Beginner’s Guide to Clinical Data Interoperability

Clinical Data Interoperability: How to Fix Healthcare’s $2.6 Trillion Data Crisis
Clinical data interoperability is the ability of different healthcare systems to exchange, integrate, and use patient information seamlessly—regardless of where that data originated. Without it, clinicians make decisions without complete patient histories, leading to duplicate tests, medication errors, and avoidable hospitalizations.
What Clinical Data Interoperability Enables:
- Unified patient records across hospitals, clinics, pharmacies, and labs
- Real-time data access for providers at the point of care
- Reduced costs by eliminating duplicate tests and procedures
- Improved outcomes through comprehensive treatment histories
- Regulatory compliance with CMS, TEFCA, and USCDI standards
The cost of not solving this is staggering. The U.S. healthcare system wastes an estimated $265 billion annually on administrative complexity and fragmented care coordination alone. Two out of three older Americans live with at least two chronic conditions, and treating people with multiple chronic conditions accounts for an estimated 66% of US healthcare costs. Yet less than half of hospitals integrate external data they receive into individual patient records. Just 23% of physicians say it’s “very easy” to use outside information, and only 8% find it easy to use data from different EHR systems. Meanwhile, the U.S. interoperability rate sits at 59.8%—far behind Estonia (99.1%), Finland (98.9%), and Denmark (98.2%).
The problem isn’t a lack of data. It’s that healthcare data remains trapped in silos—scattered across EHRs, claims systems, labs, wearables, dental records, and social care databases. When a patient moves from primary care to a specialist to a hospital, their data often doesn’t follow. The result? Fragmented care, preventable errors, and billions in wasted spending. This “data crisis” isn’t just a financial burden; it is a patient safety issue. When a physician cannot see a patient’s full medication list or recent lab results from an out-of-network facility, the risk of adverse drug events and misdiagnosis skyrockets.
That’s why federal initiatives like FHIR (Fast Healthcare Interoperability Resources), USCDI (United States Core Data for Interoperability), and TEFCA (Trusted Exchange Framework and Common Agreement) are pushing the industry toward standardized, secure data exchange. National networks and health information exchanges are building the infrastructure. Tools like REDCap’s Clinical Data Interoperability Services (CDIS) are enabling researchers to pull structured EHR data into studies. And by 2026, CMS will require FHIR APIs and expanded data standards for providers and payers.
But technology alone won’t fix this. Success requires coordination across vendors, providers, payers, and patients—plus the right platforms to harmonize, analyze, and act on data in real time. We must move beyond simple data transmission to true semantic interoperability, where the meaning of the data is preserved across systems.
I’m Maria Chatzou Dunford, CEO and Co-founder of Lifebit, where we help global health organizations solve clinical data interoperability challenges by enabling secure, federated analysis across fragmented datasets without moving data. With over 15 years in computational biology, AI, and health-tech, I’ve seen how the right infrastructure can turn siloed data into life-saving insights.
What is Clinical Data Interoperability and Why Does It Matter?
At its heart, clinical data interoperability is about making sure that a patient’s story isn’t missing its most important chapters just because they changed doctors or moved across state lines. In our current system, health data is often locked in digital “walled gardens.” This creates a paradox: health data is so sensitive we are afraid to share it, yet the lack of sharing causes direct harm through poorer outcomes and bloated costs.
To understand the depth of the challenge, we must look at the four levels of interoperability as defined by HIMSS:
- Foundational Interoperability: The most basic level, where one system can send data and another can receive it. The receiving system does not necessarily need to interpret the data.
- Structural Interoperability: This defines the format and syntax of the data exchange (e.g., the layout of the message). It ensures that the data can be interpreted at the field level.
- Semantic Interoperability: This is the “holy grail.” It ensures that the two systems can exchange information and use the information that has been exchanged. It relies on common coding systems (like LOINC or SNOMED CT) so that a “blood pressure” reading in one system is recognized exactly as such in another.
- Organizational Interoperability: This involves the legal, policy, and social components that allow organizations to trust each other and exchange data securely across different business processes.
When we achieve true health data interoperability, we move from a siloed view of a person—where they are a “patient” in one system, a “member” in a health plan, and a “consumer” in an app—to a holistic, 360-degree view. This is critical as populations age. With 66% of US healthcare costs tied to chronic conditions, we simply cannot afford to keep clinicians in the dark.
However, the road to this connectivity is paved with clinical challenges in health data standardisation. Different hospitals might use different codes for the same lab test, or one system might record a patient’s allergy in a way that another system can’t interpret. Without a common language, the data is just noise. For example, if one system uses a local code for “Type 2 Diabetes” and another uses the ICD-10 code E11.9, a search for diabetic patients might miss half the population unless the systems are semantically aligned.
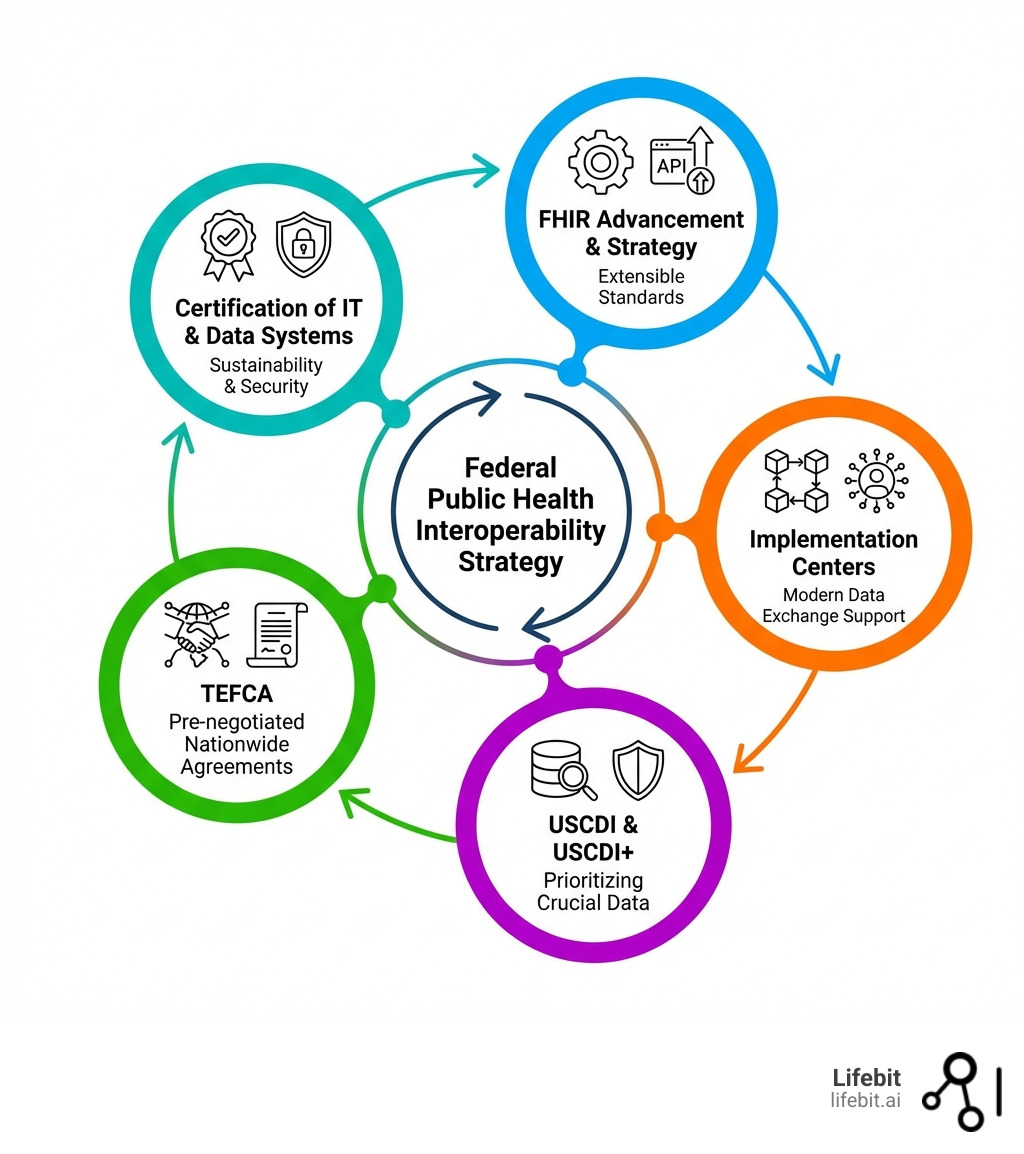
The Federal Strategy: FHIR, USCDI, and TEFCA Explained
To stop this digital Babel, the U.S. government has rolled out a multi-layered strategy. Think of it as building a nationwide highway system for data.
- Fast Healthcare Interoperability Resources (FHIR): This is the language we speak on the highway. Developed by Health Level Seven (HL7) International, FHIR uses “resources” (like Patient, Observation, or Medication) and modern APIs to make data exchange as easy as browsing a website. Unlike older standards, FHIR is designed for the mobile age, allowing developers to build apps that can plug into any EHR.
- United States Core Data for Interoperability (USCDI): This is the cargo we carry. It’s a standardized set of health data classes (like “Immunizations” or “Vital Signs”) that must be available for nationwide exchange. USCDI sets the minimum baseline for what data must be shareable to support patient care.
- TEFCA (Trusted Exchange Framework and Common Agreement): These are the rules of the road. TEFCA establishes a floor for interoperability across the country by creating Qualified Health Information Networks (QHINs) that can talk to each other. In late 2023, the first QHINs—including Epic Nexus, eHealth Exchange, and Health Gorilla—were officially designated, marking a massive milestone for nationwide connectivity.
By leveraging a hie health information exchange, providers can finally stop faxing records and start querying for patient data in real-time. If you want to define hie simply: it’s the electronic movement of health-related information among organizations.
How USCDI Version 6 and FHIR APIs Drive Clinical Data Interoperability
We are currently moving toward more granular and useful data sets. What is health data standardisation if not an evolving process? USCDI Version 6 is a massive leap forward. It expands the required data elements to include:
- Facility Information: Knowing exactly where care was delivered, which is vital for tracking outbreaks or auditing care quality.
- Unique Device Identifier (UDI): Crucial for tracking implants, pacemakers, or medical devices in the event of a recall.
- Portable Medical Orders: Such as POLST (Physician Orders for Life-Sustaining Treatment), ensuring a patient’s end-of-life wishes are respected across different care settings.
- Clinical Notes: Moving beyond just data points to include the narrative context of a physician’s assessment.
These advancements come with health data standardisation technical challenges. For example, many Long-Term Post-Acute Care (LTPAC) providers use EHRs that aren’t ONC-certified, making it expensive to adopt these new standards. However, with the CMS deadline for FHIR APIs set for July 2026, the industry is under pressure to modernize fast. This mandate will require payers to implement a Patient Access API, a Provider Access API, and a Payer-to-Payer API, ensuring that data follows the patient even when they change insurance plans.
Breaking the Barriers: Why 40% of Hospital Data is Still Lost
Despite the hype, we have a long way to go. A JAMA Open Network study revealed that only 23% of physicians found it “very easy” to use outside information. Even worse, only 8% said it was easy to use information from different EHR systems.
Why is this happening? One major reason is “Information Blocking.” Historically, some vendors and providers intentionally made it difficult to export data to keep patients within their own network. The 21st Century Cures Act has made this illegal, but the technical and cultural remnants of these silos remain. Furthermore, even when data is exchanged, it often isn’t integrated. It might arrive as a messy PDF that a doctor has to scroll through, rather than being neatly filed into the patient’s digital chart. This is why harmonizing disparate electronic health records is so vital—it’s the difference between having data and having insight.
Another barrier is the “Semantic Gap.” While two systems might both use FHIR, they might use different terminologies within those FHIR resources. One might use SNOMED CT for a diagnosis, while another uses ICD-10. Without a robust mapping layer, the receiving system cannot “understand” the data it just received. This leads to the “click fatigue” and physician burnout that plagues modern medicine.
As shown in the Black Book Research report, the U.S. is lagging behind international peers. While countries like Estonia have near-universal data exchange, the U.S. is still fighting physician burnout caused by fragmented records.
Overcoming Challenges in Clinical Data Interoperability for LTPAC and Dentistry
Two sectors that are notoriously non-interoperable are dentistry and Long-Term Post-Acute Care (LTPAC).
In dentistry, only 42% of providers can enter information into a patient’s general medical record via their EHR. This silo is dangerous; oral health is deeply linked to systemic issues like diabetes and heart disease. For instance, periodontal disease can exacerbate glycemic control in diabetic patients, yet most endocrinologists have no visibility into their patients’ dental health.
Similarly, LTPAC providers (like nursing homes) often struggle with resource needs and workflow integration. When an elderly patient is discharged from a hospital to a skilled nursing facility, the transfer of care is often fraught with missing information regarding medication changes or wound care instructions. To help, our clinical data interoperability complete guide suggests aligning new USCDI elements with existing Medicare-required assessments like MDS 3.0 to avoid duplicative data entry and reduce the burden on overworked staff.
The CMS Interoperability Framework: A Roadmap to 2026
The CMS Interoperability Framework isn’t just a suggestion—it’s a call to action. It focuses on five key pillars:
- Patient Access & Empowerment: Patients should be able to access their structured and unstructured data through apps without needing a new login for every portal.
- Provider Access & Delegation: Doctors should have full access to treatment histories, and vendors should be able to query data on their behalf.
- Data Availability & Standards: This includes moving to USCDI v3 and ensuring lab results and chart notes are shared in real-time.
- Network Connectivity: Using a national directory to find where a patient has been treated.
- Security & Trust: Achieving HITRUST certification to ensure data stays safe.
By following healthcare data integration standards, networks can become “CMS-Aligned,” proving they meet the highest bars for transparency and performance. For a deeper dive into how these systems work, check out our ehrs complete guide.
Advanced Tools for Research: REDCap CDIS and Real-Time Analytics
Interoperability isn’t just for doctors—it’s for researchers, too. Tools like REDCap’s Clinical Data Interoperability Services (CDIS) are game-changers. CDIS uses FHIR and OAuth2 to pull structured data directly from major EHR systems into research projects, reducing the need for manual data entry and the errors that come with it.
There are two main ways this works:
- Clinical Data Pull (CDP): Ideal for prospective studies (like clinical trials), it pulls data in real-time or at set intervals. This allows researchers to monitor patient safety and trial endpoints with unprecedented speed.
- Clinical Data Mart (CDM): Best for retrospective studies, it fetches bulk data for a list of patients over a specific date range, enabling large-scale population health studies.
However, a major hurdle remains: FHIR was designed for exchange, not analytics. FHIR bundles are complex JSON files with deeply nested structures. To make them useful for longitudinal records or machine learning models, we often need to “flatten” them into tables or map them to a common data model like OMOP (Observational Medical Outcomes Partnership). This is where health data harmonization complete guide principles and data integration standards healthcare guide become essential for any data science team.
Expanding Clinical Data Interoperability to Wearables and SDOH
The future of care lives outside the hospital. We need to integrate Social Determinants of Health (SDOH)—like housing stability, transportation access, and food security—and data from wearables. Research shows that clinical care only accounts for about 20% of health outcomes, while SDOH and behavioral factors account for the remaining 80%.
Initiatives like the Gravity Project are working to standardize SDOH data so it can be used in clinical decision-making. For example, if a physician knows a patient lacks reliable transportation, they can coordinate a telehealth visit or a home-based lab draw. Meanwhile, the CMS ACCESS model encourages using wearable device data to monitor patients with chronic conditions like heart failure or COPD in real-time.
Bridging these gaps requires data harmonization services bridging the gap between disparate datasets and ehr claims integration. At Lifebit, we advocate for a federated analysis approach. Instead of moving sensitive patient data into a central warehouse—which creates security risks and data sovereignty issues—we bring the analysis to the data. This allows researchers to query diverse datasets across the globe while the data remains securely behind the original organization’s firewall. This is the only way to achieve the scale needed for precision medicine while maintaining the highest standards of patient privacy.
Frequently Asked Questions about Clinical Data Interoperability
What are the primary barriers to achieving seamless health data exchange?
The biggest barriers are data silos, fragmented records, and a lack of financial incentives for vendors to play nice with each other. Technically, the challenge lies in converting “unstructured” data (like doctor’s notes) into “structured” data that systems can understand. High costs for small providers to upgrade to ONC-certified systems also remain a hurdle. Additionally, the lack of a National Patient Identifier in the U.S. makes patient matching across different systems a complex and error-prone process.
How does USCDI Version 6 expand data elements for post-acute care?
USCDI v6 adds critical elements for the LTPAC sector, including Facility Information, Unique Device Identifiers (UDI), and Portable Medical Orders. It also focuses on cognitive and functional assessments, which are vital for managing care transitions for older adults moving between hospitals and skilled nursing facilities. By standardizing these elements, we ensure that a patient’s functional status (e.g., their ability to walk or perform daily tasks) is communicated clearly to the next care team.
What role do TEFCA QHINs play in nationwide data connectivity?
Qualified Health Information Networks (QHINs) act as the backbone of nationwide exchange. Under TEFCA, these networks agree to a common set of technical and legal rules. This means a provider in California can securely query a patient’s records from a hospital in New York without having to set up a one-to-one connection. It creates a “network of networks” that simplifies the legal and technical hurdles of data sharing.
What is the difference between Interoperability and Integration?
Interoperability is the ability of two or more systems to exchange and use information. Integration is the process of connecting these systems so they work together as a unified whole. You can have interoperability (the ability to send a file) without integration (the file being automatically updated in the patient’s chart). True clinical success requires both.
How will AI impact clinical data interoperability?
AI and Natural Language Processing (NLP) are crucial for tackling the “unstructured data” problem. Much of the most valuable clinical information is buried in free-text notes. AI can extract structured data from these notes, mapping them to standards like FHIR, thereby making previously “dark data” interoperable and searchable.
Conclusion
The era of fragmented healthcare is coming to an end. As we move toward 2026, the push for clinical data interoperability will only intensify. By adopting standards like FHIR and USCDI, and leveraging frameworks like TEFCA, we can finally build a system that puts the patient at the center.
At Lifebit, we believe that the most sensitive data in the world should be the most useful. Our federated AI platform allows researchers and public health agencies to access and analyze global biomedical data securely, ensuring that privacy doesn’t have to come at the cost of progress.
Secure your research with Lifebit’s federated AI platform and help us turn broken data into a healthier future for everyone.

