Mastering the Art of EHR and Claims Data Integration

EHR Claims Data Integration: Get Real-Time Patient Insights in 48 Hours
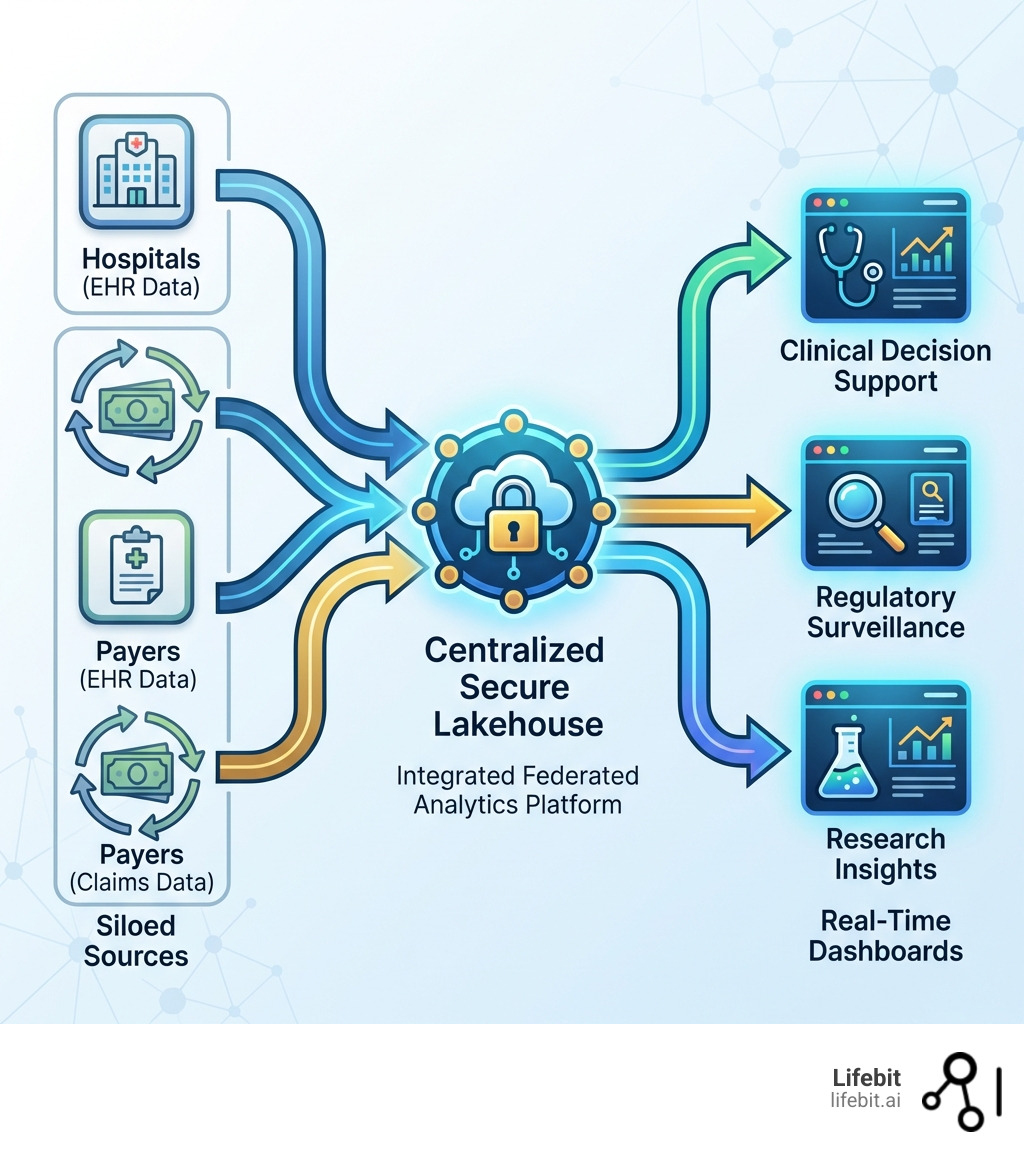
EHR claims data integration is the process of combining clinical data from electronic health records (EHRs) with administrative data from medical claims to create a complete view of the patient journey. In the modern healthcare landscape, where data is generated at an unprecedented rate, the ability to synthesize these two disparate sources is no longer a luxury—it is a fundamental requirement for survival and innovation.
Historically, healthcare data has existed in silos. Clinical teams worked within the EHR, documenting the nuances of patient care, while administrative teams worked with claims, focusing on billing and reimbursement. This separation created a “blind spot” in patient care. EHR claims data integration bridges this gap, allowing organizations to see not just what happened during a specific visit, but the entire longitudinal history of a patient across the continuum of care.
Key Benefits:
- Complete patient profiles – Claims capture longitudinal care across all providers (including out-of-network visits), while EHRs provide clinical depth like lab results, vital signs, and physician notes.
- Faster insights – Partially adjudicated claims data available in 2-4 days via modern APIs vs. weeks for full processing, enabling rapid intervention in acute care settings.
- Better outcomes – Enhanced clinical decision-making through a 360-degree view, reduced care gaps, and improved regulatory compliance for programs like HEDIS and MIPS.
- Higher ROI – 99% first-pass claims acceptance rates, reduced denials, and accelerated reimbursements by identifying coding errors before submission.
Main Challenges:
- Inconsistent data standards – Different systems use different versions of HL7, FHIR, or proprietary formats, making semantic interoperability difficult.
- Manual processes – Many organizations still rely on manual CSV exports and FTP transfers that don’t scale and are prone to human error.
- HIPAA compliance and security risks – Moving sensitive PHI between systems increases the attack surface, requiring robust encryption and governance.
- Legacy system limitations – Older EHRs often lack the modern RESTful APIs needed for real-time data exchange.
Proven Solutions:
- FHIR APIs – Utilizing the Fast Healthcare Interoperability Resources standard for standardized, secure data exchange.
- Cloud-based data lakehouse architecture – Combining the flexibility of a data lake with the performance of a data warehouse to store structured and unstructured data.
- Pre-built accelerators – Using tools like EHRapid Connect to cut implementation from years to weeks.
- Automated ingestion and governance – Implementing automated pipelines that clean, normalize, and secure data from day one.
The challenge is real: claims data tells you where and when care happened, but not why or what the results were. EHR data captures clinical details like symptoms and lab values, but often misses care delivered outside a single system. Neither source alone gives you the full story. For example, a claim might show a patient was hospitalized for heart failure, but only the EHR will show the ejection fraction or the specific titration of medications that led to their recovery.
That’s why the FDA’s Sentinel System now covers over 100 million lives by combining both data types for post-market drug safety surveillance. It’s why oncology researchers use integrated data to support regulatory approvals by tracking patient outcomes long after a clinical trial ends. And it’s why healthcare organizations achieve measurable improvements in care coordination, cost reduction, and patient outcomes when they get integration right.
As Maria Chatzou Dunford, CEO and Co-founder of Lifebit, I’ve spent over 15 years building platforms that tackle the hardest problems in computational biology and health-tech, including the secure integration of EHR, claims, and genomic data across federated environments. This guide will walk you through exactly how to implement EHR claims data integration that scales, protects patient privacy, and delivers real-time insights.
Quick ehr claims data integration terms:
Claims vs. EHR: Why Your Patient Data Is Only Half the Story
To master ehr claims data integration, we must first understand the fundamental differences between our two primary ingredients. Think of claims data like a credit card statement: it tells you exactly where a patient shopped and what they paid for, but it doesn’t tell you if the shoes they bought actually fit or if they liked the color. EHR data, on the other hand, is the personal diary of the clinician—it contains the “why” behind the care, the clinical nuances that a billing code simply cannot capture.
| Feature | Claims Data | EHR Data |
|---|---|---|
| Primary Purpose | Billing, Reimbursement, and Administrative Tracking | Clinical Care, Documentation, and Patient Management |
| Strengths | Longitudinal tracking; captures all providers; high volume; standardized codes | Deep clinical insights; lab results; vital signs; unstructured notes |
| Limitations | Lacks clinical depth (symptoms, results); coding lag (weeks/months); “upcoding” risks | Fragmented (siloed by system); missing out-of-network care; inconsistent data entry |
| Data Types | ICD-10, CPT codes, NDC codes, Revenue codes, costs | Lab values (LOINC), physician notes (NLP), imaging, vitals, RxNorm |
Scientific research on data source strengths and limitations highlights that while claims are excellent for incidence rates and utilization, they often underestimate clinical severity. For example, during the COVID-19 pandemic, relying solely on procedure codes in claims often missed the actual oxygen saturation levels or ventilator settings found only in electronic medical record systems. A claim might show a diagnosis of “Respiratory Failure,” but the EHR provides the specific arterial blood gas results that dictate the urgency of care.
The Blind Spots of Single-Source Data
When we rely on claims data alone, we suffer from “coding lag.” A claim is typically generated after the care is delivered, and it may take weeks to be processed and adjudicated. This makes it nearly impossible to use claims for real-time clinical intervention. Furthermore, claims are subject to “billing bias,” where codes are selected based on reimbursement rules rather than pure clinical observation.
Conversely, EHR data is often “siloed.” If a patient visits an emergency room while on vacation, their primary care physician’s EHR will likely have no record of that encounter unless the two systems are explicitly linked. This lack of interoperability leads to redundant testing, adverse drug events, and a fragmented understanding of the patient’s health. By integrating these sources, we create a “closed-loop” system where the EHR provides the clinical context and the claims provide the longitudinal continuity.
We also distinguish between “open” and “closed” claims. Open claims offer an unbiased, longitudinal view across various payers but may miss specific interactions if the data aggregator doesn’t have a relationship with a particular provider. Closed claims provide a complete view within a single payer—including pharmacy fills—but often come with significant delays. By integrating these with EHRs, we can confirm medication adherence (seeing the prescription in the EHR and the fill in the claims) and validate outcomes with real lab results.
Why ehr claims data integration is essential for Life Sciences
In Life Sciences, relying on a single data source is like trying to solve a jigsaw puzzle with half the pieces missing. For Health Economics and Outcomes Research (HEOR) and drug development, link-claims-ehr-data-real-world-evidence is the gold standard for generating robust Real-World Evidence (RWE).
In oncology research, for instance, EHR data from specialized systems like iKnowMed captures medical histories for over 1 million patients annually. However, without claims integration, researchers might miss the care a patient receives when they visit an emergency room outside their primary oncology network. Integrated data allows us to identify patient cohorts with specific biomarkers (from the EHR) and follow their journey across every site of care (from the claims), providing the comprehensive evidence required for regulatory submissions and market access strategies. This is particularly critical for rare diseases, where every data point is vital for understanding the natural history of the disease.
Stop the Delay: Use FHIR APIs for 2-Day Data Integration
The road to integration is often blocked by “patchwork” IT systems. We frequently see healthcare organizations struggling with inconsistent standards where one system defines an “encounter” differently than another. Manual processes—like troubleshooting brittle FTP transfers or manually mapping CSV columns—quietly drain resources and introduce human error that can compromise patient safety.
Security is the biggest hurdle. Healthcare faces the highest breach costs of any industry, averaging nearly $11 million per incident. Compliance with HIPAA, GDPR, and 42 CFR Part 2 (for substance use disorder records) is non-negotiable. Harmonizing disparate electronic health records requires a system that doesn’t just move data, but standardizes it while maintaining strict audit trails. Legacy systems often lack the modern APIs needed for this, forcing teams to retrofit old technology into new cloud architectures—a process that can take years if done manually.
Leveraging FHIR APIs and BCDA for real-time ehr claims data integration
The game-changer in this space is the shift toward Bulk Fast Healthcare Interoperability Resources (FHIR). This standard allows us to move data in bulk using secure, standardized JSON schemas, moving away from the clunky HL7 v2 messages of the past. FHIR uses modern web technologies (REST, OAuth2) to make data exchange as simple as any other modern web service.
About BCDA (Beneficiary Claims Data API) is a prime example of this evolution. Released by CMS, it allows eligible entities to access Medicare Parts A, B, and D claims data. Most importantly, it provides access to partially adjudicated claims. While fully adjudicated claims can take 14 to 30 days or longer to process, partially adjudicated data is available in just 2-4 days. This allows for near-real-time monitoring of hospital discharges or ER visits, enabling care managers to intervene before a patient is readmitted.
Our approach to ehr-claims-integration leverages these APIs to automate ingestion into a unified NDJSON (Newline Delimited JSON) format. By using the /Group and /Patient endpoints, we can filter for exactly the data needed, reducing noise and accelerating the time it takes to move from raw data to actionable insight. This technical efficiency is what allows Lifebit to deliver integrated insights in a fraction of the time required by traditional ETL (Extract, Transform, Load) processes.
The Role of Semantic Interoperability
It’s not enough to just move the data; the systems must understand what the data means. This is “semantic interoperability.” When one EHR uses a local code for “Glucose Test” and another uses a LOINC code, the integration layer must map these to a common standard. Without this, your analytics will be flawed. We utilize automated mapping tools that leverage machine learning to identify and normalize these disparate codes, ensuring that when you run a query across your integrated dataset, you are comparing apples to apples.
The 6-Step Blueprint to 99% Claims Acceptance and Higher ROI
Success in ehr claims data integration isn’t about the biggest budget; it’s about the best strategy. We recommend a phased approach that prioritizes high-value use cases to secure early wins and leadership buy-in. A “big bang” approach often fails due to the sheer complexity of healthcare data.
- Define Your Data Strategy: Identify the specific business decisions your data must support. Are you looking to reduce readmissions, optimize your supply chain, or generate RWE for a new drug launch? Defining the “North Star” prevents scope creep.
- Build a Scalable Cloud Architecture: Move away from on-premise silos. A Trusted Data Lakehouse (TDL) provides the flexibility to store both structured clinical data and unstructured notes. This architecture allows for high-performance SQL queries alongside advanced machine learning workloads.
- Automate Ingestion: Stop relying on manual extracts. Use pre-built accelerators—like EHRapid Connect—to cut implementation time from years to weeks. Automation ensures that your data is always fresh, which is critical for real-time clinical decision support.
- Enforce Governance and Standardization: Implement unified data models (like OMOP or FHIR) and automated quality checks from day one. Refer to our ehrs-complete-guide for best practices on data stewardship. Governance should include data lineage, so you always know where a specific data point originated.
- Phased Rollout: Start with a single department (e.g., Cardiology) or a high-priority patient cohort (e.g., Diabetic patients with multiple comorbidities) before scaling across the enterprise. This allows you to refine your processes in a controlled environment.
- Continuous Optimization: Regularly review your integration against evolving regulations (like the 21st Century Cures Act) and new data sources like multi-omics or social determinants of health (SDoH).
Measuring the ROI of integrated healthcare data
The financial impact of getting this right is staggering. For example, Inovalon Claims Management Pro has demonstrated a 99% first-pass claims acceptance rate. By integrating claims with EHR data, organizations can automatically pre-screen for errors—such as a procedure code that doesn’t match the clinical diagnosis in the EHR—drastically reducing denials and “timely filing” write-offs.
Beyond the billing office, Data Stewardship and methodological rigor improve clinical decision-making. When a doctor has a holistic view of a patient’s out-of-network history, they avoid redundant testing (saving hundreds of dollars per patient) and prevent adverse drug events (saving thousands in potential litigation and care costs).
The Cost of Inaction
Organizations that fail to integrate their data face significant risks. Beyond the obvious financial losses from denied claims, there is the “opportunity cost” of missed research insights. In the competitive world of biopharma, being six months late to market because of fragmented data can result in billions of dollars in lost revenue. More importantly, it means patients wait longer for life-saving treatments. Integrated data is the fuel for the modern healthcare engine; without it, the engine stalls.
From FDA Safety to COVID-19: EHR Integration in Action
The value of ehr claims data integration is best seen in action. The FDA’s Sentinel System is a landmark example of how large-scale integration can transform public health. Mandated by the FDAAA of 2007, it now monitors the safety of drugs across more than 100 million lives. By supplementing claims with EHR data, the FDA can validate code-based algorithms with actual clinical outcomes. For instance, if a claim shows a patient took a specific drug and then had a “cardiac event,” the EHR can be used to verify if that event was truly a myocardial infarction or something else entirely.
During the COVID-19 pandemic, this integration was vital for survival. Researchers used claims to track patient enrollment and medical history, while using EHRs to monitor real-time vital signs, respiratory indicators, and lab results like D-dimer levels. This allowed for the rapid identification of risk factors and the evaluation of treatments like dexamethasone in real-world settings, long before formal clinical trials were completed.
Population Health and Value-Based Care
In the realm of Value-Based Care (VBC), integration is the key to managing risk. Accountable Care Organizations (ACOs) use integrated data to identify “high-utilizers”—patients who frequently visit the ER but whose underlying conditions are not being managed effectively. By combining EHR data (showing uncontrolled blood sugar) with claims data (showing multiple ER visits for ketoacidosis), care managers can intervene with home health services, reducing costs and improving the patient’s quality of life.
Similar technology is used for sepsis prediction via machine learning. Sepsis is a leading cause of hospital death, but it is notoriously difficult to diagnose early. By streaming EHR data (vitals, labs) and comparing it against historical claims data (comorbidities), AI models can alert clinicians to a patient’s risk hours before they show clinical signs of crashing. These electronic-health-records-programs prove that when data is integrated, we don’t just see the past—we can predict the future and save lives in the process.
Beyond the Note: Open up the 80% of Health Data Trapped in EHRs
The next frontier of ehr claims data integration lies in the “unstructured” world. It is a well-known industry fact that up to 80% of healthcare data is trapped in physician notes, discharge summaries, and pathology reports. This data is often the most valuable, containing the “nuance” of a patient’s condition that cannot be captured in a dropdown menu. We are now seeing Natural Language Processing (NLP) tools that can “read” these ehrs and turn them into structured data points for analysis.
For example, an NLP model can scan thousands of physician notes to identify patients who are experiencing a specific side effect of a medication that doesn’t have a dedicated ICD-10 code. This “signal detection” is a game-changer for pharmacovigilance and drug safety.
The Rise of Multi-Modal and Federated Analytics
Furthermore, the rise of multi-modal systems is allowing us to combine EHR and claims data with genomic and imaging data. This creates a “360-degree” patient view that powers AI-driven safety surveillance and real-time evidence generation. Imagine a researcher being able to query a dataset to find all patients with a specific genetic mutation (genomic data) who were treated with a specific drug (claims data) and showed a positive response in their tumor size (EHR/imaging data).
At Lifebit, we believe the future is federated. Traditional data integration often involves moving massive amounts of sensitive data to a central location, which creates enormous security risks and regulatory hurdles. Our federated approach allows researchers to access and analyze these massive, sensitive datasets without the data ever having to leave its secure home. The analysis “travels” to the data, rather than the data traveling to the analysis. This preserves patient privacy while enabling the large-scale collaboration necessary for the next generation of medical breakthroughs.
Privacy-Preserving Record Linkage (PPRL)
To make this work, we use Privacy-Preserving Record Linkage (PPRL). This technology allows us to link a patient’s record in a claims database with their record in an EHR database without ever seeing their name, Social Security number, or other identifying information. By using secure “tokens,” we can ensure that we are looking at the same patient across different systems while maintaining 100% anonymity. This is the cornerstone of ethical, modern ehr claims data integration.
EHR Claims Data Integration: Your Top Questions Answered
What is the difference between partially and fully adjudicated claims?
Partially adjudicated claims are shared via APIs like BCDA just 2-4 days after a provider submits them to Medicare. They contain raw financial and clinical details used for rapid intervention and care coordination. Fully adjudicated claims are the “final word,” typically available after 14 to 30 days, and include historical data, finalized reimbursement details, and any adjustments made during the review process. For ACO REACH participants, daily updates of partial claims allow for much faster care coordination and risk management.
How do FHIR APIs facilitate ehr claims data integration?
FHIR (Fast Healthcare Interoperability Resources) provides a standardized language for healthcare systems to talk to each other. By using modern HL7 standards and JSON schemas, FHIR APIs allow for secure, automated workflows. Instead of custom-building a bridge for every system, FHIR provides a universal “plug-and-play” connector. This reduces the cost of integration and ensures that data remains consistent as it moves between an EHR and a claims database.
Why is data governance critical for life sciences research?
Without governance, you have data, but you don’t have trust. Governance ensures data quality, protects patient privacy, and maintains the audit trails required for regulatory compliance. It involves defining who can access the data, how it can be used, and how it is protected. As experts like Ryan Leurck on RWD insights point out, the integration of claims and EHR data is only powerful if the resulting insights are based on a foundation of methodological rigor and trustworthy analytics.
Can integrated data help with clinical trial recruitment?
Absolutely. One of the biggest challenges in clinical trials is finding the right patients. By integrating EHR data (to find patients with the right clinical profile) with claims data (to see where those patients are receiving care), researchers can identify “hot spots” for recruitment. This can shave months off the clinical trial timeline and ensure that the trial population is more representative of the real-world patient population.
What is the role of OMOP in data integration?
OMOP (Observational Medical Outcomes Partnership) is a Common Data Model (CDM) that allows for the systematic analysis of disparate observational databases. By transforming both EHR and claims data into the OMOP format, researchers can run the same analytical code across different datasets, making it much easier to conduct large-scale, multi-center studies.
Conclusion: Turn Fragmented Data Into Life-Saving Insights
The era of siloed healthcare data is over. To compete in modern life sciences and deliver high-value care, ehr claims data integration is no longer optional—it is the engine of innovation. The ability to see the full patient journey, from the first clinical symptom documented in an EHR to the final pharmacy fill recorded in a claim, is what will drive the next generation of medical breakthroughs.
At Lifebit, we provide the next-generation federated AI platform that makes this integration seamless and secure. Our Trusted Research Environment (TRE) and Trusted Data Lakehouse (TDL) allow you to harmonize disparate datasets and run advanced AI/ML analytics in real-time, all while keeping sensitive patient data protected. Whether you are conducting large-scale pharmacovigilance, building real-time evidence layers (R.E.A.L.), or optimizing population health management, we give you the tools to turn fragmented data into life-saving insights.
Ready to open up the full potential of your healthcare data and lead the charge in the data-driven healthcare revolution?

