What You Need to Know About Singapore Healthcare Data

Singapore Healthcare Data: Access 5.8M Records to Solve Asian Health Challenges
Singapore healthcare data offers one of the most complete, high-quality windows into a modern, high-income health system in Asia — and the numbers tell a striking story. As a nation of approximately 5.8 million people, Singapore serves as a unique “living laboratory” for health researchers. The data is characterized by its high resolution, longitudinal nature, and multi-ethnic composition, representing the three major Asian ethnic groups: Chinese, Malay, and Indian. This makes the data exceptionally valuable for understanding disease phenotypes and treatment responses across the broader Asian continent.
Here are the key facts at a glance:
| Indicator | Value |
|---|---|
| Population (2023) | 5,789,090 |
| WHO Region | Western Pacific |
| Income Level | High Income (HIC) |
| Current Health Expenditure | 5.57% of GDP (2021) |
| Projected Health Expenditure (2030) | ~US$43 billion (5.9% of GDP) |
| Elderly population over 65 (current) | 10.7% |
| Elderly population over 65 (by 2030) | Over 25% |
| Residents with hypertension or hyperlipidaemia | ~1 in 3 |
| Global health ranking (Legatum Prosperity Index, 2023) | 1st out of 104 countries |
| Annual medical tourists | ~500,000 |
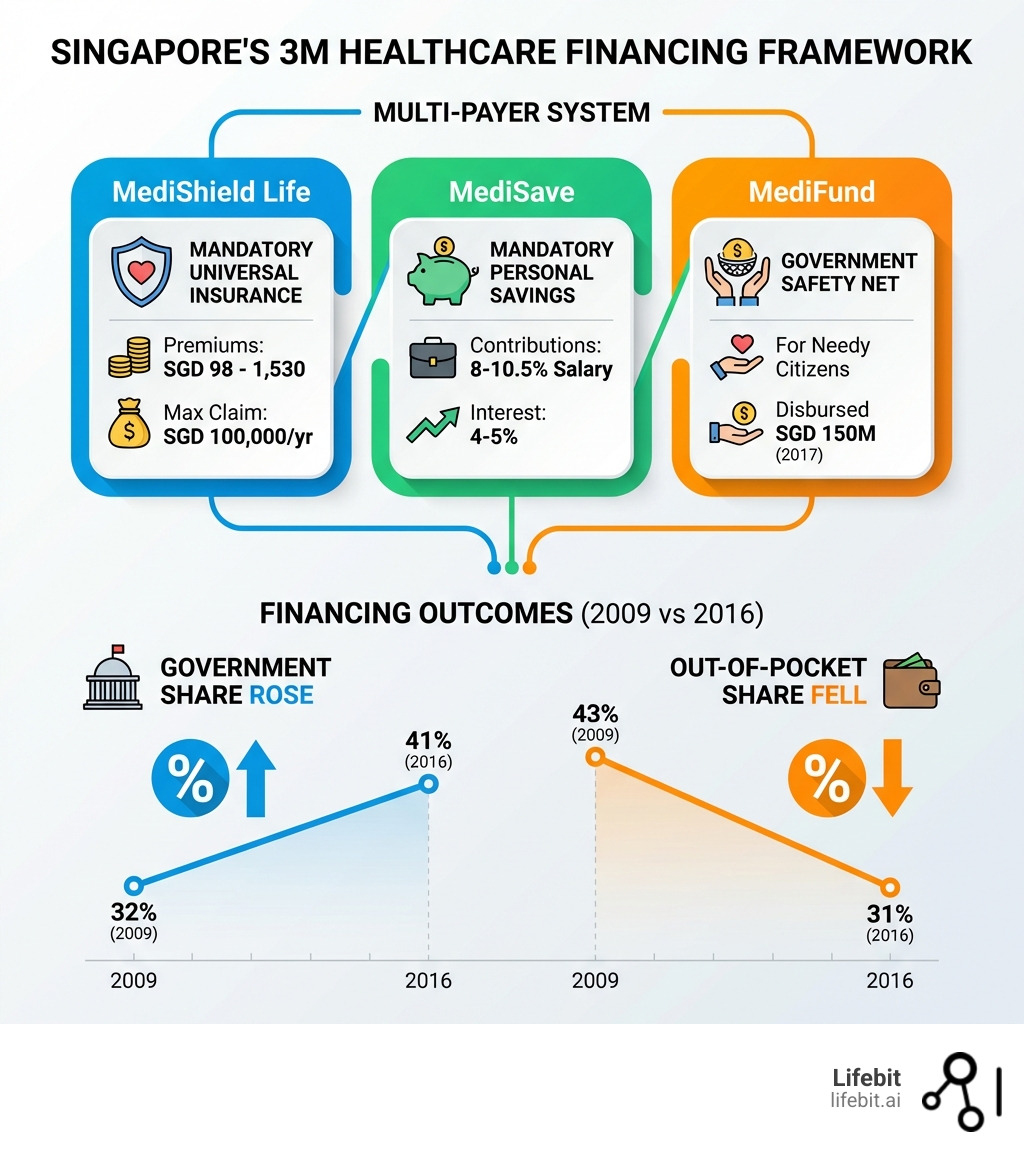
Singapore runs a universal healthcare system built on three pillars — MediShield Life (mandatory insurance), MediSave (personal savings accounts), and MediFund (a government safety net for those who cannot afford care). This “3M” framework balances individual responsibility with strong public funding, keeping out-of-pocket costs low while maintaining financial discipline across the system. Under the “Smart Nation” initiative, the Singapore government has prioritized the digitization of health records, ensuring that data flows seamlessly from primary care clinics to tertiary hospitals. This digital transformation is guided by the Ministry of Health’s (MOH) “Three Beyonds” strategy: Beyond Healthcare to Health, Beyond Hospital to Community, and Beyond Quality to Value.
The country is also a regional leader in precision medicine, home to major initiatives like SG100K, PRECISE, and the HELIOS study — all generating rich, multi-ethnic genomic and clinical datasets that are increasingly valuable to global life sciences research. These initiatives are not just academic; they are integrated into the national health strategy to ensure that genomic insights lead to better clinical outcomes for the population.
Yet significant challenges remain. An aging population, rising obesity rates, and growing mental health pressures are straining a system that already spends more on healthcare per capita than any of its ASEAN neighbors. The “Health District @ Queenstown” is one such pilot project where data is being used to test urban design and community interventions to promote healthy aging, showing how Singapore uses its data to innovate at the intersection of health and urban planning.
I’m Maria Chatzou Dunford, CEO and Co-founder of Lifebit, and my work in federated biomedical data platforms has given me a front-row seat to how Singapore healthcare data is being unlocked for research at scale — securely and compliantly. In the sections below, I’ll break down everything you need to know, from population trends and disease burden to digital infrastructure and future challenges.
Key Singapore healthcare data vocabulary:
Singapore Healthcare Data: Why 1 in 3 Residents Face Chronic Disease Risks

When we look at Singapore healthcare data, the most prominent trend is the incredible longevity of its residents. Singapore currently boasts some of the highest life expectancy figures globally. As of 2021, a newborn in Singapore can expect to live a long life, but the real metric researchers watch is “Healthy Life Expectancy” (HALE).
HALE represents the number of years a person lives in “full health,” accounting for years lost to disease or injury. While Singaporeans are living longer, the gap between total life expectancy and HALE highlights the years spent managing chronic conditions. You can Download data on Singapore life expectancy trends to see how these figures have shifted from 2000 to 2021. The data reveals that while life expectancy has increased by several years over the last two decades, HALE has not kept pace, suggesting a growing period of morbidity at the end of life.
Beyond longevity, the data shows a highly efficient system for maternal and child health. Neonatal and under-five mortality rates are among the lowest in the world, supported by nearly 100% immunization coverage and births attended by skilled personnel. For those interested in the granular details of how this information is captured, check out our Singapore clinical data complete guide.
Leading Causes of Death in Singapore Healthcare Data
Despite its high-income status, Singapore is not immune to the global shift toward non-communicable diseases (NCDs). The leading causes of death in 2021 were dominated by:
- Cancer: A primary driver of mortality for both sexes, with lung, colorectal, and breast cancers being the most prevalent.
- Cardiovascular Disease: Accounting for nearly 30% of all deaths, driven by high rates of hypertension and sedentary lifestyles.
- Pneumonia: Particularly impactful among the elderly population, often as a complication of other underlying chronic conditions.
The probability of dying from NCDs between the ages of 30 and 70 remains a key indicator for the Ministry of Health (MOH). You can Download data on top causes of death by sex to understand the nuances between male and female mortality profiles in the region.
Chronic Disease Prevalence and the “War on Diabetes”
The National Population Health Survey (NPHS) 2024 report released a wake-up call for the nation. While some areas showed improvement, the prevalence of chronic “lifestyle” diseases remains high:
- Hypertension and Hyperlipidaemia: Approximately 1 in 3 residents suffer from high blood pressure or high cholesterol. The data shows a direct correlation with high sodium intake, which remains nearly double the WHO recommended limit in the average Singaporean diet.
- Diabetes: Prevalence remains stable but high. The “War on Diabetes,” launched in 2016, has focused on early detection and lifestyle intervention. Data-driven policies like the “Nutri-Grade” labeling system for beverages are direct interventions aimed at reducing sugar consumption.
- Obesity: This is a major concern. The NPHS 2024 reported a significant increase in obesity prevalence (BMI ≥30.0 kg/m²), particularly among younger adults.
- Mental Health: The 2024 survey highlights that 15% of residents reported poor mental health, with the highest prevalence among those aged 18-29. This has led to a national strategy to integrate mental health services into primary care and community settings.
Interestingly, the data shows that while residents are more willing to go for health screenings now than during the COVID-19 pandemic, the “silent” nature of these conditions means many remain undiagnosed until they reach an acute stage. The “National Steps Challenge,” a gamified health initiative, has successfully used data to encourage physical activity, with over a million participants tracking their daily movement.
How Singapore’s 3M Framework Cuts Out-of-Pocket Healthcare Costs to 31%
Singapore’s healthcare delivery is a unique hybrid of public and private sectors. Primary care is the front line, with over 2,200 private General Practitioner (GP) clinics and 20 (soon to be 32) public polyclinics. While polyclinics only make up a small fraction of the total clinics, they handle about 20% of primary care attendances, specifically focusing on chronic disease management and subsidized care for lower-income groups.
The “3M” financing framework ensures that no Singaporean is denied care due to an inability to pay:
- MediShield Life: A mandatory, universal basic health insurance that covers large hospital bills and expensive outpatient treatments like dialysis. It is designed to protect citizens from catastrophic medical expenses.
- MediSave: A compulsory savings account where 8% to 10.5% of a worker’s salary is set aside for personal or family medical expenses. This encourages individual responsibility for health costs.
- MediFund: The ultimate safety net. It is a government-endowed fund that steps in when MediShield Life and MediSave are exhausted, ensuring that the most vulnerable are covered.
This structure is supported by a robust workforce. As of 2022, the density of doctors stood at approximately 2.4 per 1,000 people. To dive deeper into the technical side of how this infrastructure generates research-ready information, see our page on Singapore biomedical data.
Healthier SG: The Shift to Preventive Care
In 2023, Singapore launched “Healthier SG,” a fundamental shift from reactive to preventive care. This national initiative encourages residents to enroll with a single family physician who manages their long-term health through a personalized Health Plan. This strategy is data-driven at its core, utilizing the National Electronic Health Record (NEHR) to track health outcomes across the population. By incentivizing preventive screenings and vaccinations, the government aims to reduce the long-term burden on acute hospitals. For researchers, this shift creates a wealth of longitudinal primary care data that provides a more holistic view of patient health than hospital-only records.
Managing Costs and Affordability with Singapore Healthcare Data
In 2021, Singapore’s current health expenditure was 5.57% of its GDP. While this is lower than many Western nations, it is projected to rise to 5.9% or even 9% by 2030 as the population ages. To keep costs manageable, the government uses means-testing. This ensures that subsidies are tiered based on income. For example:
- C-class wards in public hospitals can receive up to an 80% subsidy.
- CHAS (Community Health Assist Scheme) provides subsidies for lower-to-middle-income citizens to visit private GPs and dentists, effectively integrating private providers into the public safety net.
- Pioneer and Merdeka Generation packages offer additional subsidies and MediSave top-ups for older residents who built the nation, acknowledging their contribution while managing their higher healthcare needs.
- Primary Care Networks (PCNs): These are groups of private GPs who share resources like nurse educators and care coordinators to manage chronic disease patients more effectively, using shared data to track patient progress.
How Singapore’s TRUST Platform Fixes Data Privacy for Genomic Research
Singapore is betting big on the future of medicine. The National Precision Medicine (NPM) strategy is a multi-phase roadmap aimed at transforming healthcare through genomics. This strategy is divided into three phases: Phase I established the baseline for 10,000 genomes; Phase II (SG100K) is currently sequencing 100,000 genomes; and Phase III will focus on clinical implementation at scale.
Key initiatives include:
- SG100K: A massive effort to sequence the genomes of 100,000 Singaporeans across major ethnic groups (Chinese, Malay, and Indian) to understand Asia-specific disease markers. This is one of the most significant genomic projects in the region.
- PRECISE: The central entity coordinating this strategy, ensuring that genomic data is translated into clinical action and that the infrastructure for precision medicine is robust.
- HELIOS Study: Led by NTU’s Lee Kong Chian School of Medicine, this study tracks 50,000 men and women to identify how lifestyle, environment, and genetics interact to cause chronic disease in an Asian context.
Digital health is the backbone of these innovations. The National Electronic Health Record (NEHR) system aims for “One Patient, One Health Record,” allowing seamless data flow between different care providers. For citizens, the HealthHub portal provides a direct window into their own records, appointments, and lab results. You can learn more about the role of technology in our article on AI healthcare Singapore.
The TRUST Platform: Secure Data Exchange for Research
One of the most significant developments for researchers is the TRUST (Trusted Research and Real-world-data Utilisation and Sharing Tech) platform. TRUST acts as a national data exchange that allows for the secure use of Singapore healthcare data without compromising patient privacy. It is designed to solve the “data silo” problem while maintaining the highest standards of security.
The platform operates on a “SAFE” framework, a globally recognized standard for data governance:
- Safe Purpose: All requests are vetted by a Data Access Committee to ensure the research has a clear public interest and ethical approval.
- Safe People: Only authorized researchers with verified credentials and training in data privacy can enter the environment.
- Safe Settings: Data is hosted in a secure, government-standard, air-gapped environment where data cannot be downloaded or leaked.
- Safe Data: Information is de-identified using advanced techniques like k-anonymity and differential privacy to prevent re-identification of individuals.
- Safe Output: Only aggregate insights and statistical summaries, not raw data, can be exported from the platform after a final review.
This enables the analysis of rich multi-omic datasets and real-world data (RWD) in a way that was previously impossible, fostering a new era of collaborative life sciences research. It allows for the integration of clinical records, genomic data, and even socio-economic data to provide a 360-degree view of health.
The Silver Tsunami: How Singapore Manages a 33% Elderly Population Shift
Singapore is heading toward what experts call “hyper-aging.” By 2030, one in four Singaporeans will be over the age of 65. This demographic shift will place unprecedented pressure on the healthcare system, requiring a complete rethink of how care is delivered and financed.
| Demographic Metric | 2023 (Actual) | 2050 (Projected) |
|---|---|---|
| Total Population | 5.79 Million | ~6.3 Million |
| % Population Over 65 | 10.7% | ~33% |
| Old-Age Dependency Ratio | ~19.0 | ~50.0 |
This “silver tsunami” means a higher incidence of age-related conditions like dementia, frailty, and multi-morbidity. In response, the government has launched the Action Plan for Successful Ageing, a whole-of-nation blueprint. Key components include:
- CareShield Life: A mandatory long-term care insurance scheme that provides monthly payouts for life in the event of severe disability.
- ElderFund: A discretionary assistance scheme for lower-income citizens with severe disabilities who are not covered by other insurance.
- Age Well SG: A program focused on community support, active aging centers, and senior-friendly urban planning.
- Community Care Apartments: A new housing-cum-care model that integrates senior-friendly housing with on-site care services, allowing seniors to live independently for longer.
The “Old-Age Dependency Ratio” data shows that by 2050, there will be only two working-age adults for every senior citizen, down from about five today. This has profound implications for the healthcare workforce, leading to a heavy investment in assistive technology and telehealth to allow seniors to age in place.
Mental health is another growing concern within this demographic. While there is a greater willingness to seek help, the system must adapt to provide more community-based support and early intervention. The “Silver Zone” program in urban planning also uses data to identify areas with high senior populations and implements traffic calming measures and senior-friendly infrastructure to improve safety and mobility.
Singapore Healthcare Data: 6 Critical Questions Every Researcher Must Answer
What is the difference between life expectancy and healthy life expectancy (HALE)?
Life expectancy is the total number of years a newborn is expected to live based on current mortality rates. Healthy Life Expectancy (HALE) is a more nuanced metric; it subtracts the years spent in poor health due to disease or disability. For researchers, HALE is often the more important number because it reflects the actual quality of life and the true burden on the healthcare system. In Singapore, the gap between the two is widening, indicating a need for better chronic disease management.
How does Singapore achieve universal health coverage?
Singapore achieves universal coverage through a “shared responsibility” model. The government provides heavy subsidies (up to 80%) for public care, while the 3M system (MediShield Life, MediSave, and MediFund) ensures that individuals have the means to pay their share. It is a multipayer framework that combines mandatory insurance with personal savings and a state-funded safety net, ensuring financial sustainability.
What are the primary sources for Singapore healthcare data?
The primary sources include:
- Ministry of Health (MOH): For official statistics, policy reports, and expenditure data.
- SingStat: The Department of Statistics for broad demographic and health trends.
- NPHS: The National Population Health Survey for annual updates on lifestyle and chronic disease.
- TRUST Platform: For researchers seeking secure access to anonymized clinical and genomic data.
What legal framework governs health data in Singapore?
The Human Biomedical Research Act (HBRA) and the Personal Data Protection Act (PDPA) provide the legal guardrails. The HBRA specifically regulates the use of human biological materials and health data in research, ensuring ethical conduct and donor protection, while the PDPA governs the collection and use of personal data.
Can international researchers access Singapore’s healthcare data?
Yes, but access is strictly controlled. International researchers can collaborate with local institutions and access data through the TRUST platform, provided their projects meet the “Safe Purpose” criteria and they adhere to the platform’s security protocols.
What is the role of AI in Singapore’s healthcare strategy?
Singapore’s National AI Strategy identifies healthcare as a key sector. Projects like SELENA+, an AI system for detecting diabetic eye disease, are already being deployed. AI is essential for processing the vast amounts of data generated by the NEHR and the National Precision Medicine strategy to improve diagnostic accuracy and risk stratification.
Start Using Singapore Healthcare Data to Accelerate Your Next Breakthrough
The landscape of Singapore healthcare data is a testament to what is possible when a nation combines rigorous data collection with forward-thinking policy. From its world-class life expectancy to its pioneering work in precision medicine through SG100K and the TRUST platform, Singapore serves as a global blueprint for data-driven health. The nation is moving toward a “One Health” approach, where the boundaries between clinical, social, and environmental data are blurring to create a more holistic view of population health.
As the nation faces the challenges of an aging population and rising chronic disease, the focus is shifting toward community care, digital transformation, and personalized medicine. The goal is to create a “Digital Twin” of the population’s health, allowing policymakers to simulate the impact of different interventions before they are implemented. For global researchers and biopharma companies, the multi-ethnic datasets emerging from Singapore offer an unparalleled opportunity to develop treatments that are effective for Asian populations, who have historically been underrepresented in clinical trials.
At Lifebit, we are proud to support this journey. Our next-generation federated AI platform enables secure, compliant access to these vital datasets, ensuring that the next breakthrough in human health can happen faster and more securely than ever before. By bridging the gap between data and insights, we are helping to accelerate the development of the next generation of therapies that will benefit not just Singaporeans, but people across the globe.

