All About Data Governance Models: Centralized vs. Decentralized

Your Clinical Trials Are 80% Likely to Fail Because of Bad Data Governance—Here’s How to Fix It
When you compare solutions for centralized vs decentralized data governance in clinical research, you find two distinct approaches to managing sensitive patient information:
| Centralized Governance | Decentralized Governance |
|---|---|
| Single authority controls all data policies | Multiple teams manage their own data domains |
| High consistency, easier compliance | Greater agility, faster innovation |
| Risk of bottlenecks and slow delivery | Risk of inconsistent standards |
| Single point of failure | Resilient, distributed architecture |
| Best for: highly regulated, single-site studies | Best for: multi-site trials, diverse datasets |
Clinical research is drowning in data. A typical Phase III trial now generates 3.6 million data points—three times more than 15 years ago. With the market projected to hit $886.5 billion by 2032, traditional data management is failing, causing 80% of trials to face delays. As global data explodes toward 180 zettabytes by 2025, organizations face a critical choice: centralize for control or decentralize for speed?
This isn’t just an IT decision; it’s a strategic one impacting innovation, compliance with GDPR and HIPAA, and the speed at which treatments reach patients. Pure centralization creates bottlenecks, while pure decentralization leads to chaos. The right answer lies in finding a balance.
As Maria Chatzou Dunford, CEO and Co-founder of Lifebit, I’ve helped organizations steer this choice for over 15 years. This guide will help you find the winning strategy for your clinical research.
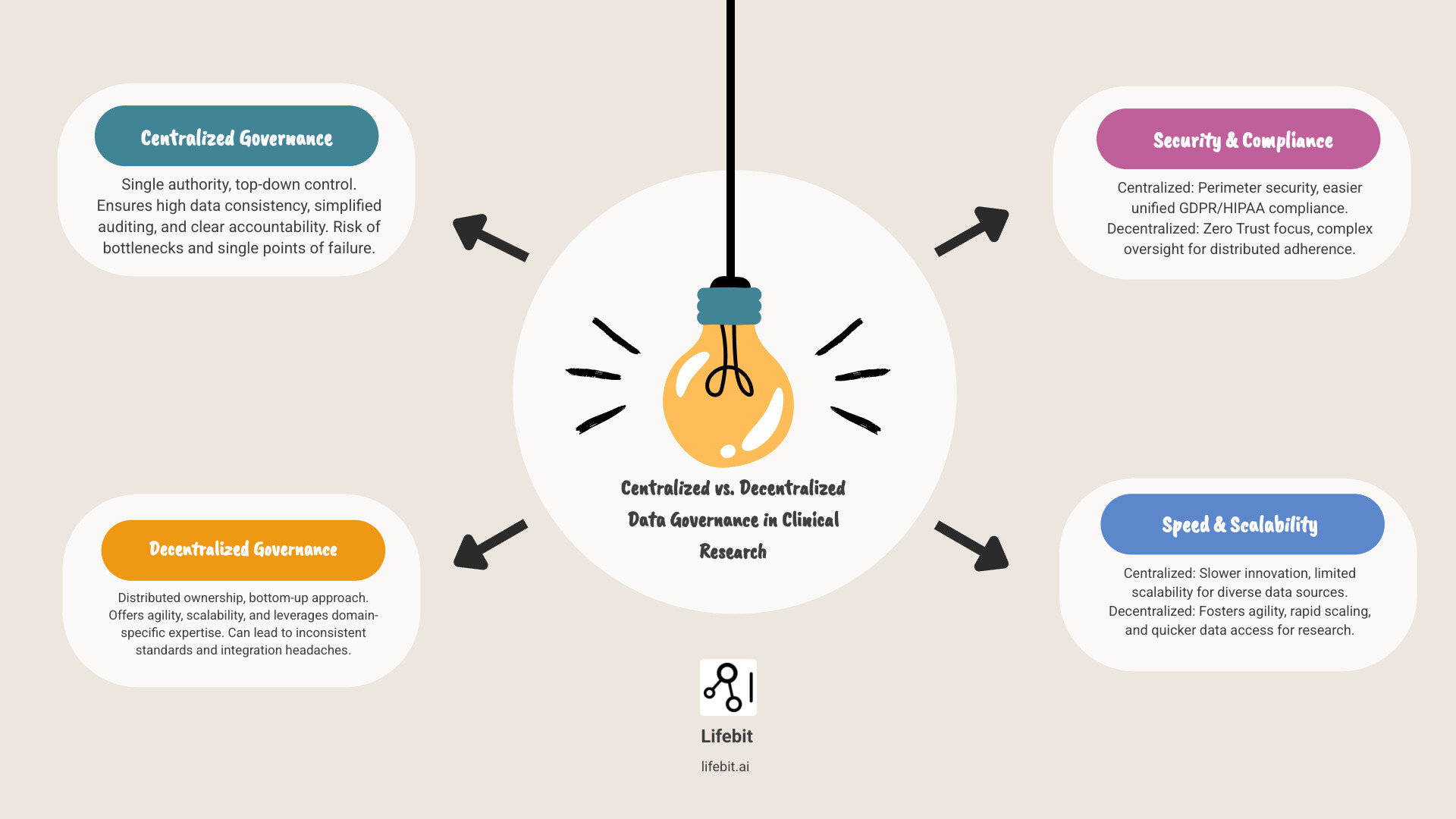
Compare solutions for centralized vs decentralized data governance in clinical research. terms to remember:
Centralized Data Governance Costs You $8 Million Per Day in Trial Delays
Centralized data governance operates like a fortress: one authority controls all data access and movement. For decades, this top-down approach was the standard in clinical research, offering the appeal of complete control. But as data volumes and trial complexity grow, this fortress can become a cage.
Benefits: The Single Source of Truth
When you compare solutions for centralized vs decentralized data governance in clinical research, the centralized model’s main strength is consistency, creating a “single source of truth.”
- Standardization & High Data Quality: A single team enforces rules for data formats and validation, ensuring consistency and reducing errors across all sites.
- Simplified Auditing & Compliance: With all data flowing through one hub, tracking lineage for GDPR or HIPAA audits is straightforward. Policies are applied uniformly, simplifying compliance.
- Clear Accountability: A single team owns data governance, eliminating confusion over responsibility.
Drawbacks: When the Fortress Becomes a Prison
The same walls that protect can also trap you, creating the very problems they aim to solve.
- Research Bottlenecks: Funneling all requests through one team creates delays. Queries that should take hours can stretch into weeks, costing millions and delaying patient access to treatments.
- Data Silos: When formal access is too slow, researchers create workarounds like local copies and shadow databases, leading to the risk of data silos.
- Single Point of Failure: If the central system goes down, everything stops. A server outage can halt multi-site trials and disable safety monitoring, creating a single point of failure.
- Slow Innovation & Limited Context: Rigid, one-size-fits-all rules stifle the adoption of new technologies and fail to account for the nuances of different research domains. This bureaucracy forces researchers to fight the system instead of focusing on science.
While a centralized model offers control, it often comes at the cost of speed and flexibility. It may work for small, simple studies, but it struggles with the scale and complexity of modern clinical research.
How Decentralized Governance Cuts Trial Time by 40%—But Risks Million-Dollar GDPR Fines
A decentralized model is a network of outposts, each with local governance. This bottom-up approach distributes data ownership to teams and collaborators, empowering those closest to the data. Instead of a single authority, you trust domain experts—like the oncology or genomics labs—to manage their own data effectively.
Benefits: Empowering Domain Experts
When you compare solutions for centralized vs decentralized data governance in clinical research, decentralization excels at open uning speed and scale.
- Agility and Speed: Local teams make decisions without central approval, accelerating adjustments to protocols and enabling rapid testing of new analytics.
- Scalability and Resilience: The structure scales organically as new trial sites or data types are added. With no single point of failure, the system is more resilient; an issue at one site doesn’t halt the entire study.
- Domain-Specific Expertise & Innovation: Teams can tailor governance to their specific data needs (e.g., genomics vs. imaging), ensuring policies are practical. This autonomy fosters experimentation and innovation.
Drawbacks: The Wild West of Data
Without coordination, decentralization can lead to chaos.
- Inconsistent Standards: With multiple teams setting their own rules, aggregating data becomes a nightmare. Different sites may use conflicting terminologies (e.g., ICD-10 vs. SNOMED CT), making enterprise-wide analysis difficult.
- Data Silos and Integration Headaches: Instead of breaking down silos, this model can create new ones, leading to worsening data silos at the local level. Integrating these disparate datasets is expensive and time-consuming.
- Security Gaps: Varying security controls across teams can create vulnerabilities. Inconsistent privacy policies have led to multi-million dollar GDPR fines.
- Duplicated Work and Costs: Teams may unknowingly reinvent the wheel, building similar tools or buying redundant software, which wastes time and money.
Decentralization offers speed and scale, but it requires strong guardrails to prevent fragmentation and compliance risks.
Compare Solutions for Centralized vs Decentralized Data Governance in Clinical Research
When we compare solutions for centralized vs decentralized data governance in clinical research, we’re looking at how each approach impacts security, data quality, technology adoption, and cost. The choice affects every aspect of a clinical trial, from compliance protocols to the speed of innovation.
Impact on Security, Privacy, and Compliance
In clinical research, security and compliance are non-negotiable. Centralized models traditionally rely on a strong perimeter defense—a digital fortress—which simplifies security management but creates a high-stakes single point of failure. A breach of the central repository can be catastrophic, exposing all patient data at once. Decentralized environments, by contrast, are better suited to modern Zero Trust security architectures. This ‘never trust, always verify’ principle means that every user, device, and application must be authenticated and authorized before accessing any data, regardless of whether they are inside or outside the organization’s network. This is particularly effective in decentralized models where the network perimeter is ill-defined, creating layered, resilient security as advocated by NIST guidance on secure data sharing.
For global regulations like GDPR and HIPAA, the models present different challenges. A centralized system ensures consistent rule application but concentrates risk; a single breach could lead to fines of up to 4% of global annual revenue under GDPR. In decentralized systems, risk is localized, but ensuring consistent policy application across dozens of sites is a major challenge. For example, the roles of ‘data controller’ and ‘data processor’ under GDPR can become ambiguous in a decentralized setup, increasing legal risks if not clearly defined for each participating site. Managing patient consent is also more complex. While simpler to track in a central database, federated models must handle dynamic consent—where patients update their preferences over time—across multiple systems. This often requires advanced techniques like privacy-preserving record linkage (PPRL) and even exploring blockchain for immutable, auditable consent logs, adding another layer of technological complexity but enabling collaboration as data centralization becomes “increasingly non-viable.”
Effect on Data Quality, Consistency, and Integration
Research utility depends on data quality. Centralized harmonization, where a single team cleans and standardizes all incoming data, makes it easier to enforce standards. This leads to higher consistency and less time spent on data cleaning during analysis. In decentralized settings, data is often heterogeneous, as different sites use local standards, terminologies, and measurement units. This makes enterprise-wide analytics a significant challenge without a robust strategy for interoperability.
This is where Common Data Models (CDMs) like OMOP and CDISC become essential for decentralized and federated research. Implementing a CDM involves a significant upfront effort in data mapping, where local terminologies (e.g., proprietary lab codes) must be translated into the standard vocabulary. This process, known as ETL (Extract, Transform, Load), can be resource-intensive and requires deep domain expertise. However, the payoff is immense: once data is in the CDM format, standardized analytical tools can be run across all sites with minimal modification, drastically accelerating multi-site studies. Even with CDMs, challenges remain, such as assessing EHR data quality, which can vary widely between institutions, and overcoming interoperability problems in multi-site studies.
Furthermore, robust, federated metadata management is crucial in a decentralized system. Without it, researchers at one site may not know what data exists at another, or they may misinterpret its meaning. A federated data catalog becomes essential, acting as a searchable index of all available datasets across the network, complete with lineage, quality scores, and access protocols. This prevents data silos from becoming data swamps.
The Role of Modern Technology
Technology is reshaping clinical research and its governance. The process of digitizing clinical trials is accelerating the shift away from purely centralized models.
- Telemedicine, Wearables, and IoT: These tools generate continuous, real-time data from patients’ everyday lives, offering richer insights than periodic clinic visits. Governing this massive influx of data requires flexible and scalable solutions.
- Cloud-Based Systems: The cloud provides the necessary scalability and flexibility for modern trials, enabling real-time data integration from multiple sources with robust security.
- AI and Machine Learning: AI can rapidly analyze vast datasets to find patterns, but it requires strong governance to ensure ethical use. Federated learning is a key technology, allowing collaborative model training on decentralized data without moving it, thus preserving privacy.
Cost Implications of Each Model
When we compare solutions for centralized vs decentralized data governance in clinical research, cost is a critical factor beyond the initial investment.
| Factor | Centralized Governance | Decentralized Governance |
|---|---|---|
| Upfront Cost | Potentially higher for initial infrastructure & software | Lower initial investment, distributed across teams/nodes |
| Operational Cost | Centralized staff, maintenance, potential for delays to be costly | Distributed personnel, technology costs per node, potential for duplicated efforts |
| Scalability | Can be expensive and slow to scale up | Scales naturally with new nodes, but integration costs can rise |
| Speed | Slower decision-making, potential for bottlenecks | Faster local decisions, quicker innovation |
| Security | High cost for robust perimeter defense, single point of failure risk | Costs for distributed security tools, Zero Trust, potential for varied security postures |
| Compliance Fines | High risk for single, large breach | Risk from inconsistent local policies, but smaller individual impact |
Centralized models have high upfront infrastructure costs, while decentralized models distribute them. Personnel costs are concentrated in centralized teams but spread out in decentralized ones. While some research suggests decentralized management is costlier, the delays from centralized governance bottlenecks can cost up to $8 million per day. Efficient data management is key to reducing clinical trial costs. The long-term ROI depends on balancing these factors: a system that accelerates drug findy and improves patient retention may justify higher operational costs.
The Future is Federated: A Hybrid Approach for Modern Trials
The debate to compare solutions for centralized vs decentralized data governance in clinical research isn’t about choosing a side. The most successful organizations are finding a middle ground that delivers both control and innovation. This is the promise of federated governance: maintaining strong standards while empowering teams to move fast, and analyzing global data while it remains secure in its original location.
What are Hybrid and Federated Governance Models?
Hybrid and federated models blend the strengths of both approaches. Hybrid governance establishes a central body to set core principles (the ‘what’ and ‘why’), while local teams manage daily operations and implementation within those guidelines (the ‘how’). This allows for both strategic oversight and local flexibility.
The technological and organizational paradigm that enables this is the Data Mesh, a new paradigm shift in data ownership that treats data as a product. It is built on four core principles:
- Domain-Oriented Ownership: Instead of a central data team, ownership and responsibility for data are pushed to the business domains that are closest to it—the ‘producers’ of the data. For example, the genomics lab team owns the genomic data, and the clinical operations team owns the trial management data. These teams are responsible for the quality, security, and accessibility of their data assets.
- Data as a Product: Each domain must treat its data as a product it provides to the rest of the organization (the ‘consumers’). This means the data must be discoverable, addressable, trustworthy, self-describing, interoperable, and secure. The domain team is accountable for the user experience of their data products, just like a software team is for a software product.
- Self-Serve Data Platform: To enable domains to manage their data products effectively without being data engineering experts, a central platform team provides a self-service infrastructure. This platform offers tools for data storage, processing, access control, federated learning, and monitoring, allowing domain teams to build and deploy their data products efficiently.
- Federated Computational Governance: This is the linchpin that prevents chaos. A federated governance body, composed of representatives from each domain and the central platform team, defines global standards, policies, and best practices. This includes interoperability standards (like using CDMs), security policies, and privacy rules. Crucially, the platform then automates the enforcement of these rules, ensuring compliance without creating a central bottleneck.
The technological backbone for analysis in this model is federated learning, which trains AI models across these decentralized data products without moving the data. An analysis of centralized and federated models confirms this is critical for collaborative, multi-site modeling.
Why Federated Governance is a Game-Changer
Federated governance solves the major headaches of multi-site, international clinical trials.
- Secure Multi-Site Collaboration: Data stays at the source institution, under local control, respecting data sovereignty laws across Europe, the USA, and Canada. Researchers collaborate by sharing insights, not raw patient data.
- Access to Diverse Global Datasets: It becomes feasible to conduct rare disease studies or pharmacovigilance analyses across continents, as institutions don’t have to give up control of their data.
- Powerful Real-World Evidence (RWE) Generation: Federated models can leverage distributed data from EHRs, claims, and wearables to understand how treatments perform in the real world.
This shift toward empowering decentralized research is supported by analysts like Gartner, whose research on adaptive governance advocates for tailoring governance to the business context. At Lifebit, our platform is built for this federated future, enabling organizations to implement a hybrid approach that provides flexibility, security, and scale without compromise.
How to Choose the Right Data Governance Model for Your Trial
Choosing the right data governance model is a strategic imperative. To compare solutions for centralized vs decentralized data governance in clinical research effectively, you need a clear framework based on your trial’s specific context.
When to Use Each Model
The optimal model depends on the nature and scale of your clinical trials.
- Centralized: Best for small, single-site, or early-phase studies where direct control and simplicity are paramount.
- Decentralized/Hybrid: Ideal for large, multi-national trials (e.g., across the USA, Europe, Canada), late-phase trials, and real-world data (RWD) studies. These models handle distributed data and complex regulations by keeping data local.
- Federated: The preferred choice for public health surveillance and complex international collaborations, enabling analysis across health systems while maintaining privacy.
Key Decision Factors
When you compare solutions for centralized vs decentralized data governance in clinical research, consider these factors:
- Organizational Culture & Maturity: A ‘mature’ data organization exhibits several key traits: strong data literacy across teams, established data stewardship roles, and a culture that treats data as a strategic asset, not an IT byproduct. Immature organizations often struggle with basic data quality and lack clear ownership, making a centralized model a necessary first step to establish control. Top-down cultures may start with centralized models, while larger, more autonomous organizations can more easily adopt federated approaches. A gradual transition, starting with a hybrid model, is often the most practical path.
- Regulatory Landscape: The global nature of clinical research makes this a paramount concern. Consider a trial running in the EU, the US, and China. The EU’s GDPR has strict data transfer restrictions. The US has HIPAA for health data, plus state-level laws like the California Consumer Privacy Act (CCPA). China’s Personal Information Protection Law (PIPL) has even stricter data localization requirements. A centralized model requiring data to be moved to a single location (e.g., a US server) would be legally impossible. A federated model, where data remains within each legal jurisdiction while allowing for aggregate analysis, is often the only viable path forward.
- Research Complexity & Technology: Simple studies may fit centralized models, but complex, multi-modal research requires the flexibility of federated models and a modern tech stack.
- Budget: Consider both upfront investment and long-term ROI, including the cost of delays vs. the cost of new platforms.
The Role of Supporting Tools and Platforms
Effective governance requires the right tools, regardless of the model:
- Data Catalogs & Metadata Management: In a federated system, a data catalog acts as a ‘Google for data,’ allowing researchers to find relevant datasets across the entire ecosystem. A good catalog for clinical research will not only index tables and files but also provide rich context: the study protocol it belongs to, the patient cohort characteristics, data lineage (how it was created and transformed), and quality metrics. This prevents data swamps and makes data truly findable, accessible, interoperable, and reusable (FAIR).
- Data Quality Frameworks: To define, measure, and automate data quality checks, especially in distributed environments. These tools can profile data, identify anomalies, and provide dashboards to monitor quality over time, ensuring that data ‘products’ are trustworthy.
- Access Control Platforms: To secure data using mechanisms like attribute-based access control (ABAC) and Zero Trust. These platforms manage permissions based on user roles, project affiliations, and data sensitivity, ensuring that only authorized individuals can access specific data for approved purposes.
- Trusted Research Environments (TREs): Also known as Secure Data Environments, TREs are more than just secure servers. They are highly controlled digital workspaces that provide researchers with access to analytical tools (like R, Python, SAS) next to the sensitive data, but prevent the data itself from being downloaded or moved. All activity is logged and audited. This ‘code-to-data’ approach is the cornerstone of modern federated analysis, enabling secure collaboration without compromising patient privacy, and is a core component of platforms like Lifebit’s.
Conclusion: Building a Future-Ready Data Governance Strategy
When you compare solutions for centralized vs decentralized data governance in clinical research, it’s clear there’s no single best answer—only different trade-offs. The centralized fortress offers control but creates bottlenecks, while the decentralized frontier offers speed but risks chaos. Neither extreme is sufficient for modern clinical research.
Context is king. The right model depends on your trial’s scale, your organization’s culture, and the regulatory landscape across regions like Europe, the USA, and Canada. The unmistakable trend is toward federated models that balance control with agility. They allow data to remain secure and local while enabling powerful, collaborative AI-driven research.
This balance is the ultimate goal: providing strategic oversight while empowering researchers to innovate. At Lifebit, our platform is built for this federated future. Our Trusted Research Environment (TRE), Trusted Data Lakehouse (TDL), and R.E.A.L. (Real-time Evidence & Analytics Layer) enable secure, compliant collaboration across distributed data. We help biopharma, governments, and research institutions get real-time insights from sensitive patient data without centralizing it.
The future of clinical research requires an adaptable strategy that evolves with your needs. It’s about empowering your teams, protecting patients, and accelerating findy without compromise.
Ready to build a future-ready data governance strategy? Find how to implement a federated data strategy and open up the full potential of your clinical research data.

