The Definitive Guide to Leading AI Chronic Disease Platforms

Why Chronic Disease Registers Need AI Now
What are the leading platforms for creating and managing a chronic disease register using AI? The leading platforms are those that move beyond simple data collection to offer automated data abstraction, predictive analytics, and federated learning capabilities for secure, multi-institutional research. They turn static patient lists into intelligent systems for proactive care.
Chronic diseases affect nearly 40% of Americans—approximately 129 million people. Five of the top 10 U.S. causes of death are linked to these preventable conditions. Yet, traditional disease registers often rely on fragmented spreadsheets and manual data entry, creating reactive care models that can’t keep pace.
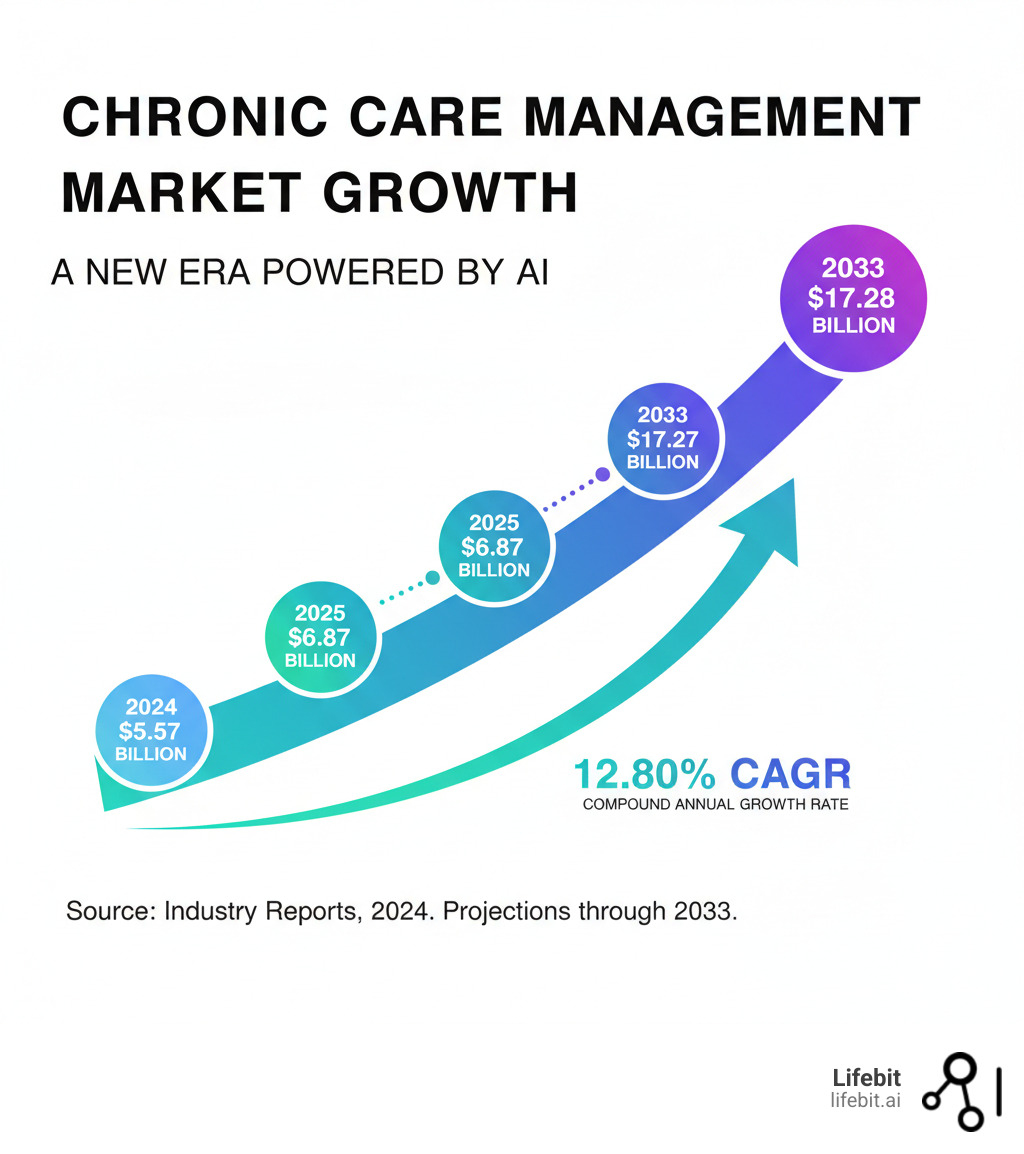
The chronic care management market, valued at $5.57 billion in 2024 and projected to hit $17.28 billion by 2033, signals an urgent need to move beyond these legacy approaches.
AI is rewriting the rules. Modern platforms automate data abstraction from unstructured clinical notes, predict patient deterioration, and enable care teams to manage more patients with the same resources. Instead of waiting for ER visits, AI-powered registers identify risk in real time to trigger proactive interventions.
I’m Maria Chatzou Dunford, CEO and Co-founder of Lifebit. With over 15 years in computational biology and precision medicine, I’ve seen how platforms that securely analyze distributed health data can transform clinical and research outcomes.
What are the leading platforms for creating and managing a chronic disease register using AI? terms to remember:
From Static Lists to Smart Systems: The Evolution of Chronic Disease Registers
A chronic disease register is a structured database for population health management, tracking patients with long-term conditions like diabetes, heart disease, or chronic obstructive pulmonary disease (COPD). It helps care teams monitor clinical trends, coordinate interventions, and measure population-level outcomes. For public health agencies, these registers are vital for disease surveillance, resource allocation, and policy-making, as highlighted by the CDC’s focus on using EHRs to build smarter registries.
For decades, however, these registers were anything but smart. Traditional methods relied on manual data entry into disconnected spreadsheets and rudimentary databases. This approach was plagued with fundamental flaws. Data was often siloed, with a patient’s information fragmented across primary care EHRs, specialist notes, hospital discharge summaries, and pharmacy records. Assembling a complete, longitudinal picture of a patient’s health was a Herculean task, often impossible. The data itself was latent; by the time it was manually entered, it was already outdated, reflecting a past crisis rather than present risk. This created a reactive care model where providers managed diseases only after an acute event, like a hospitalization for heart failure, instead of preventing it. The administrative burden was immense, with clinical staff spending hours on data entry instead of patient care, leading to burnout and a high potential for human error. High-risk patients were easily missed amidst the noise of stale, incomplete data.
AI changes everything.
Modern platforms use automation and Natural Language Processing (NLP) to fundamentally rewire this process. AI algorithms can pull and interpret data directly from unstructured sources like clinical notes, pathology reports, and discharge summaries in near real-time. NLP can understand clinical context, differentiating between a patient’s diagnosis of diabetes and a note about their family history of the disease. This eliminates the bottleneck of manual entry and captures rich, nuanced information—such as symptom severity or social determinants of health (SDoH)—that is often buried in free-text fields.
Data integration becomes a seamless reality. AI-powered systems act as a central nervous system, harmonizing information from disparate sources—EHRs, pharmacy databases, lab systems, remote monitoring devices, and even patient-reported outcome surveys—into a single, unified patient view. But the real game-changer is predictive analytics. Machine learning models analyze these comprehensive datasets to identify subtle patterns that precede adverse events. By analyzing thousands of variables, these models can flag patients at high risk of hospitalization, disease progression, or medication non-adherence, shifting the entire paradigm from reactive firefighting to proactive, preventative care.
The contrast is stark. Imagine a care manager for a diabetic population. The old way involved manually cross-referencing a spreadsheet of patient names with lab reports to find those with high HbA1c levels, a process that could take days. The new way involves an AI-powered dashboard that automatically flags patients with rising HbA1c, recent ER visits for hyperglycemia, and documented transportation issues, prioritizing them for immediate outreach. This evolution is about building registers that actively help keep populations healthier, not just passively document their decline.
What are the leading platforms for creating and managing a chronic disease register using AI?
The next generation of disease registers is built on intelligence, not just information. From automated data collection to predictive insights, these platforms are already changing chronic disease management. They are distinguished by a core set of powerful capabilities that transform raw data into actionable clinical intelligence.
Key Features of AI-Powered Registry Platforms
Modern platforms make data useful. Here’s what separates them from legacy systems:
- Natural Language Processing (NLP): This is the engine that unlocks the 80% of health data trapped in unstructured text. Advanced NLP models go beyond simple keyword matching to understand clinical syntax, negation, and context. For example, an NLP algorithm can accurately extract a patient’s ejection fraction from a cardiologist’s note, identify mentions of medication side effects from a discharge summary, and differentiate between a patient’s active diagnosis of cancer and a note about their mother’s history of the disease. This allows for the creation of a much richer, more accurate patient profile automatically.
- Automated Data Abstraction: This feature uses AI to parse both structured data (like lab values and billing codes) and unstructured text with superhuman speed and high accuracy. It frees up highly trained clinical staff, such as nurses and data abstractors, from the tedious and error-prone task of manual chart review. Instead of a clinical team spending hundreds of hours per year building and maintaining a registry, AI can populate and update it continuously, ensuring the data is always current and ready for analysis.
- Real-World Evidence (RWE) Generation: AI transforms a static registry into a dynamic research engine. By continuously analyzing anonymized data from routine clinical practice, these platforms generate RWE to answer critical questions about treatment effectiveness, disease progression, and long-term outcomes in diverse patient populations. Our Lifebit platform’s R.E.A.L. layer, for example, is designed to facilitate this continuous insight generation, helping researchers understand how a new therapy performs outside the controlled environment of a clinical trial.
- Predictive Modeling & Risk Stratification: This is where AI shifts care from reactive to proactive. Machine learning models are trained on historical data to identify patients at high risk of future adverse events. For instance, a heart failure readmission model might analyze variables like recent medication changes, fluctuating weight from remote monitoring, lab results (like BNP levels), and previous hospitalizations to assign a risk score. This allows care teams to focus their limited resources on the patients who need them most, intervening before a crisis occurs.
- Interoperability with EHRs: To be effective, an AI platform must integrate seamlessly into clinical workflows. This is achieved through modern APIs and adherence to interoperability standards like FHIR (Fast Healthcare Interoperability Resources). This ensures a bidirectional flow of data, where the AI platform can pull the latest information from the EHR and, in some cases, push insights and alerts back into the clinician’s native workspace, minimizing disruption and maximizing adoption.
- Data Security Standards: Trust is the bedrock of any healthcare technology. Leading platforms are built with privacy-by-design principles, adhering strictly to regulations like HIPAA in the U.S. and GDPR in Europe. They validate their security posture through independent certifications like SOC 2 Type 2 and ISO 27001, which provide assurance that robust controls are in place for security, availability, processing integrity, and confidentiality.
- Federated Learning: This groundbreaking approach enables large-scale research and model training without centralizing sensitive data. Instead of moving patient data to a central server, the AI model (the code) is sent to the data’s source institution (e.g., a hospital). The model trains on the local data behind the institution’s firewall, and only the aggregated, non-identifiable insights or model updates are shared. Our platform uses this federated architecture to protect patient privacy while enabling powerful, multi-institutional research that would otherwise be impossible.
Types of AI Platforms Changing Chronic Disease Management
Different platforms serve different needs across the healthcare ecosystem:
- Population Health Management (PHM) Platforms: These provide health systems with a high-level, panoramic view of their patient populations. For example, a PHM platform can identify all patients with COPD across a network, flag those who are overdue for a spirometry test, and stratify them by risk of a future exacerbation, enabling targeted public health campaigns and resource allocation.
- EHR-Integrated AI Modules: These tools embed predictive analytics and clinical decision support directly into the electronic health record. A primary care physician might receive an alert within the EHR that their patient’s recent lab results and vital signs, when analyzed by an AI model, indicate a high risk of developing sepsis, prompting immediate action at the point of care.
- Data Analytics & RWE Platforms: These platforms are specialized for deep analysis, turning vast amounts of real-world data into actionable insights for life sciences research, regulatory submissions, and personalized medicine. Lifebit, for instance, specializes in enabling secure analysis of complex biomedical and multi-omic data within distributed environments, helping researchers discover novel biomarkers or validate drug targets.
- AI-Supported Care Coordination Tools: These platforms focus on the operational side of chronic care. They can automate patient outreach for follow-up appointments, send personalized reminders for medication refills, and streamline communication between different members of a patient’s care team (e.g., primary care, specialists, and social workers).
- Patient Engagement Platforms with AI: These tools empower patients to take an active role in their own care. An AI-powered mobile app might provide a diabetic patient with personalized dietary suggestions based on their blood glucose readings, use a chatbot to answer common questions about their condition, and offer encouragement to help them meet their activity goals.
How can AI-powered registers facilitate personalized treatment plans and interventions?
AI makes personalized care scalable by moving beyond one-size-fits-all protocols:
- Automating Care Plan Generation: AI algorithms can synthesize a patient’s complete profile—including medical history, comorbidities, genomic data, lab trends, and even social determinants of health—to suggest a highly personalized care plan. This plan can be tailored to the individual’s specific risk factors and goals.
- Driving Patient Adherence: Non-adherence to medication and lifestyle changes is a major challenge in chronic disease. AI can deliver timely, personalized “nudges” and reminders via text message or app notifications, using behavioral science principles to encourage positive actions and help patients stay on track.
- Customizing Patient Communication: AI can tailor educational materials and messages based on a patient’s documented health literacy level, preferred language, and cultural background. This ensures that information is not just delivered but is also understood and accessible, improving patient engagement.
- Suggesting Proactive Interventions: By continuously monitoring streams of data from wearables, remote monitors, and the EHR, AI can detect subtle changes that signal a patient’s condition is worsening. It can then alert the care team to intervene—perhaps with a telehealth visit or a medication adjustment—long before the patient would have ended up in the emergency room.
- Identifying and Closing Care Gaps: These platforms automatically scan patient records to find missed appointments, overdue cancer screenings, or needed vaccinations. The system can then automate the outreach process to schedule these essential preventative care services, ensuring no patient falls through the cracks.

A unified patient view, pulling data from all sources, is the foundation that makes true personalization possible at scale.
The Tangible Benefits & Inherent Challenges of AI Adoption
AI offers transformative potential for chronic disease management, but its adoption is not a simple plug-and-play solution. It requires a strategic approach to overcome implementation challenges and ensure equitable, effective deployment.
The Upside: Why AI-Driven Registers are a Game-Changer
The shift to AI-powered systems delivers fundamental, measurable improvements across clinical, operational, and financial domains:
- Improved Patient Outcomes: By enabling earlier detection and more personalized interventions, AI directly contributes to better health. One study found that chronic care management services, often powered by such platforms, led to 32-99 fewer hospital stays and 23-76 fewer ER visits per 1,000 patients. For specific conditions, the impact is even clearer: AI algorithms that predict sepsis can reduce mortality rates, while predictive models for diabetic ketoacidosis can trigger alerts that lead to life-saving early treatment.
- Operational Efficiency and Reduced Clinician Burnout: AI automates the most tedious and time-consuming aspects of data management. Instead of spending hours each week manually abstracting data from charts, a care coordinator can review an AI-prioritized list of high-risk patients in minutes. This automation frees clinicians to practice at the top of their license, focusing on complex decision-making, patient counseling, and direct care, which in turn helps mitigate the growing crisis of clinician burnout.
- Proactive vs. Reactive Care: This is the most profound shift enabled by AI. Traditional healthcare is inherently reactive. AI-powered registers enable a crucial pivot to proactive prevention. By identifying at-risk individuals before they decompensate, health systems can intervene earlier, improve patients’ quality of life, and significantly lower the high systemic costs associated with emergency care and hospitalizations.
- Scalability of Care Management: With AI handling the heavy lifting of data analysis and patient prioritization, care teams can manage significantly larger patient populations without a proportional increase in staff. Some organizations report being able to manage 3x more patients with the same care management team, expanding access to high-quality chronic care services.
- Financial Sustainability: AI-driven programs are not just a cost center; they generate substantial revenue and savings. They enable practices to capitalize on reimbursement programs like Medicare’s CCM codes. Furthermore, in value-based care models (e.g., Accountable Care Organizations), AI is essential for meeting the quality metrics and cost-reduction targets that trigger shared savings and bonuses, making the platform a financially sound investment.
The Problems: Challenges and Limitations to Overcome
Implementing AI is a complex undertaking with significant hurdles that must be addressed strategically:
- Data Quality and Completeness: The “garbage in, garbage out” principle applies forcefully to AI. Models trained on incomplete, inaccurate, or inconsistent data will produce flawed and unreliable insights. For example, if an EHR contains sporadic data entry for a key lab value, a predictive model relying on that value will fail. This necessitates a strong data governance framework and robust data validation and cleaning pipelines before AI can be deployed effectively.
- Algorithmic Bias: This is one of the most critical ethical challenges. If an AI model is trained on historical data that reflects existing health disparities, it can perpetuate and even amplify those biases. For example, a widely used algorithm for predicting kidney disease risk systematically under-predicted risk in Black patients because it incorporated a flawed, race-based clinical variable. Mitigating bias requires conscious effort, including fairness audits, using representative training data, and designing models that are transparent and explainable.
- High Implementation Costs: The initial investment in AI technology can be substantial. Costs include not only software licensing fees but also potential infrastructure upgrades (cloud computing resources), data integration expenses, and, crucially, the cost of training staff to use the new tools and workflows. While many organizations find that the ROI is achieved within the first year through increased revenue and efficiency, the upfront capital can be a barrier for smaller or less-resourced practices.
- Regulatory Compliance: The legal and regulatory landscape for health data and AI is complex and constantly evolving. Platforms must ensure strict compliance with data privacy laws like HIPAA and GDPR. As AI becomes more autonomous, new regulatory questions around algorithmic transparency, accountability (who is responsible if an AI makes a mistake?), and FDA oversight for clinical decision support tools are emerging, requiring constant vigilance.
- Essential Human Oversight: AI is a powerful tool for augmentation, not replacement. It cannot replicate a clinician’s judgment, empathy, or ability to understand a patient’s unique life context. The most effective models operate with a “human-in-the-loop” design, where the AI provides recommendations and prioritizations, but the clinician makes the final decision. They must be trained to critically interpret AI-generated insights, understand their limitations, and override them when their clinical judgment dictates.
- Interoperability with Legacy Systems: Many health systems still rely on older IT infrastructure and EHRs that were not designed for modern data exchange. Integrating a new AI platform with these legacy systems can be technically complex and costly, often requiring custom-built connectors and middleware. A lack of standardized APIs can create significant friction and delay the realization of AI’s benefits.
The question isn’t whether AI will revolutionize chronic disease management—it already is. The real question is how organizations can strategically navigate these challenges to realize its full, equitable potential.
Securing the Future: Data Privacy, Governance, and What’s Next
The long-term success and ethical implementation of AI in healthcare hinge on a foundation of robust security, strong governance, and a commitment to continued innovation.
How do these platforms ensure data privacy and security when managing sensitive patient information?
Leading platforms employ a multi-layered, defense-in-depth strategy to protect sensitive health information:
- Regulatory Compliance: Adherence to legal frameworks is the baseline, not the goal. This includes the Health Insurance Portability and Accountability Act (HIPAA) in the U.S., which mandates specific administrative, physical, and technical safeguards for Protected Health Information (PHI), and the General Data Protection Regulation (GDPR) in Europe, which enforces principles like data minimization and purpose limitation. At Lifebit, we build our platform with these privacy-by-design principles embedded from the start.
- Certifications and Audits: To provide objective proof of their security posture, top-tier platforms undergo rigorous independent audits. Certifications like SOC 2 Type 2 verify that a vendor has effective, long-term controls for security, availability, and confidentiality. ISO 27001 is another key certification that demonstrates a systematic approach to managing information security.
- Data Encryption: All sensitive data is rendered unreadable to unauthorized parties through encryption. This applies to data at rest (when stored in databases or on servers) and data in transit (as it moves between systems over a network). This ensures that even in the event of a physical breach or interception, the underlying data remains protected.
- De-identification and Anonymization: To enable analysis while protecting privacy, personally identifiable information (PII) is removed or masked. It’s important to distinguish between anonymization (where all identifiers are permanently stripped) and pseudonymization. The latter replaces direct identifiers with a reversible token, allowing researchers to link a patient’s data over time for longitudinal studies without revealing their real-world identity.
- Federated Trusted Research Environments (TREs): This is a paradigm shift in data security for research. Instead of pooling sensitive data into a central location (which creates a high-value target for attack), our Lifebit platform uses TREs to bring the analysis to the data. The process works like this: an approved analytical model is sent into the secure, firewalled environment of each data custodian (e.g., a hospital). The model runs on the local data, and only the aggregated, non-identifiable results are returned. The raw patient data never leaves its secure, original location.
- Secure Data Enclaves: These are highly restricted, isolated computing environments where sensitive data can be processed. Access is strictly controlled through multi-factor authentication, and every action taken within the enclave is logged and audited. This ensures that only authorized personnel and vetted analytical processes can interact with the data.
The Role of AI in Identifying At-Risk Populations and Predicting Disease Progression
AI’s superpower is its ability to detect complex, non-linear patterns in massive datasets to anticipate patient needs long before they become critical:
- Predictive Risk Scoring: AI models analyze hundreds of variables—including clinical history, lab results, medication records, and social determinants of health—to calculate a patient’s risk for a specific adverse event. This score allows care teams to triage and prioritize their efforts effectively. For example, a model predicting COPD exacerbations might incorporate not just clinical data but also real-time inputs like local air quality data, pollen counts, and medication adherence data from a smart inhaler.
- Early Disease Detection: Algorithms can monitor high-frequency data streams (e.g., from wearables or remote patient monitoring devices) for subtle deviations from a patient’s baseline. These small changes, often imperceptible to a human reviewer looking at periodic data, can be early warning signs of disease progression or an impending acute event, enabling preemptive intervention.
- Identifying Care Gaps at Scale: AI can systematically scan an entire patient population to pinpoint subgroups that are missing recommended care. This could include identifying all women over 40 with a family history of breast cancer who are overdue for a mammogram or finding diabetic patients who have not had a retinal eye exam in the past year, then automating outreach to close these gaps.
- Analyzing Social Determinants of Health (SDoH): Health outcomes are profoundly influenced by non-clinical factors. AI allows for the integration and analysis of SDoH data—such as a patient’s zip code (as a proxy for socioeconomic status), access to transportation, or food insecurity data. A model might learn that patients living in a “food desert” are at higher risk for poor glycemic control, prompting a referral to a social worker or community food program.
Future Trends in AI for Chronic Disease Management
The AI revolution in healthcare is just beginning. The next wave of innovation will bring even more sophisticated capabilities:
- Generative AI for Patient Education and Engagement: Imagine an AI-powered assistant that can create personalized, easy-to-understand educational materials for a patient in real time. A patient newly diagnosed with heart failure could ask a chatbot, “What does my new medication do and what side effects should I watch for?” The AI would generate a response in their preferred language and at their specific health literacy level, drawing from their EHR and approved medical knowledge bases.
- AI-Powered Clinical Trial Matching: Chronic disease registries are a goldmine for clinical research. AI will be able to scan the rich, longitudinal data in these registries to identify eligible patients for clinical trials with unprecedented speed and precision. This will dramatically accelerate recruitment for studies on new therapies, especially for rare diseases.
- Hyper-Personalization of Care Plans: Future systems will move beyond static care plans to create dynamic, adaptive recommendations. By integrating genomics, real-time wearable data (sleep, activity), and even environmental factors, an AI could create a care plan for a person with asthma that adjusts medication recommendations based on the day’s pollen count and air quality forecast.
- Federated Learning for Global Research: As federated learning technology matures, it will enable secure research collaboration on a global scale. This will be particularly transformative for rare diseases, where patient data is sparse and scattered across many countries. Researchers will be able to train robust AI models on these distributed datasets without ever compromising patient privacy or violating data sovereignty laws.
- Real-Time Pharmacovigilance: Instead of relying on slow, voluntary reporting systems, AI will continuously scan registry data for signals of adverse drug reactions. If a new medication is associated with a statistically significant increase in a particular side effect across thousands of patients, the system could raise an alert for regulatory review months or even years earlier than traditional methods.
Frequently Asked Questions about AI in Chronic Disease Management
How much does an AI chronic care management platform cost?
Pricing for AI platforms varies based on features, patient volume, and service level. However, many practices achieve a positive ROI within the first year. Medicare’s Chronic Care Management (CCM) program allows practices to earn approximately $332-$372 per enrolled patient annually. For a practice with 200 patients, this can translate to nearly $150,000 in annual revenue.
When you factor in operational savings from automation and benefits from value-based care agreements, these platforms often become profitable investments that also improve patient outcomes.
How does AI integrate with existing Electronic Health Records (EHRs)?
Seamless integration is crucial. Modern AI platforms are built to connect with EHRs using standard tools:
- APIs (Application Programming Interfaces) act as digital handshakes, allowing different software systems to exchange data automatically.
- Interoperability standards like FHIR (Fast Healthcare Interoperability Resources) provide a common language for healthcare data, ensuring information is not lost in translation.
- Direct integrations with major EHR vendors enable real-time data synchronization, so AI-driven insights are based on the most current patient information available.
At Lifebit, our federated platform is designed to connect to multiple data sources, including EHRs, while keeping data secure and in its original location. This provides clinicians with AI-driven insights directly within their existing workflows.
Is AI intended to replace clinicians in chronic disease management?
No. AI is a tool to augment human intelligence, not replace it. Think of AI as a tireless assistant that handles tedious administrative work, prioritizes high-risk patients, and uncovers patterns in data that might otherwise be missed.
AI automates tasks like data abstraction and report generation, freeing clinicians to focus on complex decision-making and direct patient care. It helps you know which patient needs attention most urgently and enables proactive interventions before a crisis occurs.
However, AI cannot provide empathy, build trust, or make complex judgment calls that require understanding a person’s life context. Human oversight is absolutely central. The algorithm provides the data; the clinician provides the wisdom and care. Our platform at Lifebit is designed to empower researchers and clinicians, making them more effective, not obsolete.
Conclusion: Building a Proactive, Data-Driven Future for Chronic Care
We are at a turning point. The shift from manual, reactive disease registers to intelligent, AI-powered systems is accelerating. These platforms are making proactive, personalized care an everyday reality for millions living with chronic conditions. By predicting complications, triggering timely interventions, and identifying care gaps, AI allows care teams to manage larger populations more effectively while freeing clinicians to focus on what matters most: their patients.
The greatest challenge—and opportunity—is to do this securely. The future lies in federated platforms that can analyze diverse, global data while keeping patient information private and protected. By bringing analysis to the data, we can open up real-world evidence at an unprecedented scale. Lifebit’s federated AI platform enables this next generation of research and care, providing secure access to global biomedical data through our Trusted Research Environment (TRE) and other advanced tools. We empower researchers and clinicians to uncover deeper insights and facilitate personalized treatments within a compliant, collaborative environment.

