Top EHR Vendors Ranked: Which Software Wins the Popularity Contest?
Best Electronic Medical Record Software: Reclaim 22 Hours of Physician Time Weekly
The best electronic medical record software isn’t just about digitizing patient charts anymore—it’s about reclaiming physician time, cutting operational costs, and unlocking clinical insights buried in siloed data. In the modern healthcare landscape, the EMR has evolved from a simple digital filing cabinet into a sophisticated clinical operating system. As we move into 2026, the focus has shifted from mere data entry to data utility, where the software actively assists the provider in decision-making and administrative reduction.
| Vendor | Best For | Starting Price | Key Strength |
|---|---|---|---|
| Epic Systems | Large health systems & academic centers | Custom quote | Interoperability & patient portal |
| Athenahealth | Medium to large outpatient clinics | $140/user/month | Revenue cycle management |
| Oracle Health (Cerner) | Global enterprises & government | Custom quote | Scalability & population health |
| NextGen Healthcare | Ambulatory & specialty practices | Custom quote | Comprehensive solution |
| Meditech | Community & regional hospitals | Custom quote | Inpatient & lab integration |
| DrChrono | Small practices & mobile users | ~$274/month | Mobile accessibility |
| Practice Fusion | Solo providers & small clinics | Custom quote | Ease of use & onboarding |
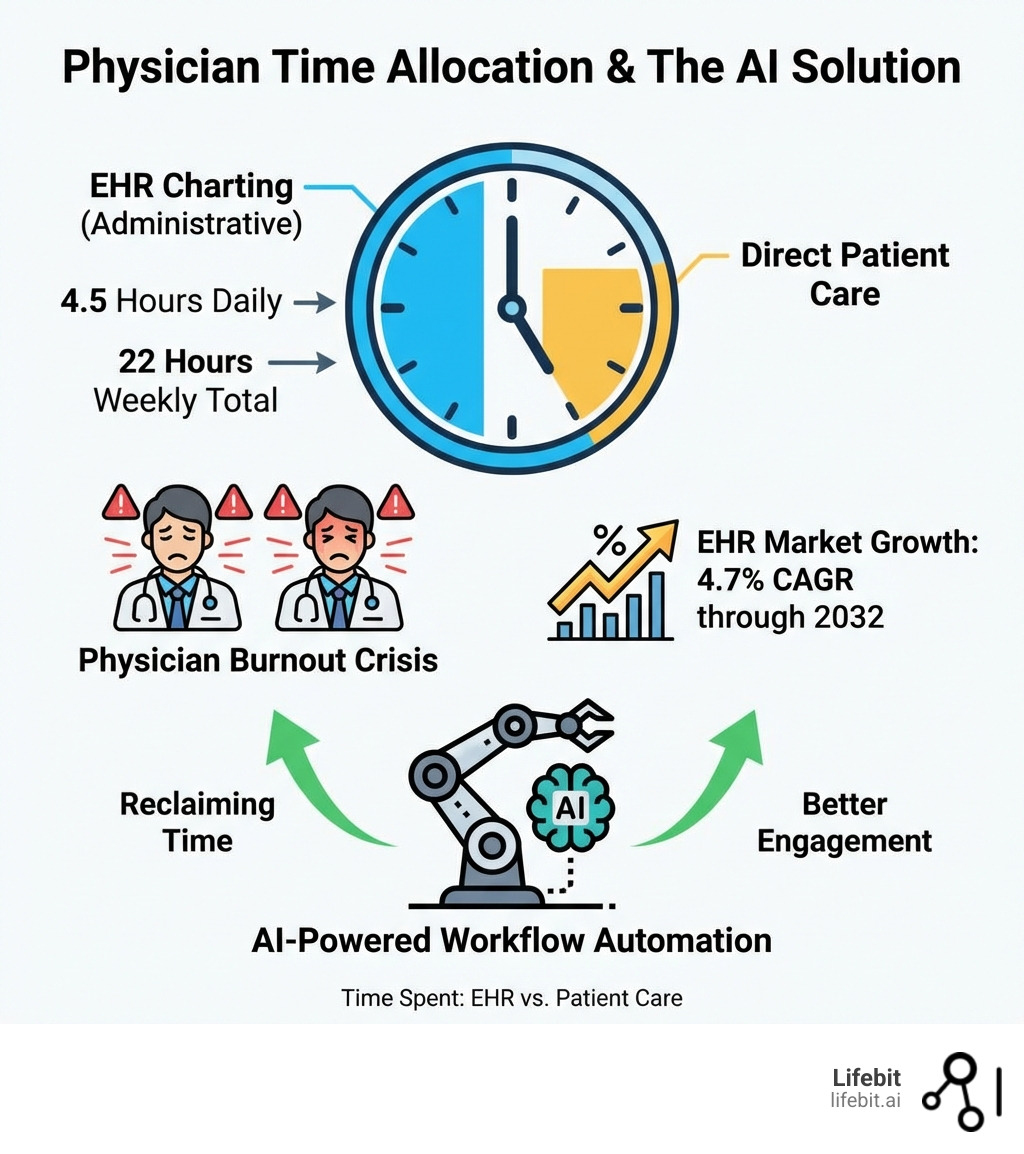
Physicians spend 4.5 hours daily—roughly 22 hours per week—completing electronic health records. That’s nearly twice as much time on EHRs as with patients. This phenomenon, often referred to as “pajama time,” is a leading cause of clinician burnout and professional dissatisfaction. Meanwhile, the EHR market is growing at 4.7% annually through 2032, yet 70% of clinicians report better patient engagement only when AI-powered workflows reduce their charting burden. The industry is at a tipping point where the software must either adapt to the physician’s workflow or continue to be a barrier to care.
The real question isn’t which system to choose. It’s whether your current EHR strategy is costing you millions in lost productivity, missed shared savings opportunities, and physician burnout. A poorly implemented system can lead to “click fatigue,” where a single prescription requires dozens of manual interactions, increasing the risk of medical errors and reducing the number of patients a provider can see in a day.
I’m Maria Chatzou Dunford, CEO and Co-founder of Lifebit, where we’ve spent over 15 years building federated AI platforms that help organizations extract real-time insights from fragmented EHR, claims, and genomics data—without moving it. This guide breaks down how the best electronic medical record software can transform your clinical operations, backed by real-world outcomes like $33.8 million in ACO shared savings and 88,000 staff hours saved through smarter data workflows. We will explore the technical nuances, the financial implications, and the future of AI-driven clinical documentation.
Best electronic medical record software terms simplified:
EMR vs. EHR: Why the Difference Matters for Your Bottom Line
When searching for the best electronic medical record software, you will likely see the terms EMR and EHR used interchangeably. However, for a growing healthcare organization, the distinction is critical for long-term scalability and regulatory compliance.
An Electronic Medical Record (EMR) is a digital version of a patient’s paper chart within one practice. It is excellent for diagnosis and treatment within that specific silo but often lacks the “portability” needed for modern, coordinated care. EMRs were the first step in the digital revolution, replacing the physical folders that used to line the walls of doctor’s offices. While they improved legibility and internal tracking, they did little to solve the problem of fragmented care when a patient moved between a primary care doctor and a specialist.
In contrast, an Electronic Health Record (EHR) is designed to go beyond the individual clinic. It enables secure sharing of information across all healthcare providers involved in a patient’s care, such as labs, specialists, pharmacies, and emergency rooms. The EHR is a longitudinal record of patient health, containing data from all clinicians involved in the patient’s care. This holistic view is essential for managing chronic conditions and preventing adverse drug events caused by multiple providers prescribing conflicting medications.

Interoperability—the ability for these systems to “talk” to each other—is no longer a luxury; it is a regulatory requirement. The HITECH Act of 2009 and the subsequent Meaningful Use stages laid the groundwork, but the 21st Century Cures Act has pushed the industry toward “Information Blocking” rules that mandate data sharing. According to current HIPAA-compliant software requirements, platforms must now include end-to-end encryption, strict access controls, and secure data transmission protocols. Furthermore, recent HIPAA updates require annual compliance audits and enhanced cybersecurity measures to protect electronic protected health information (ePHI) against the rising threat of ransomware.
For organizations looking to scale, choosing a HIPAA compliant EMR that can transition into a full EHR ecosystem is vital. This transition ensures that as your practice grows or joins a larger health network, your data remains liquid and usable for advanced analytics, population health management, and value-based care reporting.
Best Electronic Medical Record Software: Top Vendors for 2026
Selecting the right vendor requires balancing functionality, usability, and cost. According to ambulatory EHR ranking research, vendors like athenahealth and Epic lead the market in broad suite performance, but “best” is subjective to your practice size and clinical specialty.
Scaling the Best Electronic Medical Record Software for Large Enterprises
For hospital systems and integrated networks, the software must handle immense data loads, complex specialty workflows, and thousands of concurrent users. These systems often serve as the “single source of truth” for an entire region.
- Epic Systems: Widely considered the gold standard for large academic medical centers and multi-state health systems. Epic’s “One Patient, One Record” philosophy and its robust MyChart patient portal have made it a favorite for organizations prioritizing patient engagement and seamless internal interoperability. However, its high implementation cost and steep learning curve can be prohibitive for smaller entities.
- Oracle Health (formerly Cerner): A powerhouse in the global market and government sectors (including the VA). Oracle Health excels in large-scale data management and population health analytics. Since the Oracle acquisition, there has been a significant push toward integrating cloud-based AI and voice-recognition features directly into the clinical workflow.
- Meditech Expanse: A robust Meditech solution designed for hospitals that need strong inpatient support and seamless integration with labs and imaging. It is often preferred by community and regional health systems for its EHR ecosystem, offering a more cost-effective alternative to Epic while maintaining high levels of integration.
- NextGen Healthcare: A versatile electronic health records program that scales across large ambulatory groups, offering deep customization for specialty-specific workflows, particularly in behavioral health, ophthalmology, and orthopedics.
Why Small Clinics Need the Best Electronic Medical Record Software
Small practices and solo providers have different priorities: they need fast onboarding, low upfront costs, and mobile access to manage their practice without a dedicated IT department.
- Athenahealth: Often cited as the athenahealth solution of choice for independent practices, it excels in revenue cycle management (RCM) and payer connections. Its cloud-native architecture means updates are automatic, and its “athenaNet” network allows providers to see clinical data from other practices using the system. It starts at roughly $140/user/month, making it accessible for growing clinics.
- DrChrono: The “Best Mobile EHR” for 2025-2026, DrChrono is built for iPad and iPhone use, allowing physicians to chart on the go. It offers a 30-day free trial and innovative workflows that take over administrative tasks like patient check-in and automated billing. It is particularly popular among concierge medicine and mobile health providers.
- Practice Fusion: A web-based platform that is exceptionally easy to use. It is a popular choice for small physician practices that need basic billing and charting without the “click-heavy” burden of enterprise software. While it lacks some of the deep analytics of Epic, its simplicity allows doctors to focus more on the patient and less on the screen.
- Elation Health: Specifically designed for primary care, Elation focuses on a “clinical first” philosophy. It minimizes the number of clicks required to document a visit, making it a top choice for Direct Primary Care (DPC) models where physician-patient time is the primary value proposition.
Evaluating best electronic medical records companies means looking past the feature list and assessing whether the software acts as a “partner” that supports your specific workflow rather than a digital obstacle.
AI and Automation: Reclaiming 4.5 Hours of Daily Physician Time
The most significant trend in the best electronic medical record software for 2026 is the integration of AI. We are seeing a shift from simple “record keeping” to “intelligent assistance.” This is not just about chatbots; it is about deep integration of Natural Language Processing (NLP) and Machine Learning (ML) into the core clinical experience.
Modern electronic medical record systems are now incorporating:
- Ambient Scribing: AI tools like Nuance DAX or Abridge listen to patient encounters and draft clinical notes in real-time. These tools can distinguish between casual conversation and clinical findings, automatically populating the subjective and objective portions of a SOAP note. This eliminates the “pajama time” doctors spend charting at home after clinic hours.
- Adaptive Learning: Systems like Praxis EMR use AI that learns a provider’s unique charting style, becoming faster and more personalized over time rather than relying on rigid, one-size-fits-all templates. This reduces the cognitive load on the physician, as the system anticipates their next move based on historical patterns.
- Predictive Analytics: Tools that flag high-risk patients for conditions like maternal cardiovascular disease, sepsis, or chronic kidney disease before they become critical. By analyzing thousands of data points in the background, the EHR can provide “nudge” alerts to clinicians, suggesting screenings or interventions that might otherwise be missed.
- Automated Coding and Billing: AI can now suggest ICD-10 and CPT codes based on the clinical documentation, reducing the back-and-forth between the clinical staff and the billing department. This ensures that the practice is reimbursed accurately for the complexity of the care provided.
Research from ICD10 AI-powered systems shows that 70% of clinicians report better focus and engagement with their patients when AI handles the documentation. By automating ICD-10 coding and medication suggestions, these tools help reclaim those 4.5 hours lost daily to administrative tasks. Furthermore, AI-driven clinical decision support (CDS) is moving from “alert fatigue” to “contextual intelligence,” where alerts only fire when they are truly relevant to the specific patient’s genetic profile and medical history.
Implementation and Cost: Avoiding the $9,000 Monthly Trap
Pricing for the best electronic medical record software is notoriously opaque and can vary significantly based on the delivery model (SaaS vs. On-premise). While entry-level plans might average $274 per month, sophisticated enterprise systems can cost up to $9,000 per month depending on the number of users, patient panel size, and the level of support required.
When assessing the Total Cost of Ownership (TCO), we recommend looking for these often-overlooked expenses:
- Implementation Fees: These can range from a few thousand dollars for a cloud-based system to millions for hospital-wide deployments. This includes the cost of project managers, technical consultants, and the “productivity dip” that occurs during the first few months of use.
- Data Migration: Moving legacy data from an old system into a new one is a complex technical challenge. If the data is not mapped correctly, you risk losing historical patient records or creating duplicate entries that compromise patient safety.
- Training and Support: Inadequate training is the number one reason for EMR implementation failure. Organizations must budget for initial training and ongoing education as new features are released. High-quality support, available 24/7, is essential for critical care environments.
- Hardware Upgrades: Many modern EHRs require high-speed internet, tablets, or specific server configurations. If your current infrastructure is outdated, the “software” cost is only the tip of the iceberg.
According to a comprehensive EMR software guide, buyers who take longer than five months to evaluate software often suffer from “buyer’s remorse.” Successful practices typically determine their choice in under four months by focusing on core needs rather than a “feature-heavy” but unusable platform. To ensure a smooth transition, we recommend a phased approach: Discovery, Design, Build, Test, and Go-Live. For a deeper dive into the lifecycle of these systems, see our EHRs complete guide.
Interoperability and Billing: The Secret to $33M in Shared Savings
The true power of the best electronic medical record software is realized when clinical data meets financial outcomes. In the era of Value-Based Care (VBC), the goal is no longer just to see more patients, but to achieve better outcomes at a lower cost. This relies on the seamless exchange of data between providers, payers, and patients.
A prime example is the Novant Health ACO, which used clinical decision support and analytics within their EHR to generate $33.8 million in shared savings and achieve a quality score of 94.52%. This success was driven by using data to close care gaps—such as breast and colorectal cancer screenings—which not only improves patient outcomes but also significantly boosts revenue through performance-based incentives.
To achieve this level of financial and clinical success, organizations must move away from legacy EHR warehouses to FHIR (Fast Healthcare Interoperability Resources) standards. FHIR allows for modern API-led connectivity, enabling different software applications to exchange data in real-time. This is the foundation for EHR claims integration, ensuring that every clinical action is captured, coded, and billed accurately without manual intervention.
Furthermore, interoperability allows for the integration of Social Determinants of Health (SDOH) data. By understanding a patient’s housing status, transportation access, and food security through the EHR, providers can tailor their care plans to be more effective, reducing readmission rates and improving the overall health of the population. This data-driven approach is what separates the “best” software from the rest of the market.
Frequently Asked Questions about EMR Software
What is the difference between EMR and EHR?
An EMR is a digital version of a patient’s chart within a single practice, primarily used for diagnosis and treatment. An EHR is a more comprehensive, longitudinal record designed to be shared securely across different healthcare organizations, including specialists, labs, and pharmacies, to provide a holistic view of patient health.
Which EMR software is best for small practices?
Athenahealth, DrChrono, and Practice Fusion are consistently ranked as the best options for small practices. They offer lower upfront costs, cloud-based accessibility (which eliminates the need for local servers), and user-friendly interfaces that require less intensive training than enterprise systems like Epic.
How much does the best electronic medical record software cost?
Costs vary based on the size of the practice and the features required. Small practices might pay $140 to $300 per user per month for a SaaS model. Large enterprise systems typically require custom quotes that include significant implementation, data migration, and maintenance fees, which can reach thousands of dollars monthly.
Is cloud-based EMR better than on-premise?
For most modern practices, cloud-based (SaaS) EMRs are superior because they offer automatic updates, lower hardware costs, and better remote access. On-premise systems are generally only preferred by very large institutions with massive IT departments that require total control over their data servers for specific security or legacy reasons.
How does EMR software improve patient safety?
EMR software improves safety by providing automated alerts for drug-drug interactions, ensuring legibility of prescriptions, and providing a complete history of a patient’s allergies and past procedures. It also reduces the risk of lost or misplaced paper files, ensuring that critical information is available when needed most.
What is FHIR and why does it matter for my EMR?
FHIR (Fast Healthcare Interoperability Resources) is the modern standard for exchanging healthcare information electronically. It matters because it allows your EMR to easily connect with other apps, such as patient portals, billing software, and advanced AI analytics tools, ensuring your data is not trapped in a single system.
Conclusion: Beyond the Chart with Lifebit
Choosing the best electronic medical record software is the first step toward a data-driven future. However, for many organizations, the data remains trapped within these systems, making large-scale research or pharmacovigilance difficult.
At Lifebit, we take the next step. Our federated AI platform enables secure, real-time access to global biomedical and multi-omic data without moving it from its original location. By providing a Trusted Research Environment (TRE) and a Trusted Data Lakehouse (TDL), we help biopharma and public health agencies harmonize disparate EHR records and run advanced AI/ML analytics.
Whether you are looking to improve daily clinic workflows or power global health research, the goal is the same: making medical data work for the patient. Explore the Lifebit platform today to see how we turn fragmented records into life-saving insights.

