The Big List of Agencies and Government Health Initiatives Changing Lives

Government Health Initiatives: How to Access Free Care and $50B in Funding
Government health initiatives are large-scale programs run by federal, state, and international agencies to improve public health, reduce disease, and increase access to care. They target everything from maternal mental health and HIV treatment to rural healthcare transformation and digital health data sharing.
Key Government Health Initiatives at a Glance:
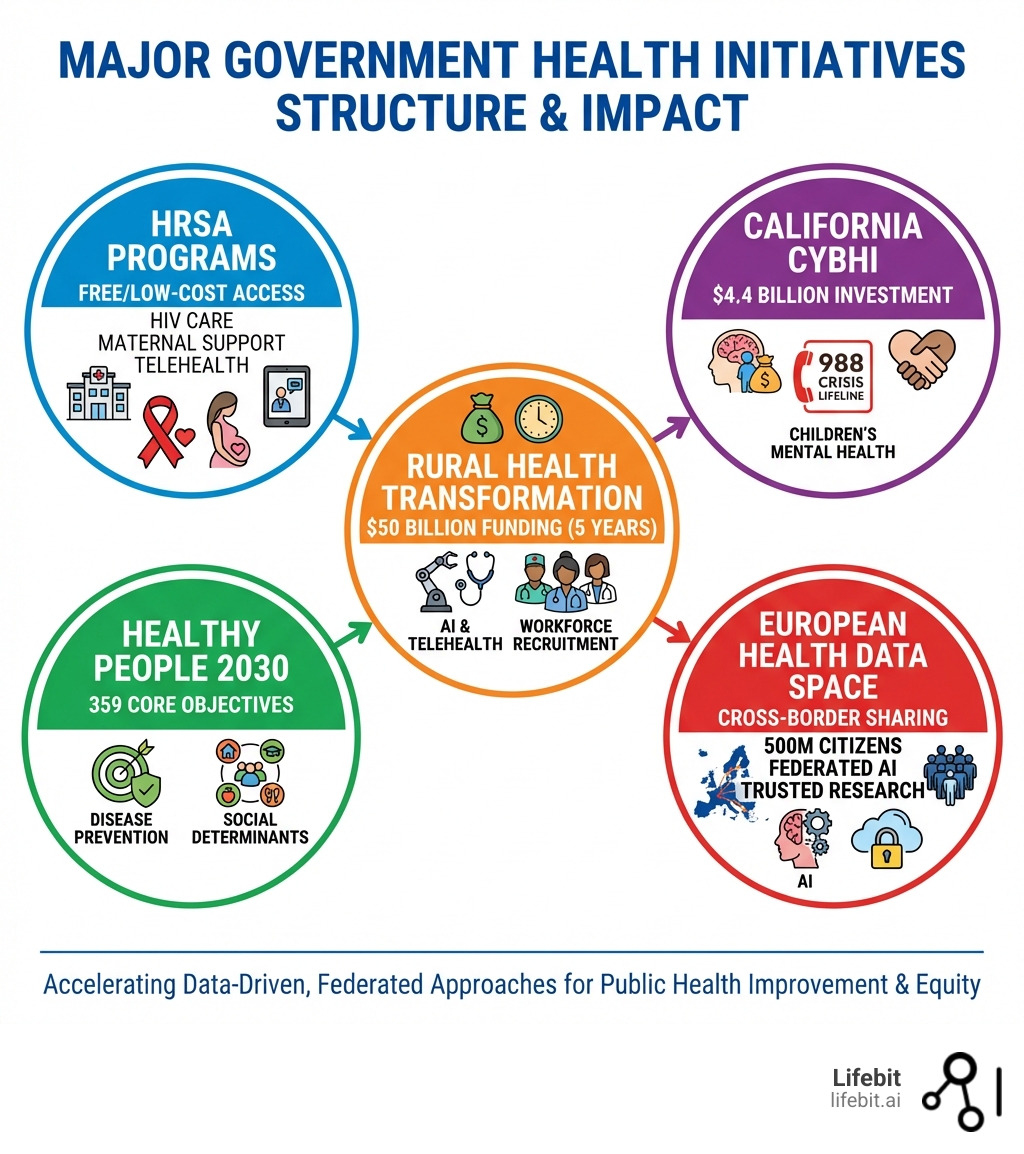
- HRSA Programs – Free or low-cost health centers, HIV care, maternal support, and telehealth access
- Healthy People 2030 – 359 measurable national health objectives focused on disease prevention and social determinants of health
- Rural Health Transformation (RHT) – $50 billion over five years to modernize rural healthcare with AI, telehealth, and workforce recruitment
- California CYBHI – $4.4 billion investment in children’s mental health and the 988 crisis lifeline
- European Health Data Space (EHDS) – Cross-border health data sharing for 500 million EU citizens using federated AI and secure environments
These initiatives address urgent gaps in healthcare access, especially for underserved populations. For example, the Ryan White HIV/AIDS Program serves over half a million people with a 91% viral suppression rate. The National Maternal Mental Health Hotline provides 24/7 confidential support via call, text, or chat. And the Rural Health Transformation Program is deploying $10 billion annually to bring AI-enabled diagnostics and remote monitoring to rural clinics.
The shift toward data-driven, federated approaches is accelerating. From EHDS creating secure processing environments for real-world evidence to Healthy People 2030 tracking health disparities with precision, these programs rely on interoperable data, AI, and cloud infrastructure to scale impact.
I’m Maria Chatzou Dunford, CEO and Co-founder of Lifebit, where we build federated data platforms that power government health initiatives across public sector institutions, enabling secure, compliant analysis of genomic and biomedical data at scale. My background in computational biology, AI, and health-tech entrepreneurship has positioned me at the intersection of precision medicine and public health transformation.
Must-know government health initiatives terms:
Stop Overpaying: Get Free Medical Care via HRSA Programs
The Health Resources and Services Administration (HRSA) is the primary federal agency for improving access to healthcare services for people who are uninsured, isolated, or medically vulnerable. Their government health initiatives are designed to bridge the gap between high-quality care and the ability to pay, ensuring that geography or financial status does not dictate the quality of care a person receives. HRSA oversees a massive network of programs that support more than 30 million people across the United States.
One of the most effective ways to access care is through Health Centers. These HRSA-funded clinics, often referred to as Federally Qualified Health Centers (FQHCs), operate in cities, rural areas, and everywhere in between across all U.S. states and territories. These centers are unique because they provide comprehensive primary care, including dental, mental health, and pharmacy services, on a sliding fee scale based on the patient’s income. If you are looking for a provider, you can Find a health center that provides primary and preventive care regardless of your insurance status. These centers are governed by community boards, ensuring that the services offered are directly tailored to the specific needs of the local population.
Life-Saving Support: Ryan White HIV/AIDS Program
The Ryan White HIV/AIDS Program is a cornerstone of American public health and a model for integrated chronic disease management. It provides care, treatment, and support services to more than half a million people with diagnosed HIV, reaching approximately 50% of all people living with HIV in the U.S. Recent data highlights the program’s incredible success, showing a 91% viral suppression rate among its patients. This is a monumental achievement in public health; when a person’s viral load is suppressed to undetectable levels, they can lead long, healthy lives while virtually eliminating the risk of transmitting the virus to others (U=U). The program is divided into several “Parts” (A through F), which fund everything from emergency relief in metropolitan areas to specialized care for women, infants, and children. To get started, patients can Find HIV care at a HRSA-funded clinic for free or low-cost treatment.
Beyond direct care, HRSA also focuses on the Health Workforce and Rural Health Policy. By offering Scholarships and Loan Repayment through the National Health Service Corps, the government incentivizes doctors, dentists, and behavioral health professionals to work in underserved communities. These Public Sector Initiatives ensure that even the most remote areas have access to qualified professionals, addressing the chronic provider shortages that plague rural America.
Maternal and Child Health Support
No parent should have to struggle alone. HRSA’s Maternal & Child Health programs offer a safety net for new and expecting families, focusing on reducing infant mortality and improving maternal health outcomes. A critical resource is the National Maternal Mental Health Hotline, which provides 24/7, free, and confidential support in English and Spanish. This service is staffed by culturally competent counselors who understand the unique pressures of pregnancy and early parenthood.
Whether you are dealing with postpartum depression, anxiety, or the overwhelming stress of a new baby, you can Web Chat with 1-833-TLC-MAMA or call/text the hotline at 1-833-852-6262. Other essential maternal government health initiatives include:
- Healthy Start: This program works in communities with infant mortality rates at least 1.5 times the national average. Find a local Healthy Start site to get community-based support, including prenatal care coordination and parenting education.
- Home Visiting (MIECHV): The Maternal, Infant, and Early Childhood Home Visiting Program supports pregnant women and parents with young children who live in communities at risk for poor maternal and child health outcomes. Find local home visiting programs where trained professionals visit your home to provide health guidance, screenings, and support for children’s development and school readiness.
Fix Health Disparities: 359 Goals from Healthy People 2030
If you’ve ever wondered how the U.S. government decides which health issues to prioritize, the answer is Healthy People 2030. Managed by the Office of Disease Prevention and Health Promotion (ODPHP), this initiative sets the nation’s health agenda every ten years. This tradition began in 1979 with the Surgeon General’s Report on Health Promotion and Disease Prevention, and it has evolved into a sophisticated, data-driven framework that guides federal, state, and local health policy.
Healthy People 2030 includes 359 core objectives—measurable goals that track everything from physical activity levels and tobacco use to cancer screening rates and vaccination coverage. As a premier Federal Health initiative, it uses a rigorous methodology to identify where the nation is succeeding and where we are falling behind. Each objective has a baseline, a target, and a data source, allowing for transparent tracking of progress over the decade.

One of the top priorities for 2030 is Health Literacy. The ODPHP has updated its definition of health literacy to include both personal health literacy (how well individuals can find and use information) and organizational health literacy (how well organizations equitably enable individuals to find and use information). The initiative provides tools to help health professionals communicate more clearly, ensuring that patients actually understand their diagnoses and treatment plans. This is a vital part of Federal Health Guide strategies to empower individuals to take charge of their own well-being and reduce medical errors caused by miscommunication.
Targeting Social Determinants of Health (SDOH)
We know that health isn’t just about what happens in a doctor’s office. Research suggests that clinical care accounts for only about 20% of health outcomes, while the remaining 80% is driven by where people live, learn, work, and play. These are known as Social Determinants of Health (SDOH). Healthy People 2030 places a massive emphasis on Reading about social determinants of health to reduce health disparities. The framework categorizes SDOH into five key domains:
- Economic Stability: Focusing on poverty, employment, and food security.
- Education Access and Quality: Tracking high school graduation rates and enrollment in higher education.
- Health Care Access and Quality: Measuring insurance coverage and access to primary care.
- Neighborhood and Built Environment: Addressing housing quality, rates of violence, and air/water quality.
- Social and Community Context: Looking at social cohesion and support systems.
To drive action, the initiative uses Leading Health Indicators (LHIs)—a small subset of high-priority objectives that are particularly important for improving health and well-being. These track critical factors like infant deaths, drug overdose deaths, and exposure to secondhand smoke. By focusing on these root causes, agencies like the NCI and the National Institute of Health can better target funding to communities with the greatest need, moving beyond treating symptoms to addressing the fundamental causes of illness.
Modernize Rural Clinics: How the $50B RHT Program Uses AI
For millions of Americans in rural areas, getting to a specialist can mean a four-hour drive or a day-long journey. The Rural Health Transformation (RHT) Program aims to fix this with a massive $50 billion investment over five fiscal years (2026-2030). This initiative represents one of the most significant federal commitments to rural infrastructure in decades, recognizing that the traditional fee-for-service model often fails in low-volume rural settings.
This program, overseen by the Centers for Medicare & Medicaid Services (CMS), allocates $10 billion annually to help states “rightsize” their rural health systems. The funding is split: 50% is distributed equally among approved states to ensure a baseline of support, and 50% is formula-based, using rural factors such as population density and poverty rates to ensure the money goes where it’s needed most. These Federal Health Tips 2025 highlight that states must choose at least three approved uses for the funds, such as workforce recruitment, chronic disease interventions, or the conversion of struggling facilities into the new “Rural Emergency Hospital” (REH) designation, which focuses on outpatient and emergency care rather than inpatient beds.
Modernizing Rural Government Health Initiatives with AI
The RHT Program isn’t just about keeping the lights on in small hospitals; it’s about a fundamental technological modernization. The initiative explicitly authorizes the use of funds for cutting-edge technologies that can bridge the distance gap:
- AI and Robotics: Enhancing diagnostics and surgical precision in remote areas. For example, AI-powered imaging can help a general practitioner in a rural clinic identify signs of a stroke or specific cancers as accurately as a specialist in a major medical center.
- Telehealth and Remote Monitoring: Expanding the digital reach of healthcare. This includes funding for wearable devices that allow doctors to monitor chronic conditions like diabetes and heart disease in real-time, reducing the need for frequent in-person visits.
- IT Infrastructure and Interoperability: Building the digital backbone needed for Solutions for Government to work effectively across state lines. This includes high-speed broadband for clinics and secure cloud storage for patient records.
By adopting alternative payment models (APMs) and value-based care, the RHT Program ensures that rural providers are rewarded for patient outcomes rather than just the number of tests performed. This shift is crucial for the sustainability of rural healthcare, as it allows providers to focus on preventive care and community health initiatives that keep people out of the hospital in the first place.
Stop the Crisis: California’s $4.4B Plan for Instant Mental Health Support
While federal programs provide the framework, states often lead the way with bold government health initiatives that serve as laboratories for national policy. California is currently undergoing a “Mental Health Revolution” with a $4.4 billion investment in the Children and Youth Behavioral Health Initiative (CYBHI). This initiative is part of a broader effort to transform California’s behavioral health system into a more integrated, equitable, and prevention-oriented ecosystem.
The Learn More about CYBHI portal explains that the goal is to reimagine mental health for all children and youth by delivering services where they are—in schools, primary care offices, and community centers. This includes the 988 Suicide and Crisis Lifeline, an easy-to-remember number for anyone experiencing a mental health or substance use crisis. This service is a lifeline for many, including those supported by Veterans Affairs, providing immediate access to trained crisis counselors who can dispatch mobile crisis teams if necessary.
How California Leads State-Level Government Health Initiatives
California’s approach is “upstream,” meaning they want to catch problems before they lead to homelessness, hospitalization, or incarceration. This involves a multi-pronged strategy that includes:
- The CARE Act: The Community Assistance, Recovery, and Empowerment (CARE) Act creates a new pathway for delivering mental health and housing services to individuals with untreated schizophrenia or other psychotic disorders. It allows family members, first responders, and others to petition a court to develop a CARE plan for an individual in need.
- BenefitsCal: A simple, unified way for residents to Apply now for BenefitsCal to access food (CalFresh), cash assistance (CalWORKs), and health coverage (Medi-Cal). By streamlining the application process, California ensures that social needs are met alongside medical needs.
- Data Exchange Framework (DxF): Mandated by AB 133, this framework requires healthcare entities, including hospitals and health plans, to share data securely and in real-time. This enables “whole-person care,” where a social worker, a primary care doctor, and a mental health specialist can all see the same patient record and coordinate treatment.
Agencies like the NHLBI and state departments are also watching California’s Master Plan for Aging closely. With the over-65 population expected to hit 8.6 million by 2030, the state is investing in “age-friendly” communities and expanding the healthcare workforce to meet the needs of an aging society. This includes the CalAIM (California Advancing and Innovating Medi-Cal) initiative, which integrates social services like housing navigation and medically tailored meals into the state’s Medicaid program.
Save €120B: How EHDS Shares Health Data Without Risking Privacy
Across the Atlantic, the European Health Data Space (EHDS) is setting a global gold standard for how government health initiatives handle digital data. The EHDS aims to create a single market for digital health services and products across the EU, potentially saving up to €120 billion over ten years through more efficient data use, reduced duplication of tests, and accelerated research.
The European Strategy for data outlines two main uses for this data, which are fundamental to the EHDS framework:
| Use Type | Description | Example |
|---|---|---|
| Primary Use | Direct patient care across borders. | MyHealth@EU allowing a doctor in Italy to see a French patient’s records in their own language during an emergency. |
| Secondary Use | Data for research, innovation, and policy-making. | Using pseudonymized records from millions of patients to train AI for rare disease diagnosis or to track the efficacy of a new vaccine. |
This framework is built on the foundation of GDPR (General Data Protection Regulation), ensuring that while data is shared, privacy is never compromised. The EHDS introduces the concept of “Data Altruism,” where citizens can voluntarily permit the use of their data for the public good, such as for medical research. For those in the defense sector, the Defense Health Data Platform Guide provides similar insights into secure data management in high-stakes environments.
Federated Learning and Secure Data Access
The EHDS doesn’t require moving massive amounts of sensitive data into a single central database, which would create a massive security risk. Instead, it utilizes Federated Learning and Trusted Research Environments (TREs). This is a “data-to-code” approach rather than a “code-to-data” approach. It allows researchers to “visit” the data where it lives (like a university hospital or a national health registry), run their analysis algorithms, and take only the aggregated insights away—never the raw patient data.
This decentralized model is essential for maintaining public trust. By using techniques like pseudonymization and differential privacy, the Federated Data Ecosystem NIAID and EHDS participants can link data for real-world evidence without revealing individual identities. This is the future of Defense Health Agency and global health research, enabling large-scale studies on rare diseases that were previously impossible due to data being siloed in different countries. The EHDS also establishes a “Health Data Access Body” in each member state to oversee requests for data, ensuring that only legitimate researchers with ethical approval can access the information.
Find Free Care Near You: Government Health Initiatives FAQ
How do I find free health services near me?
You can use the HRSA Find a Health Center tool. These centers provide care regardless of your ability to pay and are located in every U.S. state and territory. They offer primary care, dental, and mental health services. For HIV-specific care, visit ryanwhite.hrsa.gov to find a provider that offers specialized treatment and support services.
What is the goal of Healthy People 2030?
The goal is to provide a 10-year roadmap for improving the nation’s health. It focuses on 359 core objectives, with a heavy emphasis on reducing health disparities and addressing the social determinants of health, such as housing, education, and economic stability. It serves as a guide for federal funding and state-level health planning.
Who is eligible for the Rural Health Transformation Program?
The RHT Program is primarily a state-level funding initiative. Only the 50 U.S. states are eligible to apply for the $50 billion in funding. Individual hospitals and clinics in rural areas access these funds through their state’s approved RHT plan. To be eligible, facilities usually must be located in a HRSA-designated rural area.
What is the 988 Suicide and Crisis Lifeline?
The 988 Lifeline is a national network of local crisis centers that provides free and confidential emotional support to people in suicidal crisis or emotional distress 24 hours a day, 7 days a week in the United States. It is a key component of both federal and state-level mental health initiatives, including California’s CYBHI.
How does the European Health Data Space protect my privacy?
The EHDS uses a “federated” approach, meaning your data stays at its original location (like your local hospital). Researchers are allowed to run analysis on the data through secure “Trusted Research Environments,” but they cannot see your name or identity, and they cannot take the raw data out of the secure system. It is fully compliant with GDPR.
Secure Your Data: Powering Government Health Initiatives with Lifebit
From the local health centers funded by HRSA to the massive digital infrastructure of the European Health Data Space, government health initiatives are the invisible backbone of global well-being. They provide the funding, the data standards, and the crisis support that keep our communities healthy.
At Lifebit, we believe that the next frontier of these initiatives lies in the secure, federated access to data. Our Lifebit Trusted Research Environment is designed to help governments and researchers collaborate on multi-omic and biomedical data without ever moving it, ensuring total compliance with regulations like GDPR and FedRAMP.
Whether it’s accelerating the NIA Data Access Program or supporting the Common Fund, our mission is to make global health data usable for everyone, everywhere.

