Crunching Numbers, Saving Lives: Your Guide to Health Data Analytics

How Health Data Analytics Saves Lives — and $1.2 Trillion in Healthcare Waste
Health data analytics is the practice of turning raw patient information—EHRs, lab results, genomic sequences, wearables, insurance claims—into actionable insights that improve care, cut costs, and save lives. It uses statistical methods, machine learning, and visualization tools to uncover patterns, predict outcomes, and guide clinical decisions in real time.
What it does:
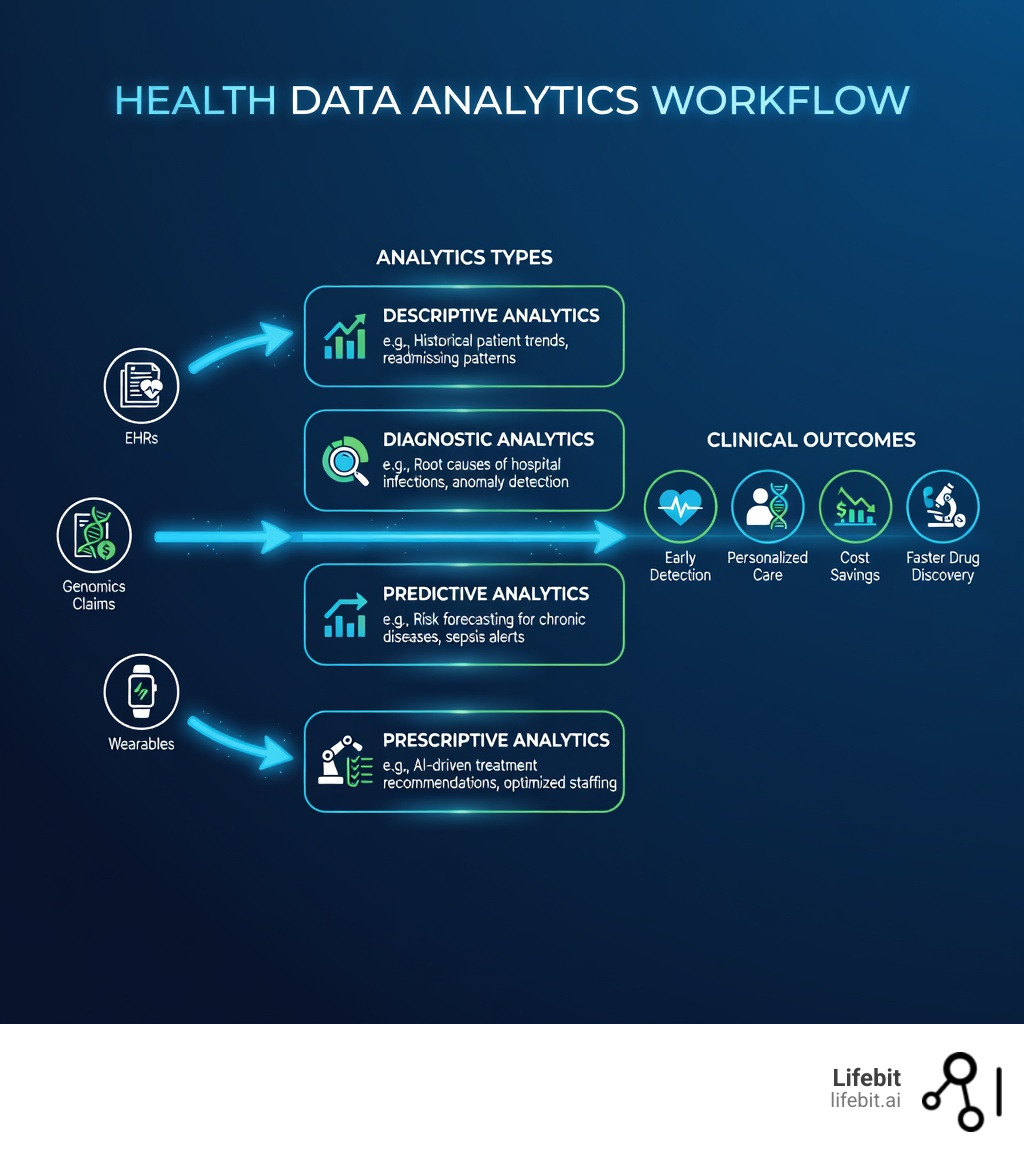
- Descriptive analytics shows what happened (e.g., patient volumes, readmission rates)
- Diagnostic analytics explains why it happened (e.g., root causes of infection spikes)
- Predictive analytics forecasts what’s next (e.g., who’s at risk of septic shock or diabetes)
- Prescriptive analytics recommends what to do (e.g., personalized treatment plans, staffing adjustments)
The healthcare industry is drowning in data—petabytes of it—from electronic health records, genomic sequences, IoT sensors, and insurance claims. But most of it sits locked in silos, unstructured, unusable, and untapped. Meanwhile, healthcare costs are skyrocketing, chronic diseases are rising, and clinicians are overwhelmed. Health data analytics is the bridge between that chaos and better outcomes.
Why it matters now:
Healthcare jobs tied to data—health information technologists, data scientists, operations research analysts—are projected to grow 16% to 36% between 2023 and 2033, far faster than most other fields. The U.S. healthcare analytics market alone is expected to surpass $31 billion by 2022. Hospitals, payers, pharma companies, and public health agencies are racing to adopt analytics—not just to stay competitive, but to survive the shift to value-based care, where outcomes and efficiency matter more than volume.
The payoff is massive. Early disease detection. Faster, more accurate diagnoses. Personalized medicine. Smarter resource allocation. Faster drug development. Lower costs. Fewer errors. Lives saved.
But getting there isn’t easy. You’re dealing with privacy risks, cybersecurity threats, messy unstructured data, and systems that don’t talk to each other. Add in regulations like GDPR and HIPAA, and it’s no wonder many organizations struggle to move from raw data to real insight.
That’s what this guide is for. Whether you’re a pharma exec trying to accelerate clinical trials, a public health leader tracking disease outbreaks, or a hospital administrator optimizing operations, you’ll learn what health data analytics actually does, how it works, and how to overcome the barriers holding you back.
I’m Maria Chatzou Dunford, CEO and Co-founder of Lifebit, a federated biomedical data platform that enables secure, real-time health data analytics across 275M+ patient records globally. Over 15 years, I’ve built computational tools for precision medicine, contributed to Nextflow, and helped pharma and public sector organizations open up insights from siloed genomic and clinical data—without moving it.
Simple health data analytics word guide:
Why Health Data Analytics is the $31 Billion Shift You Can’t Ignore
At its heart, health data analytics is about uncovering patterns and insights from raw healthcare data like patient histories, bloodwork, and genetic trackers to help healthcare providers determine the best course of treatment. We are moving away from “gut feeling” medicine toward evidence-based, data-driven decisions.
The current healthcare landscape is facing a perfect storm. Costs are rising, populations are aging with multiple chronic conditions (multimorbidity), and there is an urgent need to improve the quality of care while reducing waste. Rapid innovation in the use of analytics and data-driven technology is having a profound impact on our society, and consequently, our health and healthcare system.
The Economic Imperative: From Volume to Value
The primary driver behind the $31 billion market explosion is the global shift toward Value-Based Care (VBC). In traditional fee-for-service models, providers were paid based on the volume of tests and procedures. Today, payers (like CMS in the U.S. or national health systems in Europe) are increasingly tying reimbursement to patient outcomes.
Without robust health data analytics, surviving this transition is impossible. Organizations must be able to prove that their interventions are effective, which requires tracking longitudinal patient data over years, not just days. This economic pressure is forcing hospitals to treat data as a strategic asset rather than a byproduct of administration.
Why Health Data Analytics Is Urgent
The “Meaningful Use” era of the 2010s flooded hospitals with Electronic Health Records (EHRs). Now, the challenge is moving from “meaningful use” to “meaningful analytics.” We need these tools because:
- Faster Clinical Decisions: In emergencies, data analytics can improve ER performance and reduce overutilization of unnecessary lab tests. Real-time dashboards can alert staff to potential bottlenecks before they impact patient safety.
- Lower Costs: By identifying wasted resources in insurance claims or optimizing hospital supply chains, organizations can save millions. For example, predictive maintenance on expensive imaging equipment like MRIs can prevent costly downtime.
- Improved Population Health: Tracking disease prevention methods across large populations helps public health agencies act before an outbreak spreads. This involves analyzing social determinants of health (SDOH) to understand why certain neighborhoods have higher rates of asthma or heart disease.
- Patient-First Care: It allows for a shift from reactive therapy to proactive, data-driven preventive approaches. By analyzing wearable data, clinicians can intervene when a patient’s heart rate variability or glucose levels show early signs of distress, long before a hospital visit is required.
The 4 Pillars of Analytics: From Hindsight to Foresight
To master health data analytics, we must understand that not all “analysis” is the same. Researchers often categorize analytics into four distinct levels, each adding more value and complexity to the decision-making process. This progression is often referred to as the “Analytics Maturity Model.”
| Analytics Type | Question Answered | Healthcare Example |
|---|---|---|
| Descriptive | What happened? | Calculating the hospital readmission rate for the last quarter. |
| Diagnostic | Why did it happen? | Identifying that a spike in infections was linked to a specific ward or protocol. |
| Predictive | What will happen? | Forecasting which patients are at high risk for developing Type 2 Diabetes. |
| Prescriptive | What should we do? | Suggesting a specific drug dosage based on a patient’s genetic profile. |
Source: Khalifa M. Health Analytics Types, Functions and Levels
Deep Dive: Diagnostic Analytics and Root Cause Discovery
While descriptive analytics tells you that 15% of your patients are being readmitted within 30 days, diagnostic analytics digs into the “why.” This involves data mining and correlations. For instance, a diagnostic study might reveal that readmissions are 3x higher for patients who live in “food deserts” or those who were not provided with a follow-up telehealth appointment within 48 hours of discharge. By identifying these root causes, healthcare administrators can move from observing problems to solving them through targeted social interventions or policy changes.
Predictive Analytics: Stop Disease Before It Starts
Predictive analytics is often called “medicine’s attempt at a crystal ball.” By using historical and real-time data, we can forecast future events and intervene early. For example, research on population-level prediction of Type 2 Diabetes has shown that we can identify high-risk individuals from insurance claims data long before they show clinical symptoms.
In acute care, machine learning algorithms can detect septic shock nearly 28.2 hours before clinical onset. Sepsis is a leading cause of hospital death, and every hour of delayed treatment increases mortality risk by nearly 8%. Predictive models analyze vital signs, white blood cell counts, and even the subtle cadence of a patient’s breathing to alert rapid response teams before organ failure begins.
Prescriptive Analytics: The Frontier of Clinical Decision Support
This is the “gold standard.” Prescriptive analytics doesn’t just predict a problem; it suggests the solution. It uses advanced technologies like AI and machine learning to recommend the best course of action. In a hospital setting, this might look like an automated staffing tool that suggests moving three nurses from the surgical wing to the emergency department because a surge in respiratory cases is predicted for the next six hours.
In clinical practice, prescriptive analytics powers Clinical Decision Support (CDS) systems. When a doctor prescribes a medication, the system cross-references the patient’s entire medical history, current medications, and even genetic markers to suggest a different dosage or a different drug entirely to avoid an adverse reaction. This level of analytics turns the EHR from a digital filing cabinet into an active member of the care team.
Precision Medicine: How Big Data Cuts Drug Discovery Time in Half
The potential of big data in healthcare is unlimited. One of the most exciting frontiers is Precision Medicine—the shift from a “one-size-fits-all” approach to tailoring treatments to individual characteristics like genetics, environment, and lifestyle.

By integrating genomic sequences with clinical EHR data, we can identify which patients will respond best to specific therapies. This is particularly vital in oncology research and the treatment of rare diseases.
The Role of Multi-Omics in Modern Research
To truly understand a disease, we cannot look at DNA alone. Health data analytics now encompasses “multi-omics”—the combination of genomics (DNA), transcriptomics (RNA), proteomics (proteins), and metabolomics (metabolites). Analyzing these layers together allows researchers to see the full biological picture. For example, in breast cancer research, multi-omic analysis has helped identify specific molecular subtypes that require vastly different chemotherapy regimens. Lifebit’s federated AI platform powers this by enabling researchers to access and analyze massive, multi-omic datasets securely, ensuring that sensitive patient data stays protected while still delivering breakthroughs.
Speeding Up Drug Development and Clinical Trials
Traditional drug development is slow and expensive, often taking 10-12 years and costing over $2 billion per drug. Health data analytics accelerates this by:
- Streamlining Clinical Trials: Identifying the right patient cohorts faster by searching global EHR databases for specific biomarkers, reducing recruitment time from months to weeks.
- Predicting Drug Interactions: Using AI to model how new compounds will react in the human body, potentially identifying toxic side effects before a single human dose is administered.
- Real-World Evidence (RWE): Analyzing how drugs perform in the general population after they are released. This “Phase IV” data is crucial for identifying new opportunities for precision medicine and understanding how a drug affects diverse populations that may have been underrepresented in initial trials.
Advancing Public Health and Health Equity
Analytics can be a powerful tool for social justice. By including social determinants of health (SDOH)—like zip codes, income, and education—public health agencies can identify and reach at-risk groups that are often overlooked. For instance, analytics can map “pharmacy deserts” where elderly populations lack access to life-saving medications, allowing cities to deploy mobile clinics. In Canada, for instance, data collection for Indigenous populations follows OCAP® principles (Ownership, Control, Access, and Possession) to ensure that data is used to empower communities rather than marginalize them, ensuring that the benefits of big data are shared equitably.
Stop Data Silos: 4 Barriers Killing Your Analytics Strategy
If analytics is so powerful, why isn’t every hospital using it perfectly? The truth is that implementing these systems is incredibly difficult. We face four major problems, as detailed in research on big data challenges in healthcare:
- Privacy and Security: Hospitals are prime targets for cybercriminals. Protecting patient rights while allowing data access is a delicate balance. The rise of ransomware attacks on healthcare systems has made many organizations hesitant to share data, even for research purposes.
- Data Quality and “Messiness”: Health data is notoriously messy. It comes from different sources, may be incomplete, or contains errors. A patient’s name might be spelled three different ways across three different systems, or a lab result might be recorded in different units of measurement.
- Interoperability: Different systems (EHRs, lab systems, wearable apps) often speak different “languages.” Without a unified standard, data remains trapped in silos, unable to be aggregated for high-level analysis.
- Unstructured Data: Roughly 80% of medical data is unstructured free-text (like doctor’s notes, discharge summaries, and pathology reports). Traditional databases cannot “read” this information. We need advanced Natural Language Processing (NLP) to extract meaning from these notes and make this data computable.
The Technical Solution: FHIR and the 21st Century Cures Act
To solve the interoperability crisis, the industry is moving toward FHIR (Fast Healthcare Interoperability Resources). FHIR is a standard that allows different healthcare applications to exchange data via APIs, much like how different travel websites can pull flight data from various airlines.
In the United States, the 21st Century Cures Act has made “information blocking” illegal, forcing EHR vendors to provide patients and providers with easy, digital access to their health information. This regulatory push is finally breaking down the silos that have hindered health data analytics for decades.
Building Trust: Standards and Governance for Safe Data Use
Beyond technical standards, we rely on frameworks like ISO/HL7 27931. These international standards provide a common language for data exchange, ensuring that a blood test result from one lab is understood by a specialist in another city.
Strong data governance is also essential. This involves setting clear rules for who can access data, for what purpose, and how it is de-identified to protect privacy. Government bodies, like the ONC in the US, play a critical role here by creating “interoperability roadmaps” that force different tech vendors to work together. Effective governance ensures that data is not just available, but also accurate, timely, and ethically sourced.
High Demand, $100k Salaries: Why Health Data is the Career of 2026
There has never been a better time to enter this field. Roles for medical registrars and health information technologists are projected to grow 16%, while demand for data scientists is expected to climb by 36%. This growth is driven by the realization that having data is useless without the talent to interpret it.
- Average Salary: A healthcare data analyst’s average annual base salary typically ranges from $89,437 to $103,691, with senior data scientists in pharma often exceeding $160,000.
- Technical Skills: You’ll need a handle on SQL for database management, Python or R for analysis, and tools like Tableau or PowerBI for data visualization. Familiarity with machine learning libraries like Scikit-learn or TensorFlow is increasingly required for advanced roles.
- Soft Skills: Communication is key. You aren’t just “crunching numbers”—you are telling a story that helps a doctor or a CEO make a life-or-death decision. You must be able to translate complex statistical findings into actionable clinical insights.
The Rise of the Clinical Data Scientist
A new hybrid role is emerging: the Clinical Data Scientist. These professionals possess both deep medical knowledge (often as former nurses or pharmacists) and advanced data science skills. They are the bridge between the IT department and the ICU, ensuring that the models built by engineers actually make sense in a high-pressure clinical environment. They understand the nuances of medical coding (ICD-10, SNOMED) and the realities of clinical workflows.
How to Get Started: Education and Certification
You don’t always need a PhD to start. Many professionals are upskilling through targeted programs:
- UBC Micro-certificate: A part-time technical program focusing on real-world cases and data science storytelling.
- McMaster Health Analytics: Offers flexible learning for healthcare professionals looking to transition into administrative or leadership roles.
- Bow Valley College Diploma: A 4-term program covering relational databases, data quality, and big data.
- Certifications: Earning credentials like the CompTIA Data+, the Certified Health Data Analyst (CHDA), or training through AHIMA in areas like data governance and interoperability can give you a major edge in a competitive job market.
Health Data Analytics: Your Top Questions Answered
How is health data analytics different from health informatics?
While they overlap, health informatics is generally about the systems and “plumbing”—how data is captured and moved within a clinical setting to help doctors. Health data analytics is about the “insights”—using that captured data to find patterns, improve business efficiency, and predict patient outcomes.
What’s the role of AI and IoT in health analytics?
AI (Artificial Intelligence) is the engine that allows us to process data at a scale humans can’t match. IoT (Internet of Things), such as wearable heart monitors or smart glucose patches, provides a constant stream of real-time data. Together, they allow for remote patient monitoring, moving care from the hospital to the home.
What are the key ethical issues in health data?
The biggest concerns are consent and bias. If an AI is trained on data that doesn’t include diverse populations, its “prescriptions” might be biased. We must also ensure that “secondary use” of data (using data collected for treatment for research instead) is done with the patient’s knowledge and protects their identity.
Conclusion: The Future is Federated
The future of healthcare is proactive, personalized, and data-driven. We are moving away from a world where data is locked in a single hospital’s basement toward a global network of “shared intelligence.”
However, we cannot simply move all the world’s patient data into one giant cloud—it’s too risky and legally complex. This is where Lifebit’s federated AI platform changes the game. By delivering secure, real-time access to global biomedical and multi-omic data through our Trusted Research Environment (TRE) and Real-time Evidence & Analytics Layer (R.E.A.L.), we allow for compliant research and pharmacovigilance without compromising privacy.
The revolution in health data analytics is a collective endeavor. By embracing standards, investing in skills, and utilizing secure technologies, we can ensure that every bit of data serves its highest purpose: saving a life.

