Why Every Modern Hospital Needs a Healthcare Integration Engine

Stop Data Silos: How a Healthcare Integration Engine Slashes Costs by 50%
#
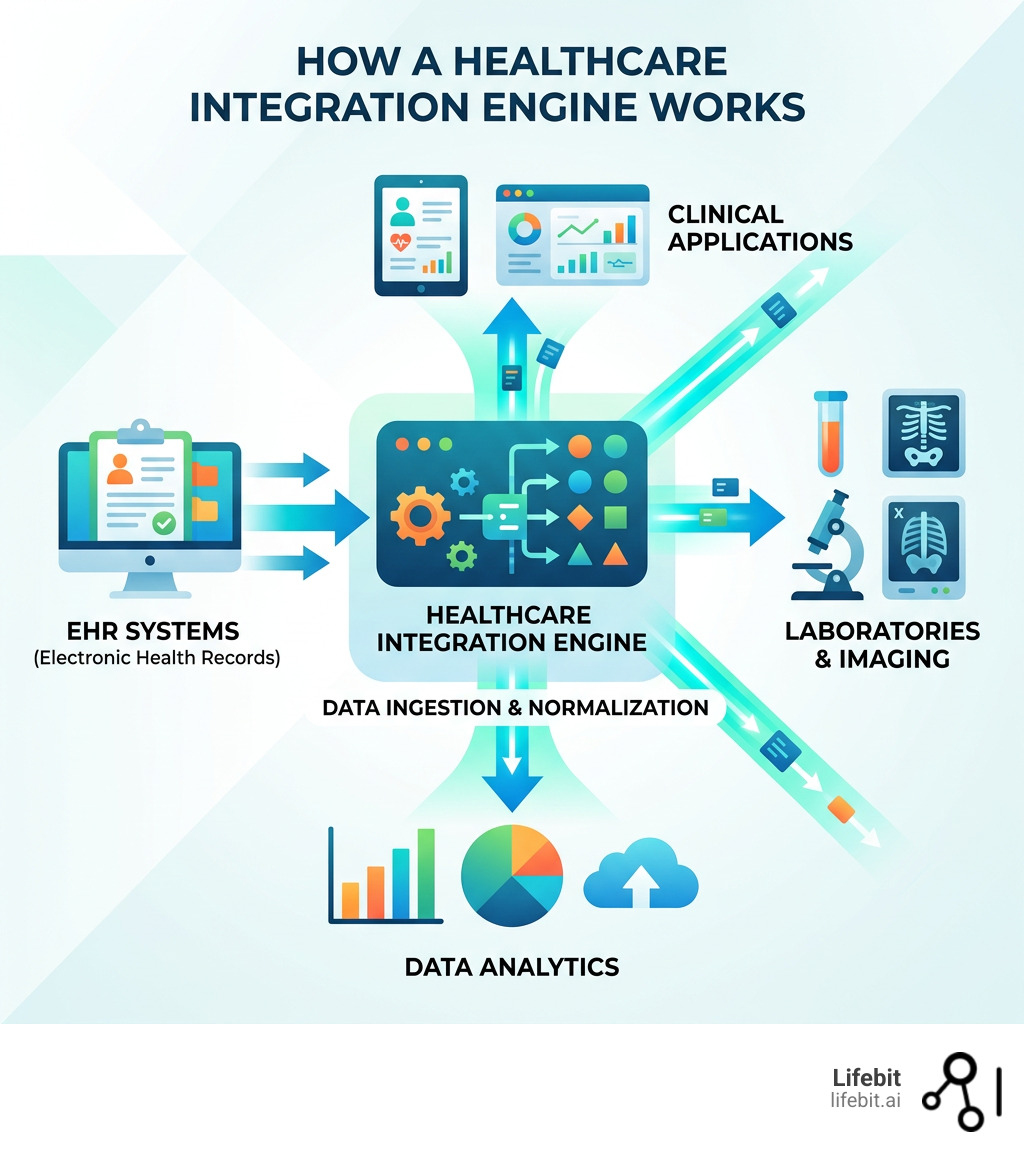
A healthcare integration engine is software that acts as a central hub, connecting siloed systems — EHRs, labs, imaging platforms, billing, and more — so they can share data in real time without manual intervention. In the modern medical landscape, where data is generated at an exponential rate, these engines serve as the vital nervous system of a healthcare enterprise, ensuring that the right information reaches the right clinician at the right time.
Every day, integration engines process millions of critical healthcare messages. When they slow down or fail, the consequences are immediate — delayed lab results, unavailable patient records in the ER, and disrupted clinical workflows. The stakes are not abstract. According to Health Level Seven International, standardized data exchange is the foundation of modern interoperability. Without a robust engine, a hospital is essentially a collection of digital islands, each speaking a different language and unable to coordinate care effectively.
Yet many healthcare organizations still rely on fragmented, point-to-point connections between systems built in different eras, using different standards. This “spaghetti architecture” is not just an IT headache; it is a massive financial drain. Research indicates that inefficient data management and manual reconciliation can consume up to 30% of a hospital’s operational budget. The result is data locked in silos, slow onboarding of new technologies, and IT teams spending more time on maintenance than on innovation. By centralizing these connections, a modern engine can slash integration-related costs by up to 50% through reduced labor, eliminated redundancies, and faster deployment cycles.
I’m Maria Chatzou Dunford, CEO and Co-founder of Lifebit, and over 15 years of work in biomedical data integration — including building federated platforms that connect genomics, EHR, and clinical data across secure environments — has shown me how a poorly integrated data infrastructure creates bottlenecks at every stage of patient care and research. Choosing the right healthcare integration engine is one of the most consequential infrastructure decisions a health organization can make, and this guide breaks down exactly how to do it.
Healthcare integration engine vocabulary:
- health data integration
- Can you list firms that specialize in clinical trial data integration platforms?
- data integrity in health information systems
In the old days of hospital IT, if you wanted the lab system to talk to the billing system, you built a direct “pipe” between them. Then you needed the EHR to talk to the lab, so you built another pipe. Pretty soon, your hospital’s backend looked like a bowl of spaghetti. This is what we call “point-to-point” integration, and it is the primary reason why digital transformation in healthcare often feels like wading through molasses. Each new connection requires custom coding, unique security protocols, and individual monitoring. If one system upgrades, every connected pipe might break, leading to a cascade of failures.
A healthcare integration engine changes the game by acting as a universal translator and traffic controller. Instead of hundreds of messy pipes, every system connects once to the engine. We have seen that implementing a robust engine can reduce development time to nearly half of what was required with legacy interface methods. This centralized communication eliminates the need for manual data entry, which is a notorious source of errors and delays. For example, when a patient is admitted, their demographic data can be automatically pushed from the registration desk to the pharmacy, the lab, and the bedside monitoring system simultaneously.
By breaking down these data silos, hospitals gain massive operational agility. When a new clinical application or a cutting-edge AI diagnostic tool needs to be onboarded, it doesn’t take eighteen months of custom coding. With the right engine, you can bridge legacy systems with modern cloud services in a fraction of the time, ensuring that your IT infrastructure supports, rather than hinders, patient care. This agility is the difference between a hospital that can pivot to meet new health crises and one that is paralyzed by its own technical debt.

How Engines Work: Standards, Protocols, and Data Transformation
Think of a healthcare integration engine as a master linguist. In any given hospital, you have systems speaking different “languages.” Your imaging department uses DICOM; your clinical systems use various versions of HL7 (v2 or v3); your billing department might use X12; and your modern web apps want to use JSON or FHIR bundles. Without a translator, these systems are effectively deaf to one another.
The engine works through several core functions that ensure seamless data flow:
- Protocol Support: It handles the “handshakes” between systems using various communication methods such as TCP/IP, HTTP, FTP, or SOAP. It manages the low-level connectivity, ensuring that a message sent from a legacy Unix-based system can be received by a modern Windows or Linux-based cloud application.
- Data Transformation: This is the magic. The engine takes an HL7 message from an old EHR—which might be a string of pipe-delimited text—and transforms it into a FHIR resource (JSON) that a modern mobile app can understand. This involves parsing the source data, applying logic rules, and reformatting it into the destination’s required structure.
- Message Queuing and Persistence: If the receiving system is down for maintenance or experiencing a traffic spike, the engine doesn’t just drop the data. It holds the message in a secure, persistent queue. Once the destination system is back online, the engine delivers the messages in the correct order, ensuring no vital patient data is lost during downtime.
- Data Mapping and Normalization: It aligns fields between different systems—ensuring that “DOB” in one database correctly maps to “DateofBirth” in another. More importantly, it can normalize values. If one system uses “M/F” for gender and another uses “1/2,” the engine translates these values on the fly so the data remains consistent across the enterprise.
- Routing Logic: Engines use sophisticated rules to decide where data should go. For instance, a lab result indicating a critical value might be routed not just to the EHR, but also as an urgent SMS alert to the attending physician’s mobile device and a notification to the charge nurse’s dashboard.
By adhering to healthcare data integration standards, these engines ensure that data isn’t just moved, but is actually usable. For instance, advanced engines use automated extraction agents to pull data even when standard APIs aren’t available, converting unstructured notes or PDFs into AI-ready datasets. This process of “semantic interoperability” means that the receiving system doesn’t just get the data; it understands the context and meaning behind it, which is essential for clinical decision support systems.
Evaluating Healthcare Integration Engine Solutions
When you are comparing solutions, you aren’t just looking for a software license; you are looking for a performance partner. Modern engines process millions of vital messages daily, so “good enough” isn’t an option. A failure in the integration layer can lead to “data ghosting,” where a clinician believes they have the full patient record, but critical updates are missing because of a silent failure in the background.
For high-transaction volumes, enterprise-grade engines are often cited as the “circulatory system” of the organization because of their high-availability features and ability to scale to the most demanding tasks. A powerful engine for hospitals focused on the supply chain should be capable of handling full item loads of over 50,000 items in mere minutes—exceeding the standard data requirements of most EMRs by three times. You must also consider the “developer experience.” An engine that requires proprietary coding languages for every simple map will eventually become a bottleneck. Look for engines that offer “low-code” visual mapping tools alongside robust scripting capabilities for complex transformations.
Choosing the Right Healthcare Integration Engine Deployment Model
The “how” of deployment is just as important as the “what.” The choice between on-premises and cloud-based solutions often comes down to a balance between control, cost, and internal expertise. We generally see three main paths:
| Model | Description | Pros | Cons |
|---|---|---|---|
| On-Premises | Installed on your own hardware within the hospital data center. | Total data control; no reliance on external internet for internal routing. | High maintenance burden; difficult to scale quickly; high upfront CAPEX. |
| Self-Managed Cloud | You host a license on your own cloud infrastructure (AWS, Azure, GCP). | Scalable infrastructure; fits into existing cloud strategy. | Requires in-house cloud expertise; you are still responsible for patching and uptime. |
| Fully Managed (SaaS) | “Interoperability-as-a-Service” where the vendor hosts and manages the engine. | No infrastructure headaches; 24/7 monitoring included; predictable OPEX. | Often limited to specific regions; less control over the underlying server environment. |
Choosing the right model is essential for long-term health data interoperability. For many organizations, a fully managed service is the fastest path to ROI because the vendor handles all the messy coordination, adapter building, and maintenance. This allows the hospital’s IT staff to focus on high-value projects like data analytics and patient engagement rather than server patching.
Future-Proofing with a Modern Healthcare Integration Engine
Healthcare is moving toward a FHIR-first world. Global regulations, such as the CMS Interoperability and Patient Access final rule in the US, now frequently mandate FHIR compliance, making “FHIR bridging”—the ability to turn legacy HL7 data into modern FHIR resources—a non-negotiable feature. If your engine cannot natively handle FHIR resources, it is already obsolete.
A modern healthcare integration engine serves as the foundation for digital transformation. It allows you to use data harmonization techniques to clean and standardize data from disparate sources, making it ready for real-time analytics and AI. This is where the transition from “storing data” to “using data” actually happens. By creating a “clean” data stream, you enable advanced use cases like predictive sepsis modeling or real-time bed management that were previously impossible due to fragmented data.
Why Monitoring Performance is Critical for Patient Safety
If an integration engine is the “brain” of your hospital’s IT, then a “stroke” in that brain can be catastrophic. Imagine a critical lab result—perhaps a life-threatening potassium level—getting stuck in a message queue because of a CPU spike. The doctor never sees the alert, the pharmacy doesn’t prepare the corrective medication, and the patient suffers. In healthcare, latency isn’t just a technical metric; it’s a clinical risk factor.
This is why vendor-neutral monitoring is critical. While many engines have built-in dashboards, they often only show you what is happening inside the engine. Specialized tools like PRTG or Datadog provide a broader view across your entire environment, showing how the engine interacts with the network, the databases, and the end-point applications. Key metrics we recommend tracking include:
- Message Throughput: Are messages moving at the expected speed? You should establish a baseline for “normal” traffic and set alerts for any deviation of more than 20%.
- Queue Depth: Is data backing up? A growing queue is an early warning of a system crash or a downstream application that has stopped accepting data. If a queue reaches a certain threshold, it should trigger an immediate high-priority ticket for the IT team.
- Failed Message Rates: Are specific interfaces dropping data? You need to know if 1% of your HL7 messages are failing due to formatting errors, as those failures represent missing pieces of patient history.
- System Health: Monitoring CPU, memory, and database latency to prevent bottlenecks. Integration engines are often memory-intensive; a leak in a custom script can slowly degrade performance over weeks before causing a total system halt.
- ACK/NACK Ratios: In HL7 communication, an “ACK” is an acknowledgment that a message was received, while a “NACK” is a negative acknowledgment. Monitoring the ratio of NACKs can help identify misconfigured interfaces before they impact clinical care.
Using specialized sensors for HL7 and DICOM ensures that you aren’t just seeing “up or down” status, but actual workflow health. For example, you can monitor the time it takes for a “Stat” order to move from the EHR to the lab system, ensuring that your technical performance aligns with your clinical SLAs (Service Level Agreements).
Use Cases: From EHR Integration to Real-Time Analytics
What does this look like in the real world? The versatility of a healthcare integration engine allows it to solve problems across the entire spectrum of care delivery and research.
- EHR Write-back and Bi-directional Sync: Using modern FHIR APIs, organizations can write analytics data back to dozens of different EHR systems in real time. This means a risk score calculated in an external AI platform—such as a readmission risk score—can appear directly in the clinician’s view within the EHR. This eliminates the need for doctors to log into multiple portals to see AI insights.
- Real-Time Event Detection and Population Health: A value-based care platform can stream clinical documents through an engine to detect care gaps the moment a patient is discharged. For instance, if a diabetic patient is discharged without a follow-up appointment scheduled, the engine can trigger an automated workflow in the care management system to call the patient within 24 hours.
- Unified Research Data and Clinical Trials: Advanced integration points allow research teams to pull data from labs, imaging, and EHR claims integration into a single environment for analysis. This is particularly powerful for clinical trials, where real-world evidence (RWE) needs to be gathered from multiple hospital sites using different IT systems. The engine standardizes this data, making it ready for researchers without months of manual cleaning.
- Telehealth and Remote Patient Monitoring (RPM): As more patients use wearable devices, the integration engine acts as the gateway. It can ingest data from a patient’s home blood pressure cuff, normalize the units, and insert the readings into the EHR’s flowsheets. If a reading is dangerously high, the engine’s routing logic can immediately alert the primary care team.
- Disaster Recovery and Business Continuity: During a system migration or an EHR downtime event, the integration engine can serve as a “read-only” backup. Because it has a record of all recent messages, clinicians can sometimes use the engine’s logs to view the most recent lab results or medications even when the primary EHR is offline.
Frequently Asked Questions about Healthcare Integration Engines
What is the difference between an interface engine and an integration engine?
While the terms are often used interchangeably, an “interface engine” traditionally focused on simple point-to-point message routing (like HL7 v2). It was a “dumb pipe” that moved data from A to B. A modern healthcare integration engine is much broader—it is an orchestration layer. It handles APIs, FHIR, complex data transformation, and often includes logic to manage multi-step workflows between dozens of systems. It doesn’t just move data; it manages the entire lifecycle of the information.
How do integration engines handle FHIR and legacy HL7 data?
They use “translation maps” or “transformers.” The engine receives a legacy HL7 message, parses the data into an internal format, and then maps it into a modern FHIR resource (like a Patient, Observation, or MedicationStatement resource). Some advanced engines offer “FHIR Façades” that allow legacy systems to look and act like modern FHIR servers to external apps without changing a single line of the legacy system’s underlying code. This is the most cost-effective way to meet modern interoperability mandates.
Why is a fully managed integration service better for hospitals?
Hospitals are in the business of saving lives, not managing server clusters or troubleshooting TCP/IP handshakes at 3:00 AM. A fully managed service offloads the burden of 24/7 monitoring, security patching, and vendor coordination to the experts. This ensures higher uptime and better security, as the managed service provider can apply security patches across their entire fleet of engines the moment a vulnerability is discovered. It also solves the “talent gap” problem, as specialized integration engineers are increasingly difficult and expensive to hire and retain.
Can an integration engine help with HIPAA compliance?
Yes, but it is not a magic bullet. A properly configured engine helps by encrypting data in transit (using TLS) and at rest. It also provides a centralized audit log, showing exactly who sent what data and where it went. This is a critical requirement for HIPAA audits. However, the organization must still ensure that access controls and user permissions within the engine are strictly managed to prevent unauthorized data access.
Conclusion
The days of treating hospital data as a series of disconnected islands are over. To provide modern, data-driven care, a healthcare integration engine is no longer a luxury—it is the essential backbone of the enterprise. By moving away from fragile point-to-point connections and embracing a centralized, FHIR-ready hub, healthcare organizations can reduce their IT overhead by 50%, improve clinician satisfaction, and, most importantly, enhance patient safety through better data availability.
As we look toward the future of medicine, the role of integration will only grow. Whether it is incorporating genomic data into routine clinical care or using AI to predict patient deterioration, the success of these innovations depends entirely on the quality of the underlying data plumbing.
At Lifebit, we take this a step further. While an integration engine moves and translates data within your walls, our federated biomedical data platform allows you to securely access and analyze that data alongside global datasets without it ever leaving your secure environment. This “federated” approach solves the final piece of the puzzle: how to use integrated data for large-scale research while maintaining absolute privacy and security. By combining robust integration with federated AI, healthcare organizations can finally unlock the full potential of their data to drive both better patient outcomes and groundbreaking research.

