Building Better Health with an EHR Software Development Company

Why the Right EHR Software Development Company Can Transform Patient Care
An ehr software development company helps healthcare organizations design, build, and deploy electronic health record systems tailored to their exact clinical workflows, compliance requirements, and data needs.
Here’s what to look for when evaluating EHR development partners:
| Factor | What to Look For |
|---|---|
| Compliance expertise | HIPAA, GDPR, ONC certification, HL7/FHIR |
| Development approach | Custom vs. off-the-shelf vs. open-source |
| Interoperability | FHIR R4, HL7 v2, API-based integrations |
| Security standards | End-to-end encryption, MFA, role-based access |
| Deployment options | Cloud-native, on-premise, or hybrid |
| Timeline & cost | MVP in 3–6 months; full systems from $50k–$500k+ |
| Post-launch support | Maintenance, updates, clinician training |
Healthcare is in the middle of a digital transformation. With 96% of US non-federal acute care hospitals now using certified EHR systems, the question is no longer whether to digitize — it’s how well your system actually works. The global EHR market is projected to reach over $47 billion by 2030, driven by the shift toward value-based care and the increasing need for real-time data access. However, the mere presence of a digital system does not guarantee efficiency. Many first-generation systems were designed primarily for billing and administrative purposes, leaving clinical utility as an afterthought.
The reality? Many healthcare organizations are stuck with rigid, off-the-shelf platforms that don’t fit their workflows. Clinicians spend hours on manual data entry, a phenomenon often referred to as “pajama time,” where doctors spend their evenings catching up on documentation. Patient data sits in silos, inaccessible to the specialists who need it most. Care coordination breaks down when systems cannot communicate. And compliance gaps create serious legal and financial risk.
Custom EHR development addresses all of this directly — but only when built by a team that understands both the technology and the clinical environment it serves. A specialized ehr software development company acts as a bridge between complex engineering and the high-stakes world of patient care. They don’t just write code; they design ecosystems that support clinical decision-making and improve patient safety.
I’m Dr. Maria Chatzou Dunford, CEO and Co-founder of Lifebit, with over 15 years of experience in computational biology, federated data platforms, and health-tech — including deep work with the kind of biomedical data infrastructure that powers modern EHR software development company decisions at scale. This guide draws on that experience to help you cut through the noise and build something them that actually works.
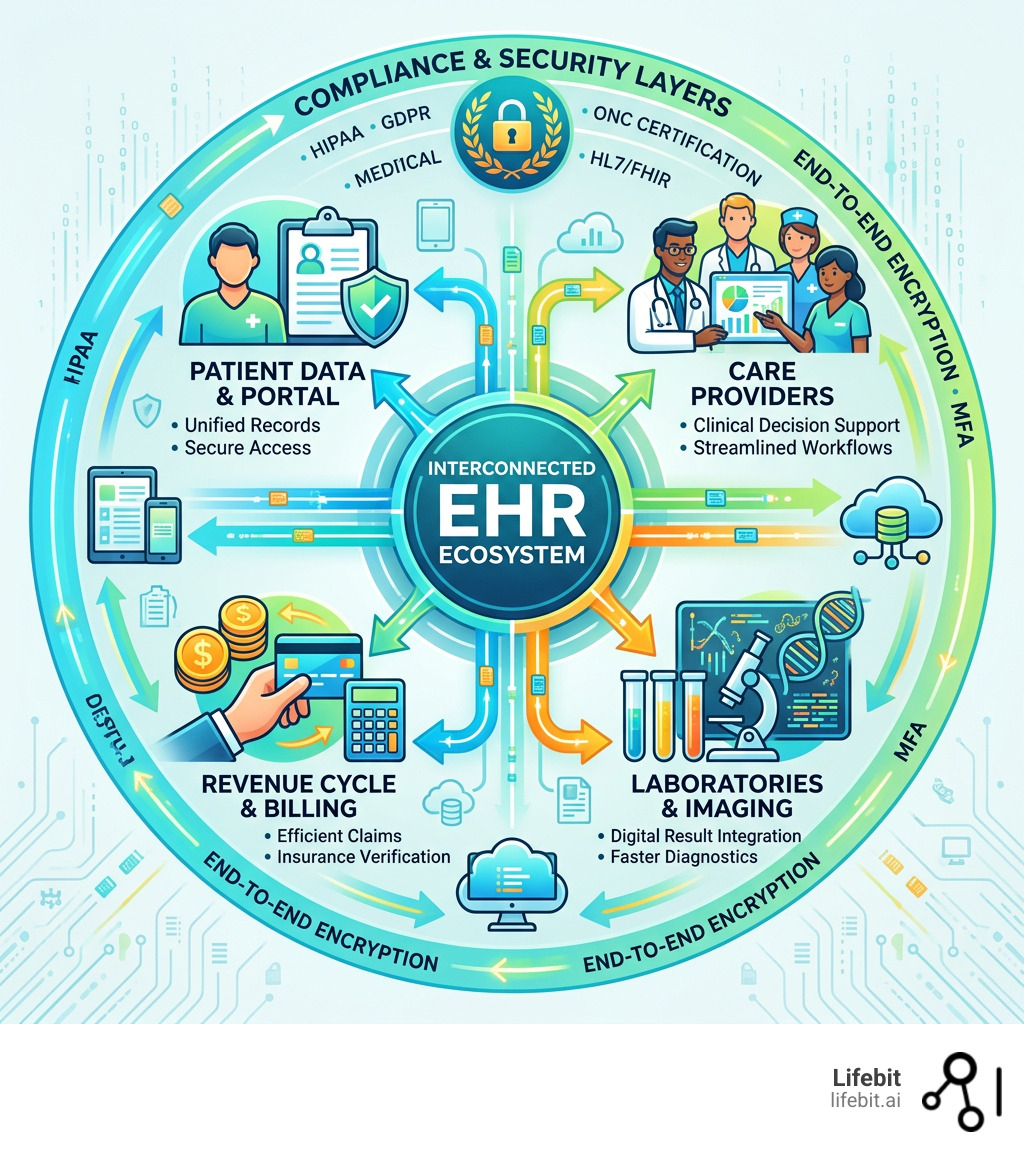
Ehr software development company definitions:
- best electronic medical record software
- electronic medical records companies
- emr systems for small practices
EHR vs. EMR: Understanding the Digital Backbone of Modern Medicine
Before diving into development, it is vital to distinguish between the two primary types of digital records. While people often use the terms interchangeably, they serve very different purposes in a clinical setting. Understanding this distinction is the first step in defining the scope of your project with an ehr software development company.
An Electronic Medical Record (EMR) is essentially a digital version of a patient’s paper chart within a single practice. It is used by clinicians for diagnosis and treatment, focusing on internal efficiency and record-keeping. Think of it as a “digital bedside chart” that stays within the four walls of one clinic. EMRs are excellent for tracking data over time, identifying which patients are due for preventive checkups, and monitoring parameters like blood pressure or vaccinations. You can explore more about these localized tools in our guide to Electronic Medical Record Systems.
In contrast, an Electronic Health Record (EHR) is designed to go beyond the individual practice. It is built to share information with other healthcare providers—such as laboratories, specialists, and pharmacies—so they contain information from all clinicians involved in a patient’s care. EHRs support interoperability, allowing for seamless care coordination across the entire healthcare ecosystem. This means that if a patient is rushed to an emergency room in a different state, the ER physician can instantly access their allergy list, current medications, and recent lab results. For a deeper look at these broader systems, check out our resource on EHRs.
| Feature | EMR (Electronic Medical Record) | EHR (Electronic Health Record) |
|---|---|---|
| Scope | Single practice/office | Multiple providers/organizations |
| Data Sharing | Limited; stays within the clinic | Broad; moves with the patient |
| Patient Access | Usually limited | Often includes a patient portal |
| Standardization | Proprietary formats common | Uses HL7, FHIR, and DICOM |
| Longitudinal View | Snapshot of care at one location | Comprehensive history over time |
The transition from EMR to EHR represents a shift from “data storage” to “data exchange.” In the modern era, the US government has incentivized this shift through the HITECH Act and the “Meaningful Use” program, which requires providers to use certified EHR technology to improve patient outcomes. When you engage an ehr software development company, you are typically looking to build an EHR that can participate in this broader health information exchange (HIE).
Why Partner with a Custom EHR Software Development Company?
With 96% of US hospitals having adopted certified EHR systems, the market is saturated with “one-size-fits-all” products. However, many of these legacy systems are famous for causing clinician burnout. They often feature rigid user interfaces that require dozens of clicks just to order a simple lab test. A study published in the Journal of the American Medical Informatics Association found that physicians spend nearly two hours on EHR tasks for every one hour of direct patient care. This “usability gap” is a primary driver for organizations seeking custom solutions.
By partnering with a specialized ehr software development company, you can move away from these “cookie-cutter” solutions. Custom development allows us to build software that mirrors your actual clinical workflows rather than forcing your staff to change how they work to fit the software. For example, an oncology clinic has vastly different documentation needs than a pediatric practice. A custom system can prioritize the specific data points, templates, and alerts relevant to that specialty. This results in higher clinician adoption rates and, ultimately, better patient outcomes. If you are curious about who the major players are, we’ve reviewed the Best Electronic Medical Records Companies currently in the space.
Overcoming the Limitations of Off-the-Shelf EHR Software Development Company Solutions
Off-the-shelf software often comes with “hidden” burdens. High licensing fees, expensive per-user costs, and “vendor lock-in” can drain a healthcare budget quickly. Furthermore, these systems are notoriously difficult to integrate with newer technologies like wearable health monitors or advanced genomic sequencing tools. When a vendor controls the source code, you are at the mercy of their development roadmap. If you need a specific feature to comply with a new local regulation, you might wait years for an update.
Modern healthcare demands the ability to move data freely. Many older systems act as “data silos,” making it nearly impossible to extract meaningful insights for research or population health. We specialize in Harmonizing Disparate Electronic Health Records to ensure that your data isn’t just sitting in a warehouse, but actively working for you. By moving from Legacy EHR Warehouses to FHIR, we enable real-time data exchange that legacy systems simply cannot match. A custom ehr software development company ensures that your data architecture is built on open standards, giving you full ownership and flexibility over your clinical information.
Core Features and Advanced Tech Stacks for Scalable Platforms
A modern EHR is much more than a digital filing cabinet. To be truly effective, it must incorporate features that enhance both the provider and patient experience. The goal is to create a “single source of truth” that is accessible, secure, and intelligent.

Essential Core Features:
- Patient Portals: Allowing patients to view results, schedule appointments, and message providers. This empowers patients to take an active role in their care and reduces the administrative burden on front-desk staff.
- E-Prescribing: Directly sending prescriptions to pharmacies, reducing errors caused by illegible handwriting and improving the speed of medication fulfillment.
- Clinical Decision Support (CDS): Providing real-time alerts for drug-drug interactions, allergy warnings, or preventive care reminders based on the patient’s specific history.
- Billing & Claims: Seamlessly connecting clinical documentation to the revenue cycle. This ensures that every procedure performed is accurately captured and billed, reducing claim denials. You can read more about how this works in our article on EHR Claims Integration.
Advanced Features:
- AI-Powered Analytics: Using machine learning to predict patient risks, such as the likelihood of readmission or the early onset of chronic conditions. AI can also automate clinical documentation by extracting key data from unstructured notes.
- Telehealth Integration: Native video conferencing and remote monitoring capabilities that allow for virtual visits within the same interface as the patient’s record.
- Voice Recognition: Allowing clinicians to dictate notes directly into the system using Natural Language Processing (NLP), saving hours of manual typing and improving the detail of clinical notes.
Building Future-Proof Systems with a Specialized EHR Software Development Company
To build a platform that lasts, we recommend a modern, cloud-native tech stack. This ensures the system can scale as your organization grows, whether you are adding ten users or ten thousand. Common technologies used by a top-tier ehr software development company include:
- Backend: Node.js, Python, or Go for high-performance data processing. Python is particularly popular for EHRs that incorporate AI and machine learning modules.
- Frontend: React or Angular for responsive, intuitive user interfaces that work across desktops, tablets, and smartphones.
- Cloud Infrastructure: AWS, Google Cloud, or Azure for secure, scalable hosting. These providers offer specialized “Healthcare Blueprints” that simplify HIPAA compliance at the infrastructure level.
- Interoperability Standards: Adherence to HL7 FHIR (Fast Healthcare Interoperability Resources) is non-negotiable. FHIR uses modern web technologies (RESTful APIs) to make it easier for different systems to exchange specific pieces of data rather than entire documents.
These technical choices are the foundation of successful Electronic Health Records Programs, ensuring that the system remains fast, secure, and compatible with future medical devices and apps. A microservices architecture is often preferred, as it allows developers to update specific parts of the system (like the billing module) without taking the entire EHR offline.
Navigating Compliance, Security, and the Development Lifecycle
In healthcare, security isn’t just a feature—it’s the law. Any ehr software development company worth its salt must prioritize a “security-by-design” approach. This means that security is considered at every stage of the development lifecycle, from the first whiteboard session to the final deployment.
Critical Security Measures:
- HIPAA & GDPR Compliance: Ensuring all Patient Health Information (PHI) is handled according to strict legal standards. In the US, HIPAA requires administrative, physical, and technical safeguards. In Europe, GDPR adds layers of data portability and the “right to be forgotten.”
- End-to-End Encryption: Protecting data both at rest (stored on servers) and while it is being transmitted (moving between the EHR and a lab). AES-256 is the industry standard for encryption.
- Multi-Factor Authentication (MFA): Adding an extra layer of protection to prevent unauthorized access. Even if a clinician’s password is stolen, MFA prevents a breach.
- Role-Based Access Control (RBAC): Ensuring that a receptionist only sees scheduling data while a doctor sees full clinical histories. This follows the “principle of least privilege.”
Building a HIPAA-Compliant EMR requires rigorous audits and a deep understanding of the ONC (Office of the National Coordinator for Health IT) certification process. The 21st Century Cures Act has further emphasized the need for “Information Blocking” prevention, requiring EHRs to provide easy data access to patients and authorized third parties.
The Step-by-Step EHR Software Development Company Process
How do we actually build these complex systems? It follows a structured lifecycle designed to minimize risk and maximize utility:
- Discovery & Requirements Gathering: We start by analyzing your current workflows. We interview clinicians, nurses, and administrative staff to identify exactly where the current system is failing. This phase defines the “User Stories” that guide development.
- Prototyping & UI/UX Design: Creating wireframes and interactive prototypes. This allows clinicians to “test drive” the interface and provide feedback on the layout before any backend code is written. This is where we solve the “too many clicks” problem.
- Agile Development: Building the system in “sprints” (usually 2-week cycles). This allows for regular feedback and adjustments. You see the system grow incrementally rather than waiting months for a “big reveal.”
- Testing & Quality Assurance (QA): Rigorous stress testing, penetration testing, and security audits. We simulate high-traffic scenarios to ensure the platform remains stable during peak hospital hours.
- Deployment & Clinician Training: Rolling out the system in phases. We often start with a “pilot group” to catch any minor issues before a full-scale launch. Comprehensive training is provided to ensure every staff member is comfortable with the new tools.
- Maintenance & Continuous Improvement: Ongoing updates to keep up with new regulations, security threats, and medical advancements. A custom EHR is a living product that evolves with your practice.
Estimating Investment: Costs, Timelines, and Deployment Options
Developing a custom EHR is a significant investment, but one that pays off through increased efficiency, reduced long-term licensing costs, and improved patient safety. When evaluating the cost, it is important to consider the Total Cost of Ownership (TCO) over five to ten years, rather than just the initial development price tag.
Budget Expectations:
- Small/MVP Systems: $50,000 to $150,000. Ideal for specialized clinics, private practices, or health-tech startups looking to prove a concept. These systems focus on core documentation and billing.
- Enterprise Platforms: $200,000 to $500,000+. Required for large hospital networks, multi-specialty groups, or regional health authorities. These projects involve complex integrations with legacy lab systems, imaging (PACS), and pharmacy networks.
Timeframes:
- MVP Development: 3 to 6 months. This gets a functional system into the hands of users quickly to begin gathering real-world data.
- Full Enterprise Rollout: 1 to 3 years. This includes the time needed for data migration from legacy systems, which is often the most time-consuming part of the process.
The choice between cloud-native and on-premise deployment also impacts cost. Cloud solutions (SaaS) are typically more cost-effective as they eliminate the need for expensive on-site servers and IT maintenance staff. They also offer better scalability and easier remote access for telehealth. On-premise solutions offer maximum control for organizations with very specific infrastructure needs or those operating in regions with unreliable internet connectivity. As we look toward the future, digital health technology for an aging population will require these systems to be more mobile and accessible than ever before, favoring cloud-first architectures.
Measuring the ROI of Custom Development
How do you justify the cost of a custom ehr software development company? The ROI comes from several areas:
- Reduced Administrative Overhead: Automating tasks like appointment reminders and insurance verification can reduce the need for administrative staff.
- Improved Billing Accuracy: Custom systems can include “hard stops” that prevent a clinician from closing a chart until all billable elements are documented, significantly increasing revenue capture.
- Lower Malpractice Risk: Better data visibility and clinical decision support reduce the likelihood of medical errors, which can lead to lower insurance premiums.
- Clinician Retention: By reducing the frustration associated with poor software, organizations can improve job satisfaction and reduce the high costs associated with physician turnover.
Frequently Asked Questions about EHR Development
How long does it typically take to develop a custom EHR?
Development timelines generally range from 6 months for a Minimum Viable Product (MVP) to 3 years for a full-scale enterprise platform. The timeline is heavily influenced by the number of third-party integrations (e.g., connecting to specific lab vendors or state immunization registries) and the complexity of the data migration from your existing system.
What is the average cost of custom EHR software?
While basic systems may start around $50,000, comprehensive enterprise solutions with advanced AI, multi-system integrations, and full regulatory compliance can exceed $500,000. It is important to budget for ongoing maintenance, which typically costs 15-20% of the initial development cost annually.
Why is interoperability so important in modern EHRs?
Interoperability ensures that different healthcare systems can exchange and interpret data seamlessly. This is critical for care coordination, reducing medical errors (such as duplicate testing), and meeting ONC certification standards. Without interoperability, a patient’s medical history remains fragmented, which can lead to dangerous gaps in care.
Can a custom EHR integrate with my existing billing software?
Yes. A professional ehr software development company can build custom APIs or use standard protocols like HL7 to ensure that clinical data flows seamlessly into your existing revenue cycle management (RCM) tools. This prevents the need for double-entry and ensures that billing is triggered as soon as care is delivered.
Is cloud-based EHR storage secure enough for HIPAA?
Absolutely. Modern cloud providers like AWS and Microsoft Azure offer HIPAA-compliant storage solutions with advanced encryption and physical security that often exceed what a private clinic could maintain on-site. The key is ensuring the software layer is correctly configured by your development partner.
Conclusion
Building a custom EHR is about more than just moving from paper to digital; it’s about creating a tool that empowers clinicians and improves patient lives. The transition from legacy, siloed systems to modern, interoperable platforms is the most significant shift in modern medicine. Whether you are looking to modernize a legacy system that is slowing your team down or build a new platform from the ground up to support a specialized clinical need, choosing the right ehr software development company is the most important decision you will make.
At Lifebit, we understand that the future of healthcare lies in data. Our federated AI platform is designed to provide secure, real-time access to global biomedical and multi-omic data, powering the next generation of large-scale research and clinical excellence. We believe that the data generated within an EHR should not just be a record of the past, but a roadmap for the future of personalized medicine. By prioritizing security, interoperability, and user experience, we help organizations turn complex data into actionable insights.
Learn more about how Lifebit’s platform can power your healthcare data strategy and help you build a more connected, compliant, and efficient future. The right technology doesn’t just store data; it saves lives.

