Exchange (JHIE) protect patient privacy?
The JHIE uses a secure gateway that complies with rigorous HIPAA and DOD privacy standards. All participating organizations must sign comprehensive trust agreements (DURSA or EULA). Data is encrypted in transit and at rest, and the system uses audit logs to track every instance of data access. Additionally, beneficiaries have the option to opt out of sharing their data with civilian partners.
What role does AI play in the MHS Digital Change Strategy?
AI is central to the strategy, focusing on four areas: integrating AI with data management for better insights, using AI for predictive health surveillance (like PTSD or suicide risk), enhancing medical education through high-fidelity simulations, and optimizing administrative tasks like acquisition and supply chain management. AI helps turn “big data” into “actionable intelligence.”
What is the OMOP Common Data Model and why is it used?
OMOP (Observational Medical Outcomes Partnership) is a standard format for health data. It is used by the DHA to harmonize data from different legacy systems and MHS GENESIS. This allows researchers to analyze data from millions of patients consistently, which is essential for identifying trends in military-specific health issues like blast injuries or toxic exposures.
How does data integration help in “disconnected” environments?
Modern integration strategies use “store-and-forward” technology and edge computing. This allows medics in low-bandwidth environments to capture data locally on ruggedized devices. Once a connection is re-established, the data automatically syncs with the central MHS GENESIS record, ensuring the continuum of care remains unbroken even in the most remote locations.
Stop Silos. Start Synergy: The Future of Military Health
The journey from fragmented data silos to a synergistic, integrated Military Health System is well underway. While the technical and policy challenges are significant, the progress made through MHS GENESIS, the Joint HIE, and AI-driven simulation proves that the vision of a “healthier military” is achievable. The transition from a system-centric to a data-centric model is the defining challenge of this decade for military medicine.
At Lifebit, we believe that federated AI and secure data integration are the keys to open uping the full potential of military health data. By enabling real-time evidence and analytics through our Trusted Research Environments (TRE) and Data Lakehouses, we help organizations bridge the gap between complex, siloed data and actionable insights. Whether it’s tracking a warfighter’s health across five continents, identifying the long-term effects of environmental exposures, or optimizing a massive global supply chain, the goal remains the same: ensuring those who serve have the best possible care, from the first day of training to their final days as a veteran.
For more information on how we support the future of military medicine through secure, federated data solutions, visit our federal health services page. Together, we can ensure that data is never a barrier, but always a bridge to better health and mission success.

