How AI Health Analytics is Changing the Game

Why Health Data Intelligence is the Key to Unlocking Real-Time Healthcare Insights
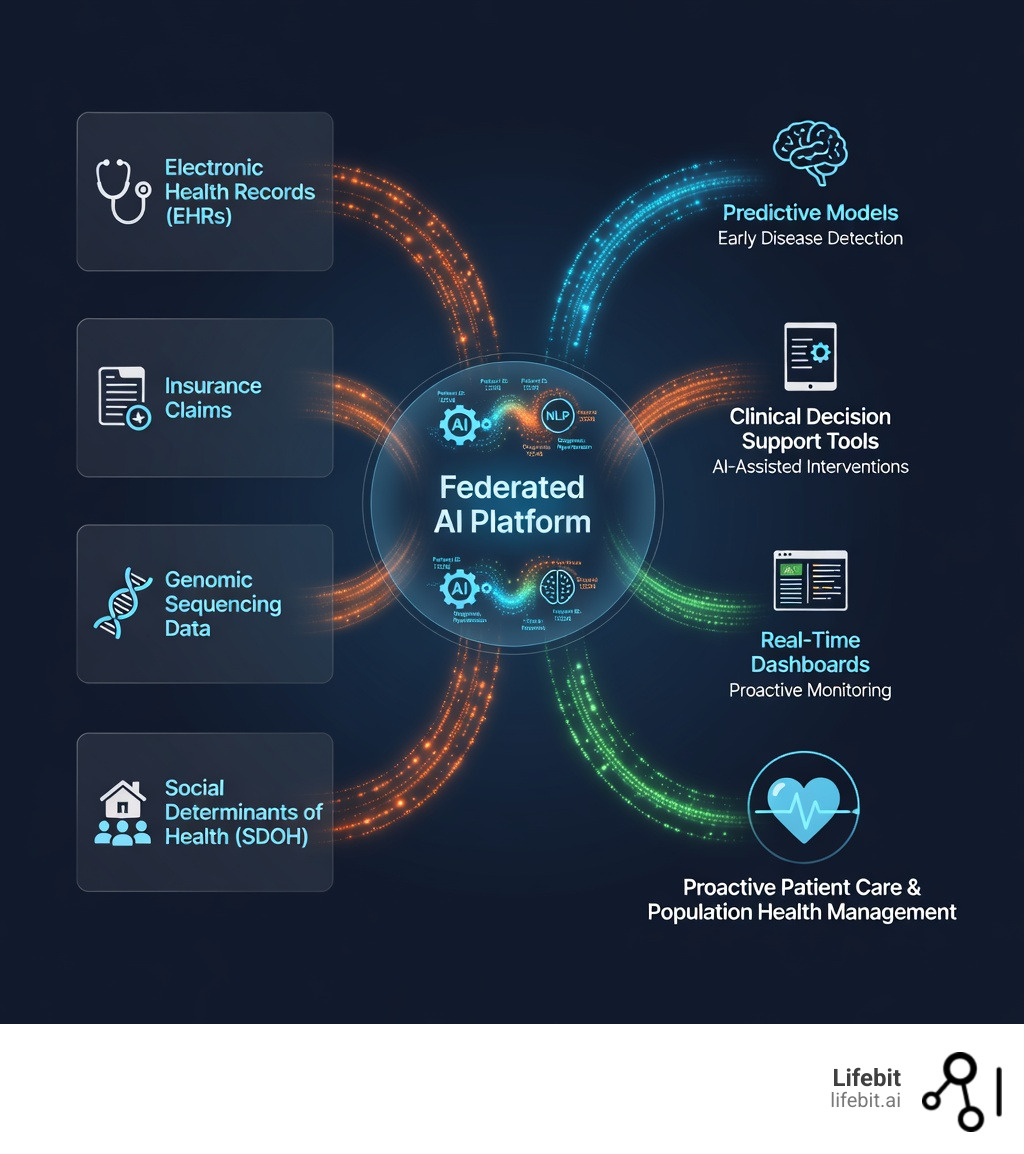
Health data intelligence is the practice of systematically collecting, integrating, and analyzing healthcare data from diverse sources—including electronic health records (EHRs), claims, genomics, pharmacy records, and social determinants of health (SDOH)—to generate actionable insights that improve patient outcomes, operational efficiency, and clinical decision-making. At its core, it transforms fragmented, siloed data into longitudinal patient records that power everything from predictive analytics and personalized medicine to fraud detection and population health management.
In the current landscape, healthcare generates approximately 30% of the world’s total data volume. However, a staggering 97% of that data goes unused because it is trapped in incompatible formats or isolated systems. Health data intelligence bridges this gap by creating a “single source of truth.” This involves not just moving data, but harmonizing it so that a blood pressure reading from a wearable device, a genomic sequence from a lab, and a clinical note from a specialist can all be analyzed together to provide a 360-degree view of the patient.
Key components of health data intelligence include:
- Data Integration: Unifying EHR, claims, genomics, imaging, and SDOH data into interoperable, longitudinal records that follow the patient across the entire care continuum.
- AI and Machine Learning: Leveraging natural language processing (NLP) to extract insights from unstructured clinical text (approximately 80% of EHR data), and deploying predictive models for early disease detection and risk stratification.
- Cloud and Federated Architecture: Enabling secure, scalable, in situ analytics across distributed data sources without centralizing sensitive patient information, which is critical for maintaining data sovereignty and compliance.
- Interoperability Standards: Using FHIR, SMART on FHIR, and OAuth 2.0 to connect disparate systems and ensure compliant, secure data access for researchers and clinicians alike.
- Real-Time Analytics: Supporting proactive care through tools like sepsis prediction (28.2 hours before onset), acute kidney injury forecasting (AUC 0.88), and AI-powered care manager workflows that deliver 5x efficiency gains.
Healthcare organizations today face a critical challenge: data silos prevent them from seeing the full patient picture. Hospitals, payers, researchers, and regulators struggle with fragmented systems, unusable data formats, and slow evidence generation—leading to missed care gaps, delayed interventions, and billions in preventable costs. Health data intelligence solves this by creating analysis-ready datasets, enabling value-based care, regulatory compliance, and AI-driven decision support at scale.
As Dr. Maria Chatzou Dunford, CEO and Co-founder of Lifebit, I’ve spent over 15 years building platforms that transform biomedical data into precision medicine breakthroughs—from co-founding Nextflow for genomic workflows to pioneering federated health data intelligence solutions trusted by pharmaceutical organizations and public sector institutions worldwide. In this guide, I’ll walk you through how AI-powered analytics is reshaping healthcare delivery and how your organization can harness this technology to accelerate discovery, improve patient outcomes, and reduce costs.
Health data intelligence terms to remember:
What is Health Data Intelligence and Why Your Organization Needs It Now
In the modern landscape, making decisions based on outdated or fragmented data isn’t just inefficient—it’s risky. Health data intelligence represents a paradigm shift from reactive treatment to proactive, evidence-based care. By creating longitudinal records that follow a patient across different providers and systems, we can finally see the “whole person,” rather than just a series of disconnected medical encounters.
Why do we need this now? Because the traditional model of managing data in isolated “homegrown” systems is failing under the weight of modern data complexity. Research shows that a professional health data intelligence platform’s total cost of ownership (TCO) is approximately four times lower than homegrown systems on a per member per month (PMPM) basis. Homegrown systems often suffer from “technical debt,” where the cost of maintaining old code and manual data cleaning outweighs the benefits of the insights generated.
Beyond cost, the complexity of modern medicine requires an Introduction to health care data analytics- an overview that accounts for more than just clinical notes. We must integrate Social Determinants of Health (SDOH)—factors like housing stability, transport access, and food security—which influence up to 80% of health outcomes. For example, a patient with diabetes may have perfect clinical care but fail to manage their condition because they live in a “food desert” without access to fresh produce. Health data intelligence identifies these patterns, allowing for social interventions that prevent medical crises.
When we combine clinical data with claims and pharmacy records, we move toward true value-based care (VBC). In a VBC model, providers are rewarded for keeping people healthy rather than just performing procedures. This requires a level of data precision that only an integrated intelligence platform can provide. For a deeper dive into the architecture behind these systems, check out our data intelligence platform ultimate guide.
How to Unify Fragmented Data Sources with Health Data Intelligence
The biggest hurdle in healthcare is that data doesn’t like to talk to other data. One system might use a specific ID for a patient, while another uses something entirely different. Furthermore, clinical terms are often recorded inconsistently; one doctor might write “Type 2 Diabetes,” while another uses a specific ICD-10 code. To solve this, we use data normalization and global standards to ensure semantic interoperability.
Interoperability is the name of the game. By leveraging standards like FHIR (Fast Healthcare Interoperability Resources) and SMART on FHIR, we allow different applications to “plug and play” with healthcare data securely. FHIR breaks down medical information into “resources”—such as Patients, Observations, and Medications—that can be easily exchanged via APIs. This isn’t just about technical plumbing; it’s about ensuring that when a researcher in London needs to analyze a cohort that includes data from New York or Singapore, the data looks and acts the same way, regardless of the underlying EHR system.
When setting up these integrations, security is paramount. We use API authorization protocols like OAuth 2.0 to ensure that only authorized systems can access sensitive records. This creates a secure “handshake” between data sources. For those looking to understand how these platforms compare and integrate, our data intelligence similar complete guide offers a comprehensive breakdown.

Leveraging AI for Health Data Intelligence
Did you know that approximately 80% of medical data in EHRs exists as unstructured free-text? These are the typed notes from doctors, discharge summaries, and pathology reports that traditional databases can’t “read.” Without AI, this information is effectively invisible to large-scale analysis.
This is where AI, specifically Natural Language Processing (NLP), becomes a superhero. NLP can scan millions of records in seconds to identify medications, adverse drug events, or symptoms that haven’t been formally coded yet. For instance, NLP can detect early signs of cognitive decline mentioned in clinical notes years before a formal diagnosis of Alzheimer’s is made. Generative AI is also stepping up, providing AI-powered summaries that can lead to a 5x gain in care manager efficiency during patient case reviews. Instead of hunting through hundreds of pages of notes, clinicians get a concise, accurate snapshot of the patient’s history. These ai-driven-insights are what turn “big data” into “smart data.”
Scaling Health Data Intelligence with Cloud and Federated Tech
The old way of doing things involved moving all your data into one giant “data warehouse.” In 2026, that’s often impossible due to privacy laws (like GDPR), data residency requirements, and the sheer size of the datasets. Genomic data alone can reach petabytes in scale, making it prohibitively expensive and slow to move.
The future is a federated architecture. Instead of moving the data to the analysis, we move the analysis to the data. This happens within a Trusted Research Environment (TRE) or a Secure Data Environment (SDE). This approach allows organizations to collaborate globally—across Europe, North America, and beyond—without the data ever leaving its home jurisdiction. This is a core component of a modern data intelligence platform, ensuring compliance with local laws while still allowing for global scientific breakthroughs. By using federated learning, models can be trained on diverse global populations, which significantly improves their accuracy and reduces demographic bias.
5 Ways AI-Powered Analytics Transforms Patient Care and Efficiency
The impact of health data intelligence isn’t just theoretical—it’s saving lives every day. By using predictive analytics, we can spot trouble before it starts, moving from a “break-fix” model of medicine to one that is truly preventive.
- Sepsis Detection: Sepsis is a leading cause of hospital mortality, often because it is diagnosed too late. Algorithms like TREWScore have achieved an ROC curve (AUC) of 0.83 for detecting septic shock. More importantly, it can identify at-risk patients a median of 28.2 hours before clinical onset. This “golden window” allows clinicians to administer antibiotics and fluids early, potentially reducing sepsis-related deaths by over 50%.
- Kidney Health: Acute Kidney Injury (AKI) is often a “silent killer” in hospital settings. Machine learning models can now predict AKI development within 7 days with an AUC of up to 0.88. By identifying these patients early, hospitals can adjust medication dosages and hydration levels, preventing permanent kidney damage and the need for costly long-term dialysis.
- Operational Efficiency: Health data intelligence isn’t just for clinical use; it’s for the business of healthcare. By analyzing order turnaround times and patient flow data, hospitals can reduce Emergency Department length-of-stay and optimize staffing levels. Predictive models can forecast patient admissions weeks in advance, allowing administrators to manage bed capacity more effectively.
- Care Coordination and Gap Closure: Automated workflows can identify “care gaps”—such as a patient with heart disease who has missed a vital screening or a child who is behind on vaccinations. The system can then alert the care team to reach out proactively. This ensures that no patient falls through the cracks of a complex healthcare system.
- Financial Performance and Fraud Detection: AI can detect Medicare fraud schemes by spotting patterns that human auditors would miss, such as “upcoding” or billing for services that were never rendered. Some of these schemes have been responsible for over $100 million in losses. By identifying these anomalies in real-time, payers can move from a “pay and chase” model to one of proactive prevention.
Reactive Care vs. Proactive Health Data Intelligence
| Feature | Reactive Care (The Old Way) | Proactive Intelligence (The New Way) |
|---|---|---|
| Data Source | Single EHR / Siloed | Longitudinal / Integrated |
| Sepsis Response | After organ dysfunction begins | 28+ hours before clinical onset |
| Patient View | Snapshot of current visit | 360-degree historical view |
| Efficiency | Manual chart review | AI-powered summaries (5x faster) |
| SDOH | Often ignored | Integrated via Z-codes and NLP |
| Decision Support | Based on general guidelines | Personalized to patient’s genetic profile |
For more on the science of these breakthroughs, see the research on Advancements in Predictive Medicine: NLRP3 Inflammasome Inhibitors and AI-Driven Predictive Health Analytics.
Practical Applications of Health Data Intelligence
We are seeing these tools used in diverse ways across the globe:
- Drug Discovery: AI models like Med-PaLM have achieved 92.6% agreement with clinicians, helping researchers identify new drug targets and predict how patients will respond to treatments. This can shave years off the drug development lifecycle.
- Personalized Medicine: In oncology, we use genomics and clinical data to tailor treatments to a patient’s specific genetic profile. This ensures that patients receive the most effective therapy with the fewest side effects.
- Population Health: Public health agencies use these platforms to segment populations by risk, helping to address health inequalities by directing resources to the most vulnerable communities.
- Chronic Disease Management: Real-time monitoring from wearables can alert doctors to anomalies in patients with heart failure or diabetes before a crisis occurs, reducing hospital readmissions.
Overcoming Security, Privacy, and Equity Barriers
We can’t talk about health data intelligence without talking about trust. Patient data is the most sensitive data there is, and any breach can have devastating consequences for both patients and institutions. Our systems must be “secure by design,” meeting rigorous standards like HIPAA in the US and GDPR in Europe.
To maintain this trust, many organizations are adopting the “Five Safes” framework: Safe People (authorized researchers), Safe Projects (approved research goals), Safe Settings (secure environments like TREs), Safe Data (de-identified information), and Safe Outputs (ensuring results don’t reveal identities). This multi-layered approach ensures that data can be used for the public good without compromising individual privacy.
One of the most exciting emerging trends is machine unlearning. Just as GDPR grants a “right to be forgotten,” we are developing ways to “teach” AI models to forget specific data points if a patient withdraws consent, without having to retrain the entire model from scratch. This is a vital part of modern data-inteligence, allowing for dynamic consent management in a world where patient preferences can change over time.
We also have a responsibility to ensure data equity. If our AI is only trained on data from one demographic, it won’t work for everyone, potentially exacerbating existing health disparities. We are actively working to include diverse datasets from underrepresented populations and use “Z-codes” to track social determinants of health. By auditing our algorithms for bias and ensuring that our training data is representative of the global population, we can ensure that health data intelligence helps close the gap on health inequalities rather than widening them.
Frequently Asked Questions about Health Data Intelligence
How does health data intelligence reduce the total cost of ownership (TCO)?
By moving to a unified, cloud-native platform, organizations can eliminate the need for multiple “point solutions” (like separate business intelligence tools, data warehouses, and NLP engines). This reduces the burden on internal IT teams, simplifies vendor management, and lowers infrastructure costs. In fact, research shows that professional platforms can be up to four times cheaper than building and maintaining a homegrown system, which often requires a large team of specialized engineers to keep running.
What is the role of FHIR and SMART standards in data integration?
These are the universal languages of healthcare data. FHIR provides a standard format for exchanging data, while SMART allows developers to create apps that run across different healthcare systems without needing to rewrite code for each one. Together, they ensure that your health data intelligence tools are “EHR-agnostic,” meaning they work regardless of whether your hospitals use Epic, Cerner, or any other electronic health record system. This prevents “vendor lock-in” and allows for faster innovation.
How does this technology help address health inequalities and SDOH?
By integrating Social Determinants of Health (SDOH) data—like zip code, transport access, and nutrition—into clinical records, we can identify which populations are at the highest risk for poor outcomes. This allows policymakers and providers to intervene with social support (like food vouchers or transportation assistance) before medical issues escalate. For example, if data shows a high rate of asthma in a specific neighborhood, intelligence tools can help link that to local air quality data, prompting public health interventions at the source.
Can health data intelligence work with legacy systems?
Yes. Modern intelligence platforms are designed to sit “on top” of legacy systems. Using specialized connectors and ETL (Extract, Transform, Load) processes, data can be pulled from older databases, normalized into FHIR standards, and then analyzed alongside modern data sources. This allows organizations to modernize their data strategy without having to undergo a costly and disruptive “rip and replace” of their existing core systems.
Conclusion
The era of making healthcare decisions in the dark is over. Health data intelligence is moving us toward a future of “preemptive medicine,” where we don’t just treat disease—we prevent it. By leveraging real-time evidence and global biomedical data, we can provide every patient with the personalized care they deserve.
At Lifebit, we are proud to lead this charge. We provide a next-generation federated AI platform that enables secure, real-time access to global biomedical and multi-omic data. Whether you are in biopharma, government, or public health, our platform is designed to harmonize complex data and power compliant research at scale.
Ready to lead the revolution? Secure your data future with a Trusted Data Marketplace and find what’s possible when your decisions are powered by the world’s most advanced health intelligence.

